Hyperpigmentation treatment UK
Hyperpigmentation & Melasma Treatment UK — Doctor-Led Care for Dark Marks, Uneven Tone and Pigmentation
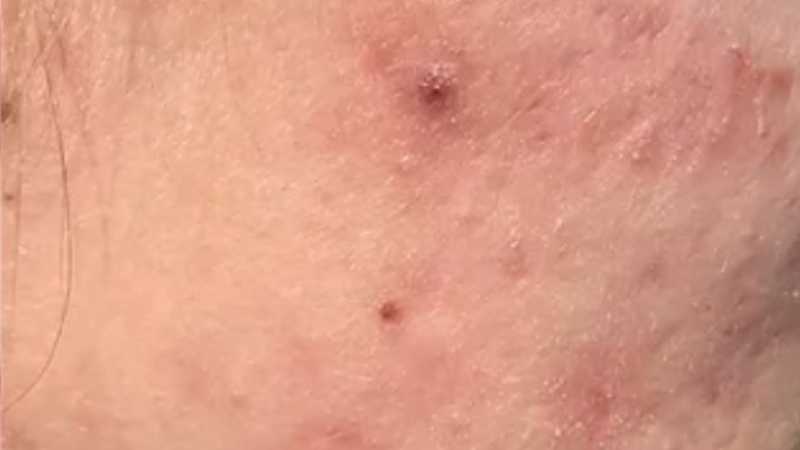
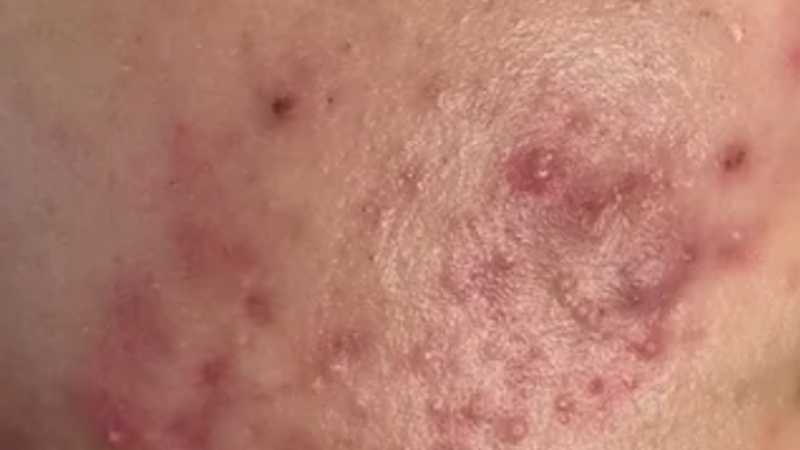
Hyperpigmentation can appear as brown patches, post-acne marks, sun-related pigmentation, melasma, uneven tone or stubborn areas of discolouration that do not fade as expected.
At The Women’s Health Clinic, we treat pigmentation carefully because the wrong approach can make marks darker, irritate the skin barrier or trigger rebound pigmentation. Your consultation focuses on identifying the type of pigmentation, triggers, skin tone, hormonal context, previous treatments and safety factors.
The aim is to build a staged, pigment-safe plan — from skincare and prescription-led options where suitable, through to chemical peels, light-based treatments, laser or combination treatment when appropriate.
Common pigmentation patterns we assess
Pigmentation needs pattern recognition before treatment is chosen.
What may be discussed
Your plan may combine prevention, skincare, medical and clinic-based options.
Educational only. Not a diagnosis or medical advice. Suitability is confirmed after consultation and assessment. Results vary. Not a cure.

At a glance
Pigmentation care starts with understanding the cause, depth, triggers, skin tone, hormonal context, sun exposure, previous treatments and whether inflammation is still active.
Assessment-led
Pigment type, triggers and skin history reviewed
First step
clinical skin review
Approach
gentle and staged
Focus
tone, triggers + prevention
Timeline
usually measured in months
Especially relevant for women
Pregnancy, hormones, contraception, menopause and sun exposure may contribute
Trigger-led assessment
We look at sun exposure, inflammation, acne history, hormones, skincare irritation and previous treatment response.
Clear next-step plan
Your plan may include prevention, skincare, pigment actives, peels, laser review or maintenance where suitable.
What is hyperpigmentation?
Hyperpigmentation means areas of skin appear darker than the surrounding skin because of increased pigment. It may follow acne, inflammation, sun exposure, hormonal changes, pregnancy, medication changes or skin irritation.
Melasma is a specific type of facial pigmentation that often appears as symmetrical brown or grey-brown patches, commonly affecting the cheeks, forehead, upper lip or jawline. It can be stubborn and may relapse without maintenance and sun protection.
Post-inflammatory pigmentation
Dark marks can appear after acne, eczema, irritation, picking, burns or procedures. This is common in pigment-prone skin and needs a gentle, barrier-aware plan.
Melasma and hormonal pigmentation
Melasma may be influenced by hormones, pregnancy, contraception, HRT, heat, visible light and UV exposure. It often needs long-term maintenance, not just one treatment.
Sun spots and uneven tone
Sun-related pigmentation, age spots and uneven tone need careful diagnosis. Some lesions should be checked medically before cosmetic-style treatment.
The balanced way to think about pigmentation treatment
Good pigmentation care is rarely about stripping the skin or using the strongest peel. It is usually about reducing triggers, protecting the skin barrier, controlling inflammation, using pigment actives carefully, then considering procedures only when suitable.
Who is hyperpigmentation treatment for?
Hyperpigmentation treatment may suit people with stubborn dark marks, melasma, post-acne pigmentation, sun-related patches or uneven tone — especially where over-the-counter brightening products have not been enough.
Women with melasma or hormonal pigmentation
Melasma may appear during pregnancy, after hormonal changes, around contraception changes, with HRT, or during perimenopause. It often needs careful long-term management.
People with post-acne pigmentation
If spots leave brown marks, dark patches or uneven tone, the plan may need to control acne, reduce inflammation and treat pigmentation together.
People with sun-related pigmentation
Sun spots and uneven tone can worsen over time. Some pigmented lesions should be checked medically before cosmetic treatment is considered.
When pigmentation needs medical review
Sudden, changing, irregular, symptomatic or unusual pigmentation should be medically assessed before aesthetic-style treatment.
Melasma treatment — hormones, sun exposure and long-term control
Melasma can be frustrating because it may improve and then relapse, especially after sun exposure, heat, irritation or hormonal change. Treatment needs to be realistic and maintenance-focused.
What we look for
A careful history helps identify whether pigmentation is likely to be melasma, post-inflammatory pigmentation, sun-related pigmentation or another pattern needing medical review.
Hormonal context
Melasma may be influenced by pregnancy, contraception, HRT, perimenopause or other hormonal changes. These details matter before treatment.
UV, visible light and heat
Sunlight and heat can worsen pigmentation. Daily broad-spectrum protection and behaviour changes are often central to the plan.
Skin barrier and irritation
Over-exfoliation, harsh actives and aggressive peels can worsen pigmentation. The skin barrier must be respected.
Maintenance planning
Melasma often needs maintenance even after improvement. Stopping prevention and skincare can lead to relapse.
Why this matters
Treating pigmentation without identifying triggers can lead to repeated relapse. Equally, assuming every brown patch is melasma can miss post-inflammatory pigmentation, sun damage or lesions that need medical assessment. The consultation helps separate these strands.
How hyperpigmentation treatment works
The safest pigmentation plan is usually staged. We first identify the pigment pattern and triggers, then protect the skin, then introduce treatment carefully.
1. Pigmentation consultation
We review the pattern, duration, triggers, skincare, medication history, hormonal context, sun exposure and previous treatment response.
2. Prevention foundation
Daily broad-spectrum sun protection, heat awareness, visible-light protection and barrier support are often the foundation.
3. Active treatment
Treatment may include pigment-focused skincare, prescription-led options, peels, laser review or combination treatment where suitable.
4. Maintenance and relapse control
Pigmentation may relapse. Maintenance, review and careful adjustment are part of the plan.
Treatment methods we may use for pigmentation and melasma
Hyperpigmentation is the concern. The treatment method depends on the type of pigmentation, skin tone, trigger pattern, sensitivity, previous response and whether the issue is melasma, post-inflammatory pigmentation, sun-related pigmentation or something that needs medical review.
Prevention and SPF strategy
Daily broad-spectrum SPF, visible-light protection, heat awareness and behavioural changes are often essential.
Prescription-led skincare
Where appropriate, pigment actives may be considered with clinical guidance, safety counselling and review.
Chemical peels
Selected peels may support pigment improvement, but strength, timing, preparation and skin tone safety matter.
Laser and device review
Laser or light-based treatments may help selected pigmentation, but can worsen melasma if chosen or timed poorly.
Why a staged pathway matters
Pigmentation can worsen if the skin is irritated. It is usually better to stabilise the barrier and prevention first before introducing stronger actives or procedures.
Why we avoid one-size-fits-all packages
Melasma, post-acne pigmentation, sun spots and inflammatory marks may look similar to patients but need different levels of caution and different methods.
When referral may be needed
Pigmented lesions that are new, changing, irregular, symptomatic, bleeding or diagnostically uncertain should be medically assessed before cosmetic pigmentation treatment.
Aesthetic-style treatments should not be used to treat uncertain lesions or replace medical skin assessment.
For women with melasma linked to pregnancy, contraception, HRT, perimenopause or medication changes, pigmentation care may sit alongside wider women’s health assessment.
This is where WHC’s broader women’s health background can be especially useful.
Pigmentation results need honest context
Pigmentation improvement depends on the cause, skin tone, sun exposure, hormones, treatment consistency, aftercare and maintenance. Melasma can relapse, and no treatment outcome can be guaranteed.
Book Free ConsultationBefore & after
Images are shown for illustration and educational purposes only. Individual results vary, and no treatment outcome can be guaranteed. Suitability and expected results are discussed during consultation.
Why choose a structured pigmentation plan?
Pigmentation treatment works best when triggers, skin barrier, sun exposure, hormonal context, skin tone and maintenance are all considered together.
Protect before treating
Without daily protection and trigger control, pigmentation is more likely to persist or return.
Avoid irritation
Overuse of actives, harsh peels or aggressive devices can worsen pigmentation. A cautious approach is often safer.
Plan for maintenance
Pigmentation, especially melasma, often needs ongoing maintenance even after visible improvement.
More even-looking tone
The goal is to reduce the appearance of patchiness and uneven colour while protecting the skin barrier.
Reduced post-acne marks
Pigmentation after acne may improve when acne control, inflammation reduction and pigment treatment are planned together.
Confidence and wellbeing
Visible pigmentation can affect confidence and make people feel dependent on makeup or filters. It deserves practical and compassionate care.
Realistic timing
Pigmentation improvement often takes weeks to months, and maintenance is usually part of the long-term plan.
Benefits patients may be looking for
Patients usually want more than “brightening.” They want clearer guidance, fewer flare-ups, less patchiness, safer use of actives, and a plan that fits their skin tone and triggers.
Results vary. Suitability is always confirmed after consultation and assessment.
Hyperpigmentation treatment prices UK
Featured consultation price and full pricing guidance
Pigmentation treatment pricing depends on the route recommended after assessment. Some patients need skincare and prevention only. Others may need prescription-led treatment, peels, laser review, test patches, maintenance products or combination treatment. For the most complete and up-to-date information, please check our full pricing page.
Free initial enquiry
A short enquiry call to understand your concern and guide you towards the most appropriate appointment or pathway.
Initial enquiry call
Pigmentation consultation
A focused clinical review of pigmentation type, triggers, skin tone, hormonal context, previous treatments and possible treatment methods.
Featured starting price
Treatment pricing
Peels, laser, prescription-led skincare, test patches and maintenance treatments are priced according to the plan recommended.
Full price list
Why prices vary
Pigmentation is not treated with one fixed package. A patient with post-acne marks may need a different plan from someone with melasma, sun spots, irritation-led pigmentation or mixed pigmentation.
What may affect the final cost?
Check the full pricing page
We are building a central pricing page so patients can check treatment costs in one place. This pigmentation page gives the featured starting point, but the full pricing page should be treated as the main source for detailed and updated prices.
Prices may vary depending on assessment, treatment suitability, prescription requirements, treatment combinations and follow-up needs. Please check the full pricing page and confirm costs before proceeding.
Risks, limitations and when pigmentation needs medical review
Pigmentation treatments can be helpful, but they must be chosen safely. Pigment type, skin tone, pregnancy, medication, sun exposure and lesion safety all matter.
Prescription safety
Some pigment treatments are unsuitable in pregnancy, breastfeeding, certain medical conditions or with particular medications. A safe plan depends on your history.
Pregnancy and fertility context
Melasma may appear or worsen during pregnancy, and some pigment actives are not appropriate when pregnant, trying to conceive or breastfeeding.
Peels, lasers and rebound pigmentation
Chemical peels, laser and light-based treatment can help selected cases, but irritation or heat can worsen pigmentation if treatment is too aggressive.
Seek medical review if pigmentation is unusual, changing or symptomatic
Cosmetic pigmentation treatment should not be used to treat uncertain lesions, changing moles, bleeding areas, irregular pigmentation or symptoms that need medical assessment.
Educational only. This page does not replace medical diagnosis, prescribing advice or urgent care. Suitability, risks, alternatives and expected outcomes must be discussed during consultation. Results vary. Not a cure.
Hyperpigmentation & Melasma Treatment FAQs
Clear answers to common questions about melasma, post-acne marks, pigmentation, peels, laser, skincare and maintenance.
Hyperpigmentation may be caused by inflammation, acne, sun exposure, hormones, pregnancy, medication, heat, irritation, skin injury or a tendency to produce more pigment after inflammation.
Melasma is a common type of pigmentation that often appears as symmetrical brown or grey-brown patches on the face. It may be influenced by hormones, pregnancy, contraception, HRT, sun exposure, heat and visible light.
No. Post-acne pigmentation is usually a colour change after inflammation. Acne scars usually involve a texture change, such as pitting, dents or uneven skin surface. Both can occur together.
Melasma can often be improved, but it may relapse. Long-term maintenance, sun protection and trigger control are usually important. No permanent cure or guaranteed outcome should be promised.
Treatment may include sun protection, pigment-focused skincare, prescription-led options, azelaic acid, retinoid review, hydroquinone review, tranexamic acid discussion, chemical peels, laser review or combination treatment where suitable.
Chemical peels may help selected pigmentation patterns, but they are not suitable for every skin type or every stage of pigmentation. Skin preparation, peel strength, pigment risk and aftercare matter.
Laser can sometimes help selected pigmentation, but melasma can worsen if treatment is too aggressive or poorly timed. Suitability depends on pigment pattern, skin tone, previous response and risk of rebound pigmentation.
UV exposure, visible light and heat can worsen pigmentation and contribute to relapse. Daily protection is often the foundation of treatment, especially for melasma and post-inflammatory pigmentation.
Yes, if treatment irritates the skin or triggers inflammation. This is why pigment treatment should be staged carefully and adjusted to skin tone, sensitivity and previous response.
Pigmentation treatment usually takes weeks to months. Melasma and deeper pigmentation may take longer and often need maintenance even after improvement.
Some pigment treatments and skincare actives are not suitable in pregnancy, breastfeeding or when trying to conceive. Always disclose pregnancy or fertility plans before starting treatment.
Yes. New, changing, irregular, bleeding, itchy or unusual pigmentation should be medically reviewed before cosmetic treatment is considered.
The featured starting price for a pigmentation consultation is from £150. Further treatment costs depend on whether you need skincare, prescription-led treatment, peels, laser review, test patches or maintenance. Please check the full pricing page for detailed and updated pricing.
It can, especially with melasma or repeated sun exposure, inflammation, hormonal triggers or stopping maintenance too early. Prevention and maintenance are often part of the plan.
Your next steps
1. Book your free consultation
2. Talk through your pigmentation pattern and concerns
3. Have a clinical skin assessment if appropriate
4. Receive a personalised pigmentation plan
5. Review progress and maintain results safely
If pigmentation is affecting your confidence, skin tone or wellbeing, you do not need to guess your way through harsh products. A structured consultation can help clarify the safest next step.
Clinical references used for this page
This page is educational and should be reviewed clinically before publication. The references below support general melasma education, pigmentation triggers, sun protection and safety-first treatment planning.
British Association of Dermatologists
Patient information on melasma, including facial brown or grey patches and common triggers.
Primary Care Dermatology Society
Clinical information on melasma as a common cause of facial hyperpigmentation that worsens after sun exposure.
DermNet dermatology resources
Used for general dermatology context on pigmentation patterns and patient-safe education.
UK clinic pricing benchmarks
London/UK clinic pricing references were used to avoid placeholder pricing and provide a realistic featured consultation price.
References
- 1. British Association of Dermatologists: Melasma patient information.
- 2. Primary Care Dermatology Society: Melasma/chloasma clinical guidance.
- 3. DermNet dermatology education resources on pigmentation and skin conditions.
- 4. UK/London dermatology and skin clinic pricing pages used for pricing benchmark context.
Watch patient stories, case studies and media features
Explore our video gallery to hear real patient experiences, learn more through case-based discussions, and watch selected media coverage featuring our work and approach.
Dr. Joe Daniels
Consultant Gynaecologist & Aesthetic Surgery Specialist With over 20 years of surgical excellence, Mr. Joe Daniels is a…
Read MoreStill not sure where to start?
Browse the wider treatment pages or book a free consultation.
Browse our women’s health FAQs
Find clear answers to common questions about consultations, treatments, symptoms, preparation, aftercare, pricing and what to expect when visiting The Women’s Health Clinic. Use the FAQ bubbles below to continue exploring.