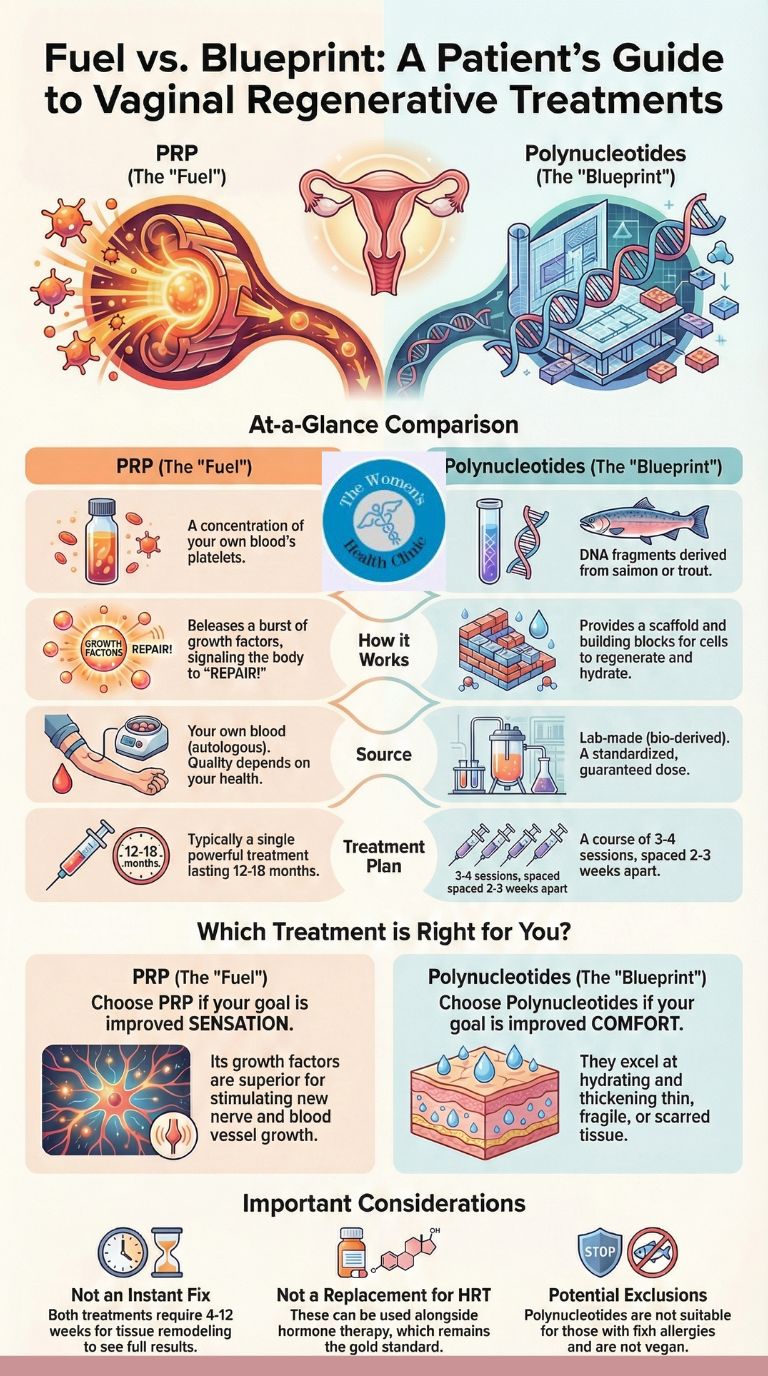
PRP vs polynucleotides—do they help comfort or tissue responsiveness?
Both platelet-rich plasma (PRP) and polynucleotides are regenerative therapies used to improve vaginal tissue health, but they work through different mechanisms. PRP releases growth factors from your own blood to stimulate collagen production and tissue repair, whilst polynucleotides provide fragmented DNA molecules that trigger cellular regeneration and hydration. Clinical evidence suggests both may improve comfort, natural lubrication, and tissue elasticity, though response varies and neither is a guaranteed cure for all symptoms.
Show Detailed Answer
Regenerative treatments for vaginal wellness have gained attention as women seek non-hormonal or complementary options to address dryness, discomfort during sex, recurrent irritation, or loss of tissue tone linked to ageing, childbirth, or menopause. Both PRP and polynucleotides aim to restore the structural integrity of vaginal tissue by encouraging the body’s own healing processes rather than simply masking symptoms.
Understanding how each therapy works, what the evidence shows, and which symptoms they target can help you have an informed conversation with your clinician about whether either option might be suitable for you.
What is PRP (Platelet-Rich Plasma)?
PRP involves drawing a small amount of your own blood, spinning it in a centrifuge to concentrate the platelets, and then injecting the platelet-rich portion into vaginal tissue. Platelets contain growth factors—such as vascular endothelial growth factor (VEGF), platelet-derived growth factor (PDGF), and transforming growth factor-beta (TGF-β)—that stimulate collagen synthesis, improve blood flow, and encourage tissue repair.
In the vaginal context, the goal is to thicken the mucosal lining, enhance natural lubrication by improving tissue hydration and blood supply, and potentially increase sensitivity or responsiveness by supporting nerve and vascular regeneration. The procedure typically involves topical anaesthetic, and effects build gradually over weeks to months as new tissue forms.
What are Polynucleotides?
Polynucleotides are biocompatible chains of nucleotides (the building blocks of DNA), usually derived from purified salmon or trout DNA. When injected into tissue, they act as biostimulators: they trigger fibroblast activity, promote extracellular matrix remodelling, reduce inflammation, and enhance tissue hydration by attracting water molecules into the tissue.
Unlike PRP, polynucleotides do not rely on your own blood components. They work by delivering a biological “scaffold” that signals cells to repair, regenerate, and maintain moisture. In vaginal applications, this may translate to improved elasticity, reduced dryness, and enhanced comfort during intercourse or daily activities.
Key Differences: Mechanism & Application
- Source: PRP uses your own blood; polynucleotides use externally sourced DNA fragments.
- Growth Factor Profile: PRP delivers a broad mix of growth factors specific to your platelets; polynucleotides deliver a standardised biostimulatory signal.
- Tissue Response: PRP primarily stimulates collagen and vascular growth; polynucleotides focus on cellular repair, hydration, and anti-inflammatory effects.
- Onset: Both require time (typically 4–12 weeks) for tissue remodelling. Neither provides instant symptom relief.
- Repeat Treatments: Both often require an initial series (e.g., 2–3 sessions) with maintenance sessions every 6–12 months, depending on individual response.
Which Symptoms Do They Target?
Both therapies are explored for similar presentations, though individual response varies:
- Vaginal Dryness & Atrophy: Both aim to thicken mucosa and improve moisture retention, especially in post-menopausal or oestrogen-deficient states.
- Discomfort During Sex (Dyspareunia): By improving tissue elasticity, hydration, and blood flow, both may reduce friction-related pain.
- Recurrent Irritation or Sensitivity: Polynucleotides’ anti-inflammatory action may be particularly helpful for chronic low-grade inflammation.
- Tissue Laxity or “Loss of Tone”: Both support collagen and elastin production, which may improve structural support.
- Sensitivity & Responsiveness: Improved vascular supply (PRP) or nerve health (both) may enhance sensation, though evidence is still emerging.
What Does the Evidence Show?
The clinical evidence base for both therapies in vaginal regeneration is developing but not yet definitive:
- PRP: Small studies and case series suggest improvements in lubrication, tissue thickness, and sexual function scores, particularly in post-menopausal women or those with lichen sclerosus. However, large randomised controlled trials are limited, and outcomes vary based on preparation technique, injection site, and individual biology.
- Polynucleotides: Evidence is newer. Dermatological and aesthetic medicine data show tissue hydration and repair benefits in skin; early vaginal applications show promise for moisture and elasticity, but peer-reviewed gynaecological trials are sparse.
Neither is currently approved by NICE or the MHRA as a first-line treatment for vaginal atrophy or dyspareunia. Both are typically offered as private, off-label regenerative options, often alongside or after first-line therapies like topical oestrogen or moisturisers have been tried.
Common Concerns & Myths
“Will one treatment fix everything forever?”
No. Both require maintenance. Tissue continues to age, and hormonal changes persist. Most patients need repeat sessions to sustain benefits.
“Are these a replacement for HRT or oestrogen cream?”
Not necessarily. Many clinicians use regenerative therapies alongside hormone therapy for synergistic benefit. Topical oestrogen remains the evidence-based gold standard for vaginal atrophy.
“Is one ‘better’ than the other?”
There is no head-to-head trial comparing PRP and polynucleotides for vaginal health. Choice often depends on clinician experience, your specific symptoms, and whether you prefer an autologous (your own) or biocompatible external product.
Clinical Context
Regenerative therapies like PRP and polynucleotides sit within a broader framework of personalised vaginal wellness care. They are not suitable for everyone and are not a substitute for treating underlying infections, skin conditions, or pelvic floor dysfunction. A thorough clinical assessment—including hormone levels, symptom timeline, and tissue examination—guides whether regenerative approaches are appropriate. Educational only. Results vary. Not a cure.
Evidence-Based Approaches
Self-Care & Lifestyle
Whilst regenerative therapies may support tissue health, foundational self-care remains essential.
- Hydration: Drinking adequate water supports overall tissue moisture.
- Regular Lubrication: Use non-irritating, body-safe lubricants during intimacy to reduce friction whilst tissue remodels.
- Pelvic Floor Awareness: Gentle pelvic floor exercises or relaxation techniques can support tissue responsiveness and reduce guarding.
- Avoiding Irritants: Steer clear of perfumed soaps, douches, or harsh products that can disrupt delicate tissue.
Medical & Specialist Options
Clinical pathways for vaginal discomfort or tissue changes typically begin with first-line, evidence-based treatments before considering regenerative options.
- Topical Oestrogen: The gold standard for vaginal atrophy. Restores thickness, moisture, and pH in oestrogen-deficient tissue.
- Vaginal Moisturisers: Non-hormonal options that provide sustained hydration for mild dryness.
- Pelvic Health Physiotherapy: Addresses muscle tension, guarding, and coordination issues that may worsen discomfort.
- PRP or Polynucleotide Injections: Offered as adjuncts or alternatives when first-line options are insufficient, not tolerated, or patient preference leans toward regenerative approaches.
If you are considering regenerative treatments, you may wish to explore treatment benefits in detail. Many patients also prefer to book a consultation for a personalised assessment of suitability.
Red Flags (When to See a GP)
Seek medical review before pursuing regenerative therapies if you experience unexplained bleeding, offensive discharge, new lumps, persistent pain unrelated to sex, or any symptoms suggesting infection or malignancy.
External Resources:
Educational only. Results vary. Not a cure.
Decision Guide: To choose the right treatment, you must define your goal. For Sexual Sensation (Nerves), PRP is superior due to its ability to regrow nerve endings. For Tissue Comfort (Hydration/Thinness), Polynucleotides are superior as they act as a moisture-binding scaffold.
Additional information
While both are regenerative, they work in opposite ways.
PRP is the "Fuel" (Acute Signal)
- Source: Your own blood (Autologous).
- Mechanism: It mimics an injury. The concentrated platelets release a massive burst of Growth Factors (VEGF, PDGF) that scream "REPAIR" to the body.
- Best For: Sensation & Urgency. The specific growth factors trigger Neurogenesis (new nerve growth) and Angiogenesis (new blood vessels), making it the gold standard for "numbness" or weak orgasms.
Polynucleotides are the "Blueprint" (Scaffold)
- Source: DNA fractions from Trout or Salmon gonads (Bio-derived).
- Mechanism: They provide the "nucleotide building blocks" your cells need to repair themselves (via the Salvage Pathway). They also act as a viscoelastic "hydrogel," trapping water in the tissue.
- Best For: Comfort & Quality. Ideal for post-menopausal "paper-thin" skin (Atrophy) or Lichen Sclerosus scarring, where the goal is to thicken and hydrate the wall rather than stimulate nerves.
A hidden factor in your decision is your own health.
- PRP relies on YOU: If you are over 60, smoke, or have a poor diet, your platelets may be "lazy" and contain fewer growth factors. The result depends entirely on your blood quality.
- Polynucleotides are Standardized: Because they are manufactured in a lab (usually from fish sources), every syringe has a guaranteed concentration of active ingredients, regardless of your age or health.
Polynucleotides (brands like PhilArt, Plinest, or Newest) are derived from the sperm/gonads of Salmon or Trout.
- Allergy Alert: While highly purified to remove proteins, they are generally contraindicated if you have a severe fish allergy.
- Lifestyle: They are not Vegan. PRP, being made from your own blood, is fully vegan and halal/kosher compatible.
PRP (The O-Shot): Often performed as a single powerful treatment that lasts 12–18 months, though some patients opt for a 2nd booster at 8 weeks.
Polynucleotides: These are a "slow burn." You typically require a course of 3–4 sessions spaced 2–3 weeks apart. You will likely not see a result after just one session.