Moisturisers vs Lubricants—What’s the Difference for Comfort?
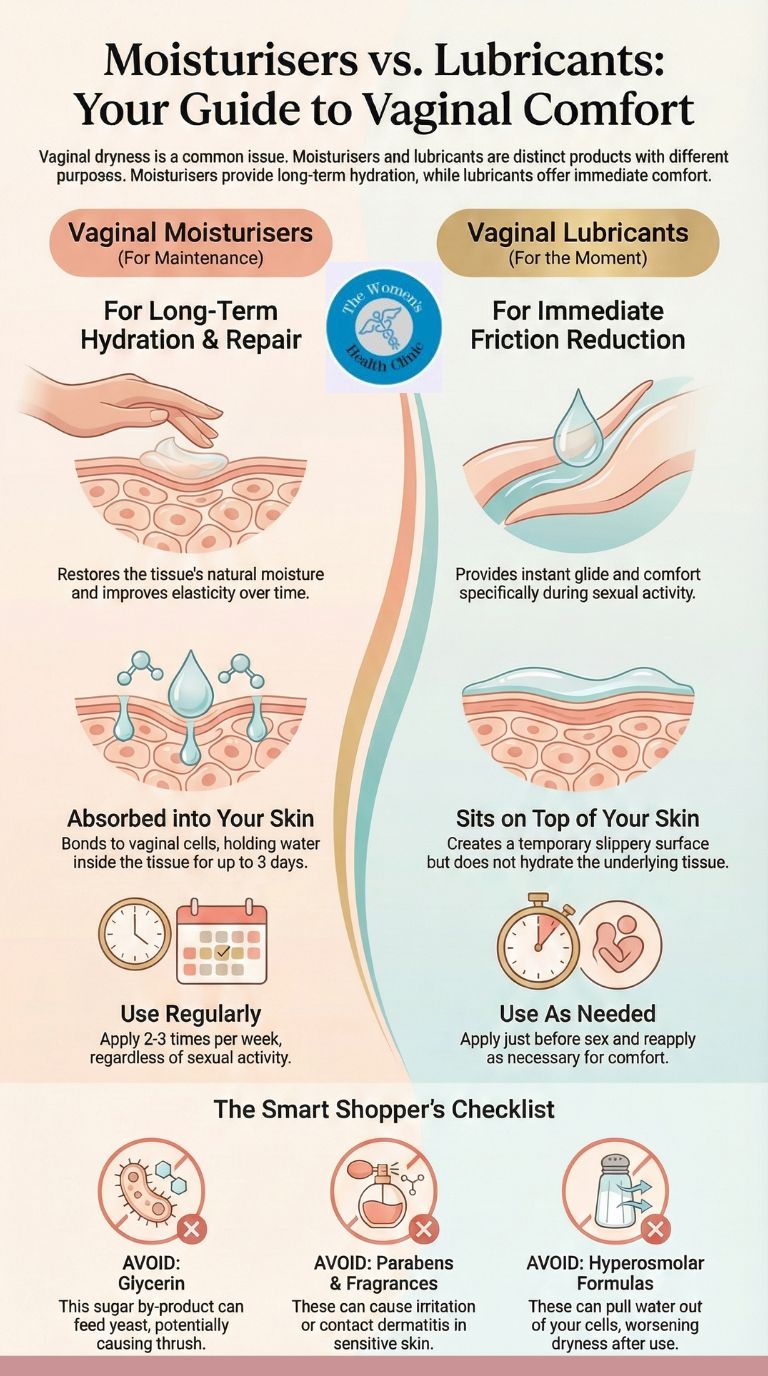
Vaginal moisturisers and lubricants serve different but complementary purposes. Moisturisers are designed for regular, daily use to restore tissue hydration over time, whilst lubricants are used immediately before sexual activity to reduce friction during penetration. Understanding which product to use—and when—can significantly improve vulvovaginal comfort, reduce pain, and support intimate wellbeing.
Show Detailed Answer
Many women experience vaginal dryness at some point in their lives—particularly during breastfeeding, perimenopause, menopause, or following cancer treatment. This dryness is not just uncomfortable; it can lead to itching, soreness, and pain during sex (dyspareunia), which in turn can affect confidence, body image, and relationships.
The confusion between moisturisers and lubricants is common. Both are available over the counter, both are applied to the vaginal area, and both promise “relief.” However, they work in fundamentally different ways, and using the wrong product at the wrong time can leave you frustrated or still in discomfort.
What Are Vaginal Moisturisers?
Vaginal moisturisers are formulated to mimic the body’s natural moisture and are designed to be absorbed into the vaginal tissue. They are used regularly—typically every 2 to 3 days—regardless of sexual activity. Think of them like a daily face moisturiser: they hydrate the tissue, improve elasticity, and help restore the vaginal lining’s health over time.
- Purpose: Long-term tissue hydration and barrier repair.
- Frequency: Applied 2–3 times per week, even when not having sex.
- Effect Duration: Lasts 2–3 days per application.
- Best For: Chronic dryness, atrophy (thinning tissue), post-menopausal changes, or conditions like Genitourinary Syndrome of Menopause (GSM).
- Examples: Yes VM, Replens MD, Sylk Natural Intimate Moisturiser.
Moisturisers do not provide immediate “slip” during intercourse, so they should not be used as a substitute for lubricant in the moment.
What Are Vaginal Lubricants?
Lubricants are designed to reduce friction during sexual activity. They sit on the surface of the tissue and provide instant glide, but they do not treat the underlying dryness. Lubricants are applied just before sex and are available in three main types:
- Water-Based: Safe with condoms and toys, easy to wash off, but may need reapplication. Examples: Liquid Silk, Yes WB.
- Silicone-Based: Long-lasting, waterproof, safe with condoms but not all silicone toys. Examples: Uberlube, ID Millennium.
- Oil-Based: Very slippery and soothing, but degrade latex condoms. Only suitable for non-barrier intimacy. Examples: coconut oil, Yes OB.
Purpose: Immediate friction reduction during penetration.
Frequency: Applied as needed, just before sex.
Effect Duration: Minutes to an hour, depending on type.
Best For: Situational dryness, peri-sex comfort, or alongside moisturisers for dual support.
Can You Use Both Together?
Absolutely—and for many women, this combination is ideal. A regular moisturiser maintains tissue health and baseline comfort, whilst a lubricant ensures smooth, pain-free intimacy. For example:
- Apply a vaginal moisturiser (e.g., Replens MD) every Monday and Thursday evening.
- Apply a water-based lubricant (e.g., Sylk or YES WB) generously just before sex.
This two-pronged approach addresses both the chronic dryness (moisturiser) and the acute friction (lubricant).
Common Concerns & Myths
“Can’t I just use a lubricant all the time instead of a moisturiser?”
No. Lubricants only work on the surface and wash away quickly. They do not restore tissue hydration or improve the vaginal lining’s health. For ongoing dryness, a moisturiser is essential.
“Is it safe to use Vaseline or baby oil?”
No. Petroleum-based products (like Vaseline) are not designed for internal use, can disrupt the vaginal pH, increase infection risk, and degrade latex condoms. Stick to body-safe, pH-balanced products.
“Will using these products make me dependent on them?”
No. There is no evidence that using moisturisers or lubricants reduces your body’s natural ability to self-lubricate. They are supportive tools, not addictive substances.
Clinical Context
Vaginal dryness is a hallmark symptom of oestrogen deficiency, which causes the vaginal lining to become thinner, less elastic, and less able to produce natural lubrication. This is particularly common during menopause but can also occur during breastfeeding, chemotherapy, or with certain medications (e.g., antihistamines, antidepressants). Moisturisers and lubricants are first-line, non-hormonal interventions recommended by the NHS and NICE for managing mild to moderate symptoms of GSM. For more severe atrophy, topical oestrogen may be needed. Educational only. Results vary. Not a cure.
Evidence-Based Approaches
Self-Care & Lifestyle
Choosing the right product and using it correctly is key to symptom relief.
- Read Labels: Avoid products with glycerin (can cause yeast overgrowth), parabens, or fragrances. Look for pH-balanced (3.8–4.5) and osmolality-tested formulas.
- Apply Correctly: Moisturisers should be inserted into the vagina (with an applicator or clean finger) and massaged gently into the tissue. Lubricants should be applied to both the vulva and the partner or toy.
- Be Generous: More is better. Reapply lubricant during sex if needed.
- Hydration & Diet: Drink plenty of water and consider omega-3 fatty acids, which support mucous membrane health.
Medical & Specialist Options
If over-the-counter products do not provide adequate relief, or if dryness is accompanied by pain, burning, or bleeding, a medical review is recommended.
- Topical Oestrogen: Low-dose vaginal oestrogen (creams, pessaries, or rings) is the gold standard for moderate to severe vaginal atrophy. It restores tissue thickness and elasticity.
- Regenerative Treatments: Options such as vaginal laser therapy or platelet-rich plasma (PRP) can stimulate collagen production and improve tissue health in suitable candidates.
- Pelvic Health Physiotherapy: If dryness coexists with pelvic floor tension or pain, specialist physio can help relax the muscles and improve comfort.
For a comprehensive approach to vaginal health, you can explore treatment benefits and book a consultation with our specialist team.
Red Flags (When to See a GP)
Seek medical advice if you experience persistent bleeding after sex, unusual discharge, a foul odour, severe pain, or if dryness does not improve after 4–6 weeks of using moisturisers and lubricants.
External Resources:
Educational only. Results vary. Not a cure.
Clinical Distinction: They are not interchangeable. Lubricants reduce friction temporarily (for sex), while Moisturisers are absorbed into the tissue to repair cells (maintenance). Using a hyperosmolar lubricant can actually worsen dryness by stripping water from your cells.
Additional Clinical Comparisons
Moisturisers (Maintenance)
- Action: They contain hydrophilic molecules like Hyaluronic Acid or Polycarbophil that physically bond to the vaginal wall cells. They hold water inside the tissue for up to 3 days.
- Frequency: Use every 2–3 days (bedtime). This matches the natural turnover rate of vaginal cells.
Lubricants (Immediate)
- Action: They sit on top of the skin to reduce friction. They do not hydrate the cells.
- Frequency: Use only during sexual activity.
Why do some lubes sting? It's often the "Osmolality" (concentration of particles).
- The Problem: Many standard lubricants are Hyperosmolar (high salt/sugar/glycerin content).
- The Effect: They pull water out of your vaginal cells to balance the chemistry. This leaves the tissue dehydrated and damaged after the lube dries, leading to irritation and susceptibility to infection.
- The Solution: Look for "Iso-Osmolar" products (balanced to your body's natural fluids).
Avoid these common ingredients if you have pain or recurrent infections:
- Glycerin: It is a sugar by-product that feeds Candida (Thrush) yeast.
- Chlorhexidine: An antibacterial preservative that kills the good Lactobacillus bacteria you need for a healthy pH.
- Parabens: Endocrine disruptors that can cause contact dermatitis in sensitive skin.