Pudendal neuralgia or nerve pain—what are the clues?
Pudendal neuralgia is chronic pelvic pain caused by irritation or compression of the pudendal nerve, which supplies sensation to the vulva, perineum, and rectum. The hallmark clues include burning or electric-shock pain that worsens with sitting, improves when standing or lying down, and is typically absent at night. Because symptoms can mimic other conditions, accurate diagnosis requires careful assessment of your pain pattern, triggers, and response to position changes.
Show Detailed Answer
Pudendal neuralgia (PN) is a neuropathic pain syndrome affecting the distribution of the pudendal nerve, which runs from the lower spine through the pelvis to the genital and anal regions. The pain is often described as burning, stabbing, aching, or like sitting on a razor blade. It can feel isolating and bewildering, especially when multiple healthcare professionals fail to recognise the pattern.
Unlike musculoskeletal pain or infection-related discomfort, nerve pain follows the anatomical path of the nerve itself. The pudendal nerve can become entrapped, stretched, or inflamed due to trauma (such as childbirth or cycling), pelvic surgery, prolonged sitting, or chronic pelvic floor muscle tension. Understanding the characteristic “clues” helps differentiate PN from conditions like vulvodynia, interstitial cystitis, or endometriosis.
The Five Nantes Criteria: Diagnostic Clues
International experts developed the “Nantes Criteria” to help identify pudendal neuralgia. These clinical features are remarkably consistent across patients:
- Pain in the territory of the pudendal nerve: This includes the vulva, clitoris, perineum, anus, or a combination. Pain is typically one-sided but can be bilateral.
- Pain is worse with sitting: The nerve is compressed when seated, especially on hard surfaces. Many patients carry a cushion or stand during meetings.
- Pain does not wake you from sleep: Unlike inflammatory conditions, nerve pain usually disappears when lying down and the nerve is decompressed.
- No objective sensory loss on examination: Despite severe pain, pinprick and light touch testing are often normal, though some patients report altered sensation or hypersensitivity.
- Positive response to a pudendal nerve block: Temporary pain relief following an anaesthetic injection near the nerve strongly supports the diagnosis.
Additional Red-Flag Symptoms
Beyond the Nantes Criteria, patients with pudendal neuralgia frequently report:
- Pain triggered by tight clothing or seams: Underwear, jeans, or cycling shorts can aggravate symptoms.
- Bladder or bowel urgency: The pudendal nerve also supplies the pelvic organs, so some patients experience a feeling of incomplete emptying or frequent urination.
- Pain during or after sex: Deep penetration or pressure can compress the nerve further, leading to sharp, burning pain that lingers for hours or days.
- Foreign-body sensation: Some describe feeling as though they are “sitting on a golf ball” or “something is stuck inside.”
Common Concerns & Myths
“Is it all in my head because scans are normal?”
Absolutely not. Nerve pain rarely shows up on standard MRI or ultrasound. Pudendal neuralgia is diagnosed clinically, based on your history and examination findings, not imaging.
“Will I be in pain forever?”
Not necessarily. With appropriate treatment—such as nerve blocks, pelvic physiotherapy, and lifestyle modifications—many patients experience significant improvement. Early intervention improves outcomes.
“Is it caused by cycling or childbirth?”
These are known risk factors, but not everyone with PN has a clear trauma history. Chronic pelvic floor tension, repeated straining, or sitting for long hours can also contribute over time.
Clinical Context
Pudendal neuralgia is under-recognised in primary care, leading to an average diagnostic delay of several years. It affects both women and men, though women are more frequently diagnosed, often following childbirth or gynaecological surgery. The pudendal nerve can be compressed at several anatomical sites, including the Alcock’s canal (between the sacrotuberous and sacrospinous ligaments). Chronic pain can lead to central sensitisation, where the nervous system becomes hyper-responsive, amplifying pain signals. Educational only. Results vary. Not a cure.
Evidence-Based Approaches
Self-Care & Lifestyle
Reducing nerve compression and inflammation is the foundation of symptom management.
- Avoid prolonged sitting: Use a standing desk, take regular breaks, or use a specially designed cushion with a cut-out to relieve pressure on the perineum.
- Modify physical activity: Avoid cycling, rowing, or exercises that directly compress the pelvic floor. Swimming and gentle walking are often better tolerated.
- Wear loose clothing: Choose soft, breathable fabrics and avoid tight waistbands or underwear seams that press on the nerve distribution.
- Heat and ice therapy: Some patients find relief with warm baths or ice packs applied to the perineum for short periods.
Medical & Specialist Options
A multi-disciplinary approach combining medical, physical, and psychological therapies is most effective.
- Pelvic Floor Physiotherapy: Specialist physios trained in pelvic pain can release muscle tension, desensitise hypersensitive tissues, and teach diaphragmatic breathing to calm the nervous system.
- Neuropathic Pain Medications: Drugs such as amitriptyline, gabapentin, or pregabalin can reduce nerve hypersensitivity. These are prescribed at low doses and titrated slowly.
- Pudendal Nerve Blocks: Image-guided injections of local anaesthetic and corticosteroid around the nerve can provide diagnostic confirmation and temporary or longer-term relief.
- Neuromodulation: In refractory cases, techniques such as pulsed radiofrequency or pudendal nerve decompression surgery may be considered by specialist pain clinics.
- Pain Psychology: Chronic pain affects mental health. Cognitive behavioural therapy (CBT) and mindfulness can help manage the emotional burden and break the pain-fear cycle.
For a comprehensive assessment and tailored approach, you can meet the clinical team specialising in pelvic pain. Many patients also wish to book a consultation to discuss their symptoms in depth.
C. Red Flags (When to see a GP urgently)
Seek urgent medical review if you experience sudden loss of bladder or bowel control (cauda equina syndrome), numbness spreading to both legs, severe unrelenting pain unresponsive to any analgesia, or signs of infection such as fever or discharge.
External Resources:
Educational only. Results vary. Not a cure.
Diagnostic Clue: Pudendal Neuralgia is often called the "Sitting Disease." The clearest giveaway is the Toilet Seat Sign: if your pain disappears when sitting on a toilet (because the pressure is off the perineum) but returns on a chair, it strongly suggests nerve entrapment.
Additional Diagnostic Signs
Doctors use a specific checklist called the "Nantes Criteria" to diagnose Pudendal Neuralgia. You likely have it if you meet these 5 rules:
The 5 Essential Signs
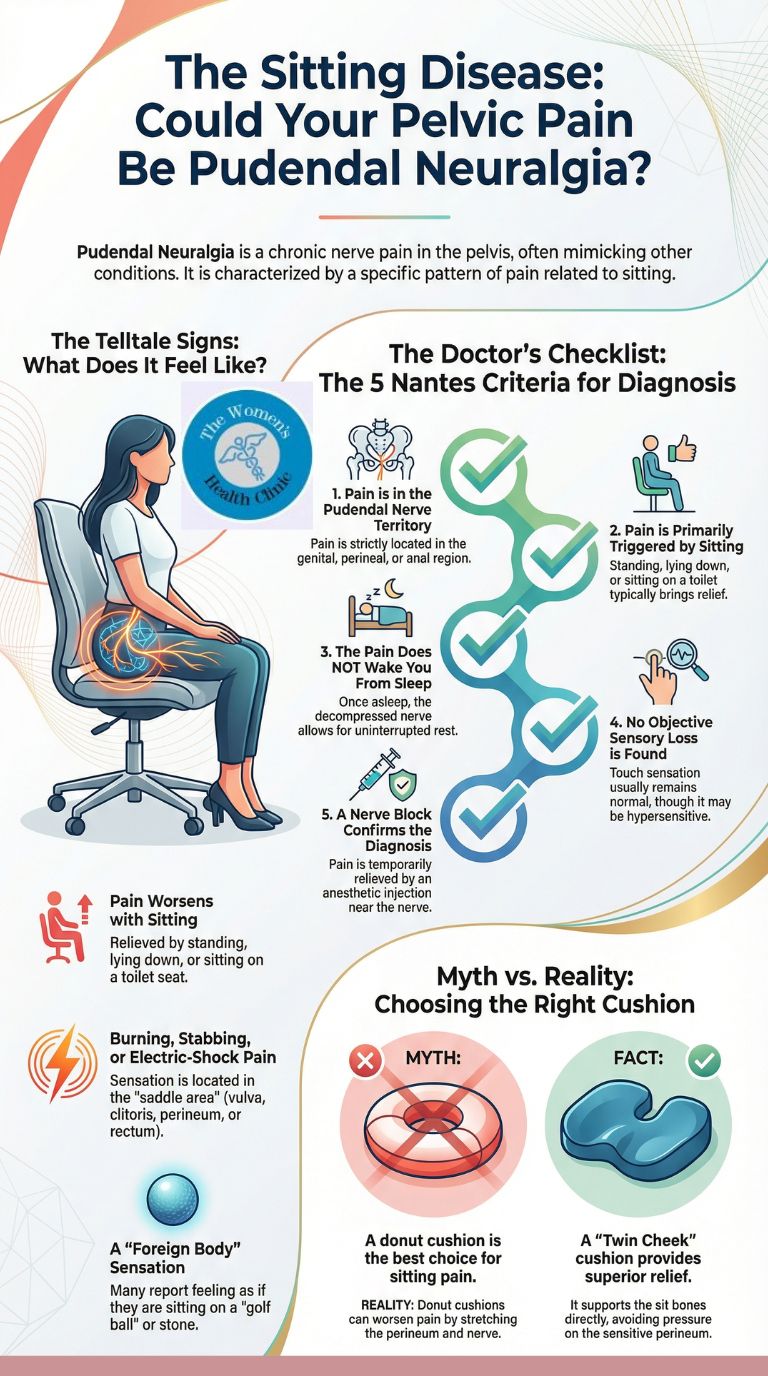
- 1. Territory: Pain is located strictly in the "Saddle Area" (Clitoris/Penis, Vagina/Scrotum, Perineum, or Anus).
- 2. The Sitting Trigger: Pain is worsened by sitting, but usually relieved by standing or lying down.
- 3. The "Night" Rule: The pain does not wake you up at night. (You may struggle to fall asleep, but once asleep, the nerve rests).
- 4. No Numbness: Unlike other nerve injuries, you rarely lose sensation. You can still feel touch, but it hurts (Allodynia).
- 5. Block Confirmation: Pain is temporarily relieved by a diagnostic nerve block injection.
A classic sign of Pudendal Neuralgia is Allotriesthesia (Foreign Body Sensation).
- The Feeling: Many patients report feeling like there is a "golf ball," "stone," or "hot poker" stuck in the rectum or vagina, even though nothing is there.
- The Cause: This is a sensory hallucination caused by the trapped nerve misfiring signals to the brain.
These two nerves run close together but serve different areas.
Know the difference
- Sciatica (Leg): Pain radiates from the lower back, down the buttock and into the leg/foot. It rarely affects the genitals.
- Pudendal (Saddle): Pain is central—between the legs (perineum) and genitals. It rarely goes below the mid-thigh.
- Cycling Risk: Both can be aggravated by cycling, but Pudendal pain is specifically linked to the pressure of the saddle nose.
MYTH: "A donut cushion is best for sitting pain."
REALITY: Donut cushions (rings) can actually worsen Pudendal Neuralgia. The hole creates a vacuum effect that stretches the perineum downwards, pulling on the nerve. A "Twin Cheek" cushion (with a channel down the middle) is clinically superior as it supports the sit bones (Ischial Tuberosities) without stretching the nerve.