Evidence-aware
Safety focused
Women’s Health Clinic FAQ
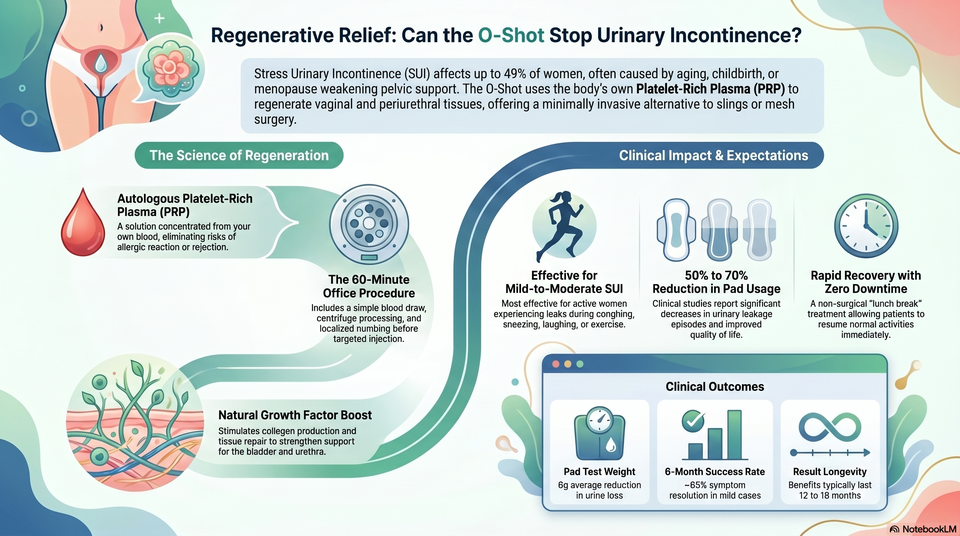
Can the O-Shot help with urinary incontinence?
The O-Shot is sometimes marketed for bladder leakage or urinary incontinence, particularly stress-type leakage, but suitability depends on the type, severity, triggers, pelvic-floor status, childbirth history, menopause status, and red flags.
Direct answer
The O-Shot is sometimes marketed for bladder leakage or urinary incontinence, particularly stress-type leakage, but suitability depends on the type, severity, triggers, pelvic-floor status, childbirth history, menopause status, and red flags.
The most useful plan starts with the underlying cause, not the treatment name. Your clinician should review symptoms, medical history, alternatives, expected benefits, limitations and safety.
Educational only. Suitability must be confirmed after consultation. Results vary. Not a cure.

At a glance
These are the main points to understand before deciding whether this option is suitable.
At a glance
Clinical summary
Mechanism
Concentrated platelets release growth factors that encourage new blood vessels, tissue repair, and nerve regeneration around the urethra.
Suitability must be confirmed after consultation.
Suitability must be confirmed after consultation.
Suitability must be confirmed after consultation.
Suitability must be confirmed after consultation.
Suitability must be confirmed after consultation.
Suitability must be confirmed after consultation.
Important safety note
General Safety: Considered highly safe; the payload is your own biological material, avoiding the foreign body responses associated with synthetic fillers or the burn risks associated with energy-based.
Suitability
Evidence
Safety
Aftercare
Detailed answer
Detailed answer
Investigational Status: Vaginal PRP and the O-Shot are not currently included in standard guidelines (like NICE or BSUG) due to a lack of large-scale, long-term randomised controlled trials. Efficacy Evidence: Pilot studies and prospective cohorts demonstrate an 80% improvement in certain quality-of-life scores (like the ICIQ-SF) and up to a 73.
Clinical context
Investigational Status: Vaginal PRP and the O-Shot are not currently included in standard guidelines (like NICE or BSUG) due to a lack of large-scale, long-term randomised controlled trials.
Evidence
Symptoms
Alternatives
What it means
Investigational Status: Vaginal PRP and the O-Shot are not currently included in standard guidelines (like NICE or BSUG) due to a lack of large-scale, long-term randomised controlled trials.
Why it happens
Symptoms may be linked to physical, hormonal, medication-related, psychological or relationship factors.
Evidence limits
Evidence may be developing, so the page should avoid promise-based language and explain uncertainty.
Treatment fit
Suitability depends on history, symptoms, examination where appropriate and discussion of alternatives.
What this means in practice
Procedure Time: It is a fast, office-based intervention taking approximately 30 to 60 minutes from start to finish. Pain Management: A topical numbing cream (such as 2% Lidocaine gel) is applied 20 minutes prior to the injections to minimise discomfort.
Initial Results: Improvements typically begin to manifest within 4 to 6 weeks following the injections. Peak Results: The peak reported response and reported symptom change are generally observed around 3 months post-treatment.
Patient safety
Why proper assessment matters
Assessment helps separate marketing claims from safe, individualised clinical decision-making.
It checks the cause
Investigational Status: Vaginal PRP and the O-Shot are not currently included in standard guidelines (like NICE or BSUG) due to a lack of large-scale, long-term randomised controlled trials.
It protects safety
General Safety: Considered highly safe; the payload is your own biological material, avoiding the foreign body responses associated with synthetic fillers or the burn risks associated with energy-based.
It reviews alternatives
Procedure Time: It is a fast, office-based intervention taking approximately 30 to 60 minutes from start to finish.
It sets expectations
Initial Results: Improvements typically begin to manifest within 4 to 6 weeks following the injections.
A clinical decision, not a shortcut
The safest final page should explain what the intervention may do, what it cannot promise, and when another route may be better.
Treatment should be discussed with realistic goals, informed consent, clear aftercare and a plan for review.
Considerations
What to consider
Procedure Time: It is a fast, office-based intervention taking approximately 30 to 60 minutes from start to finish. Pain Management: A topical numbing cream (such as 2% Lidocaine gel) is applied 20 minutes prior to the injections to minimise discomfort.
Consultation priorities
Consultation: A thorough assessment of medical history, pelvic exams, and the completion of validated symptom questionnaires (e. g.
Consent
Aftercare
Follow-up
Before treatment
Consultation: A thorough assessment of medical history, pelvic exams, and the completion of validated symptom questionnaires (e. g.
During care
The clinician should explain the procedure, likely sensations, limits and alternatives.
Aftercare
Written aftercare and follow-up should be clear before the patient leaves.
When to reassess
If expected improvement does not occur, the plan should be reviewed rather than repeated automatically.
Practical expectations
Initial Results: Improvements typically begin to manifest within 4 to 6 weeks following the injections.
Costs, access and treatment plans should be confirmed before booking.
Common concerns and myths
Common misconceptions
Clear patient information should correct over-simple claims and keep expectations realistic.
Myth: All bladder leakage is stress incontinence.
Reality: suitability depends on the symptom pattern, medical history, contraindications, alternatives and individual goals.
Myth: PRP is appropriate for every urinary symptom.
Reality: results vary, evidence may be developing, and non-response should prompt reassessment.
Myth: Leaking after childbirth or menopause is something to simply accept.
Reality: injections, devices and intimate procedures can still carry risks and need proper consent and aftercare.
Evidence and advertising
Marketing language should not outrun clinical evidence.
Alternatives
Procedure Time: It is a fast, office-based intervention taking approximately 30 to 60 minutes from start to finish.
Safety checklist
Safety checklist
Use these questions to decide whether treatment should be discussed, delayed or redirected.
Has the cause been assessed?
Symptoms should be reviewed in context before selecting a treatment.
Are red flags absent?
General Safety: Considered highly safe; the payload is your own biological material, avoiding the foreign body responses associated with synthetic fillers or the burn risks associated with energy-based.
Are alternatives clear?
Procedure Time: It is a fast, office-based intervention taking approximately 30 to 60 minutes from start to finish.
Is follow-up planned?
The clinic should explain aftercare, review timing and when to seek help.
Reassuring signs
Proceeding is more reasonable when goals are clear, red flags have been checked, and expectations are realistic.
No red flags
Follow-up plan
Reasons to pause
General Safety: Considered highly safe; the payload is your own biological material, avoiding the foreign body responses associated with synthetic fillers or the burn risks associated with energy-based.
Bleeding
Infection
When to escalate
When to seek medical help
Some symptoms should be assessed before any elective intimate treatment. Use NHS 111 online
Severe or worsening pain
General Safety: Considered highly safe; the payload is your own biological material, avoiding the foreign body responses associated with synthetic fillers or the burn risks associated with energy-based.
Bleeding or discharge
Unexplained bleeding, unusual discharge or new pelvic symptoms should be reviewed.
Infection signs
Fever, spreading redness, pus or feeling unwell after a procedure needs urgent advice.
Emergency symptoms
Call 999 in a life-threatening emergency, including collapse, chest pain or breathing difficulty.
Use NHS 111 for urgent advice or call 999 in a life-threatening emergency. This page is educational and does not replace individual medical assessment.
More clinical detail
Benchmark positioning
- The strongest page captures the commercial O-Shot search but wins trust by sorting leakage types before treatment options.
Clinical reality
- Investigational Status: Vaginal PRP and the O-Shot are not currently included in standard guidelines (like NICE or BSUG) due to a lack of large-scale, long-term randomised controlled trials.
Timeline and expectations
- Initial Results: Improvements typically begin to manifest within 4 to 6 weeks following the injections. Peak Results: The peak reported response and reported symptom change are generally observed around 3 months post-treatment.
Practical logistics
- Procedure Time: It is a fast, office-based intervention taking approximately 30 to 60 minutes from start to finish.
Research sources
- Dankova I, Pyrgidis N, et al. (2023). 'Efficacy and Safety of Platelet-Rich Plasma Injections for the Treatment of Female Sexual Dysfunction and Stress Urinary Incontinence: A Systematic Review.' Biomedicines.
- Grigoriadis T, Kalantzis C, et al. (2024). 'Platelet-Rich Plasma for the Treatment of Stress Urinary Incontinence-A randomised Trial.' Urogynecology (Phila).
- Chiang C-H, Kuo H-C. (2022). 'The Efficacy and Mid-term Durability of Urethral Sphincter Injections of Platelet-Rich Plasma in Treatment of Female Stress Urinary Incontinence.' Frontiers in Pharmacology.
- Borislavschi A, Toma C-V, et al. (2026). 'Comparing Regenerative and Rehabilitative Strategies for Female Stress Urinary Incontinence: Platelet-Rich Plasma vs. Pelvic Floor Muscle Training—A Prospective Study Evaluating Quality of Life.' Bioengineering.
Regulatory resources
Authoritative resources
These resources support assessment-led, evidence-aware patient information.
NICE guidance on vaginal laser for urogenital atrophy
NICE is a UK authority for interventional procedure governance and supports cautious language about evidence, consent and audit.
FDA safety communication on vaginal rejuvenation devices
This safety communication is a useful regulatory reference for avoiding over-claiming around sexual enhancement procedures.
RCOG patient information on menopause symptom treatment
RCOG patient information supports assessment-led discussion of vaginal dryness, discomfort and hormone-related symptoms.
Next step
Book a clinical consultation
A consultation can confirm whether this treatment may be suitable, whether another pathway should come first, and what realistic outcomes and aftercare would look like.
▶ View Research Sources (12 Sources)
These 12 source names are selected from 24 display-ready sources, with a raw audit trail of 114 imported records. Additional reviewed material included UK clinical guidance, professional society guidance, peer-reviewed clinical papers, evidence reviews; duplicate, low-relevance and non-clinical records were removed before display.
Educational only. This content is provided for educational and informational purposes only and does not constitute professional medical advice, diagnosis, or treatment. The O-Shot for urinary incontinence represents an off-label use of autologous regenerative therapies, and individual clinical results vary significantly based on patient biology, age, and severity of symptoms. Always consult with a registered healthcare professional to undergo a mandatory diagnostic assessment and to explore all established, evidence-based alternatives for managing urinary incontinence before proceeding with investigational procedures. Results vary. Not a cure.