Evidence-aware
Safety focused
Women’s Health Clinic FAQ
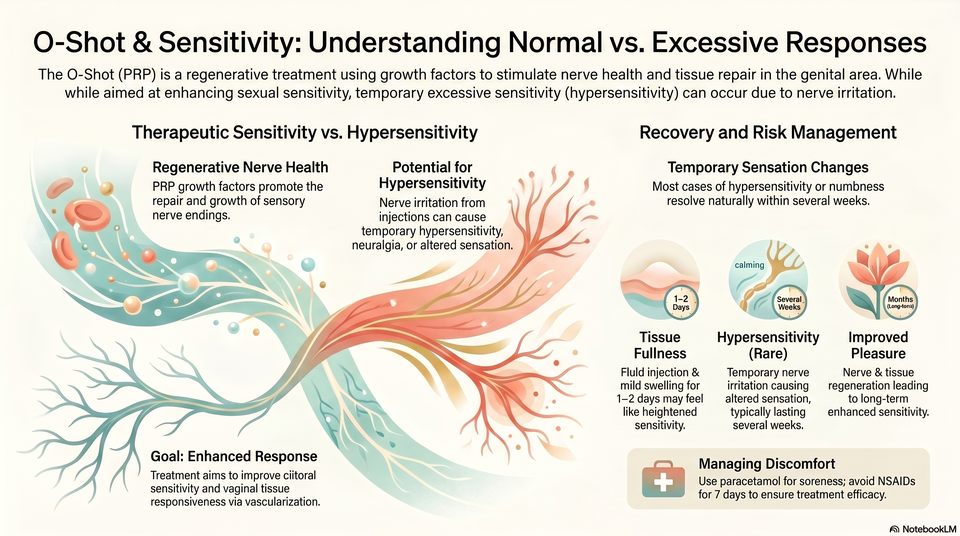
Can the O-Shot cause excessive sensitivity?
Temporary tenderness, swelling, bruising, pressure, or heightened awareness can happen after intimate injections, but persistent excessive sensitivity, pain, burning, numbness, or unwanted arousal symptoms are not outcomes to ignore.
Direct answer
Temporary tenderness, swelling, bruising, pressure, or heightened awareness can happen after intimate injections, but persistent excessive sensitivity, pain, burning, numbness, or unwanted arousal symptoms are not outcomes to ignore. The page should explain that the O-Shot is intended to support tissue quality and sensitivity in selected patients, not to create uncontrolled hypersensitivity.
The most useful plan starts with the underlying cause, not the treatment name. Your clinician should review symptoms, medical history, alternatives, expected benefits, limitations and safety.
Educational only. Suitability must be confirmed after consultation. Results vary. Not a cure.

At a glance
These are the main points to understand before deciding whether this option is suitable.
At a glance
Clinical summary
Laser Modalities
Non-ablative Erbium:YAG (Er:YAG, 2940 nm) and microablative fractional CO2 lasers.
Biologic Modality
Autologous Platelet-Rich Plasma (PRP) injections.
Primary Outcome Metrics
Statistically significant reductions in ICIQ-UI SF scores and 1-hour pad test weights.
Target Population
Optimized for women with mild-to-moderate SUI (Stamey’s Grade 1–2).
Important safety note
Common Adverse Effects: Increased vaginal discharge (reported by 88% in laser trials), transient de novo urgency, mild pain, and pinpoint bleeding.
Suitability
Evidence
Safety
Aftercare
Detailed answer
Detailed answer
Success is highly contingent upon baseline severity and patient characteristics. Outcome Data Density: Objective Success: In Grade 1 SUI, Kuszka (2019) reported a 91% objective cure/improvement rate at 6 months.
Clinical context
Outcome Data Density:
Evidence
Symptoms
Alternatives
What it means
Outcome Data Density:
Why it happens
Objective Success: In Grade 1 SUI, Kuszka (2019) reported a 91% objective cure/improvement rate at 6 months.
Evidence limits
Comparative Pad Weights: Okui (2019) demonstrated that laser therapy reduced 1-hour pad test weights from 34g to 2g, which is comparable to mid-urethral slings (TVT/TOT), which reduced weights.
Treatment fit
PRP Specificity: Tahoon (2021) found that while SUI symptoms improved, sexual function (FSFI scores) showed no significant change (p=0.25).
What this means in practice
Procedure Setting: Outpatient clinical environment. No general anesthesia is required, though topical lidocaine (spray or cream) is standard. Laser Equipment: Specialized probes such as the XS Dynamis (Er:YAG) or MonaLisa Touch (CO2). PRP Processing: Standard Preparation: Centrifugation (e. g.
Laser Regimen: Typically 3 to 5 sessions spaced 4 to 6 weeks apart. PRP Regimen: A single-session outpatient procedure involving the centrifugation of 15cc of peripheral blood to yield approximately 4cc of PRP for immediate paraurethral injection.
Patient safety
Why proper assessment matters
Assessment helps separate marketing claims from safe, individualised clinical decision-making.
It checks the cause
Outcome Data Density:
It protects safety
Common Adverse Effects: Increased vaginal discharge (reported by 88% in laser trials), transient de novo urgency, mild pain, and pinpoint bleeding.
It reviews alternatives
Procedure Setting: Outpatient clinical environment. No general anesthesia is required, though topical lidocaine (spray or cream) is standard.
It sets expectations
Laser Regimen: Typically 3 to 5 sessions spaced 4 to 6 weeks apart.
A clinical decision, not a shortcut
The safest final page should explain what the intervention may do, what it cannot promise, and when another route may be better.
Treatment should be discussed with realistic goals, informed consent, clear aftercare and a plan for review.
Considerations
What to consider
Procedure Setting: Outpatient clinical environment. No general anesthesia is required, though topical lidocaine (spray or cream) is standard. Laser Equipment: Specialized probes such as the XS Dynamis (Er:YAG) or MonaLisa Touch (CO2). PRP Processing: Standard Preparation: Centrifugation (e. g.
Consultation priorities
Screening: Patients require a normal PAP smear, negative urine culture, and baseline ICIQ-UI SF and/or urodynamics.
Consent
Aftercare
Follow-up
Before treatment
Screening: Patients require a normal PAP smear, negative urine culture, and baseline ICIQ-UI SF and/or urodynamics.
During care
Intra-procedure:
Aftercare
Laser: Involves circular irradiation of the vaginal canal followed by targeted treatment of the urethrovesical junction, anterior vaginal wall, and introitus.
When to reassess
PRP: Injections are administered at a 10mm depth into the paraurethral area, specifically targeting the region near the external urethral sphincter (typically three points on each side).
Practical expectations
Laser Regimen: Typically 3 to 5 sessions spaced 4 to 6 weeks apart.
Laser Equipment: Specialized probes such as the XS Dynamis (Er:YAG) or MonaLisa Touch (CO2).
Common concerns and myths
Common misconceptions
Clear patient information should correct over-simple claims and keep expectations realistic.
Myth: More sensitivity is always better.
Reality: suitability depends on the symptom pattern, medical history, contraindications, alternatives and individual goals.
Myth: Because PRP uses my own blood, it cannot cause uncomfortable.
Reality: results vary, evidence may be developing, and non-response should prompt reassessment.
Myth: Excessive sensitivity means the treatment has worked too well.
Reality: injections, devices and intimate procedures can still carry risks and need proper consent and aftercare.
Evidence and advertising
Objective Success: In Grade 1 SUI, Kuszka (2019) reported a 91% objective cure/improvement rate at 6 months.
Alternatives
Procedure Setting: Outpatient clinical environment. No general anesthesia is required, though topical lidocaine (spray or cream) is standard.
Safety checklist
Safety checklist
Use these questions to decide whether treatment should be discussed, delayed or redirected.
Has the cause been assessed?
Symptoms should be reviewed in context before selecting a treatment.
Are red flags absent?
Common Adverse Effects: Increased vaginal discharge (reported by 88% in laser trials), transient de novo urgency, mild pain, and pinpoint bleeding.
Are alternatives clear?
Procedure Setting: Outpatient clinical environment. No general anesthesia is required, though topical lidocaine (spray or cream) is standard.
Is follow-up planned?
The clinic should explain aftercare, review timing and when to seek help.
Reassuring signs
Proceeding is more reasonable when goals are clear, red flags have been checked, and expectations are realistic.
No red flags
Follow-up plan
Reasons to pause
Common Adverse Effects: Increased vaginal discharge (reported by 88% in laser trials), transient de novo urgency, mild pain, and pinpoint bleeding.
Bleeding
Infection
When to escalate
When to seek medical help
Some symptoms should be assessed before any elective intimate treatment. Use NHS 111 online
Severe or worsening pain
Common Adverse Effects: Increased vaginal discharge (reported by 88% in laser trials), transient de novo urgency, mild pain, and pinpoint bleeding.
Bleeding or discharge
Urogynaecological Red Flags: Rare but documented risks include vesicovaginal fistula, transverse vaginal septum, and vaginal shortening. Chronic pain, burning, and dyspareunia are reported in the FDA MAUDE database.
Infection signs
Surgical Interference: A critical concern is laser-induced vaginal mucosa scarring. Al-Badr (2019) reported that post-laser tissue becomes thin, friable, and rigid, losing its natural rugae.
Emergency symptoms
Call 999 in a life-threatening emergency, including collapse, chest pain or breathing difficulty.
Use NHS 111 for urgent advice or call 999 in a life-threatening emergency. This page is educational and does not replace individual medical assessment.
More clinical detail
Benchmark positioning
- WHC can win by owning the safety question competitors avoid: the goal is comfortable, wanted sexual sensation, not uncontrolled hypersensitivity.
Clinical reality
- Outcome Data Density:
- Objective Success: In Grade 1 SUI, Kuszka (2019) reported a 91% objective cure/improvement rate at 6 months.
- Comparative Pad Weights: Okui (2019) demonstrated that laser therapy reduced 1-hour pad test weights from 34g to 2g, which is comparable to mid-urethral slings (TVT/TOT), which reduced weights from ~38g to 3–4g.
- PRP Specificity: Tahoon (2021) found that while SUI symptoms improved, sexual function (FSFI scores) showed no significant change (p=0.25).
- Urodynamic Shifts: Following PRP, significant increases were noted in residual urine (RU) (9.7ml to 46.7ml; p=0.028) and volume at first sensation to void (FS) (135.8ml to 163.8ml; p=0.001).
- Success Predictors:
Timeline and expectations
- Laser Regimen: Typically 3 to 5 sessions spaced 4 to 6 weeks apart.
- PRP Regimen: A single-session outpatient procedure involving the centrifugation of 15cc of peripheral blood to yield approximately 4cc of PRP for immediate paraurethral injection.
- Result Durability:
- Short-term: Significant improvements are typically realized between 1 and 3 months. For example, Gambacciani (2018) noted ICIQ-SF scores dropping from a baseline of 12.2 to 4.8 at 1 month post-treatment.
- Long-term: Laser efficacy often wanes over time. Scores may return toward baseline at 18–24 months (e.g., Gambacciani reported a return to 9.9 by 24 months, losing statistical significance).
- PRP: Current data (Tahoon, 2021) demonstrates efficacy up to 3 months; longer-term data is pending.
Practical logistics
- Procedure Setting: Outpatient clinical environment. No general anesthesia is required, though topical lidocaine (spray or cream) is standard.
- Laser Equipment: Specialized probes such as the XS Dynamis (Er:YAG) or MonaLisa Touch (CO2).
- PRP Processing:
- Standard Preparation: Centrifugation (e.g., Golden VAC at 3000 RPM for 10 minutes) creates a three-layer separation (RBCs, PRP/Leukocytes, and PPP).
- Protocol Variability: Parameters vary by manufacturer. Systems like Cascade, Plateltex, and SmartPrep 2 require a double-spin protocol. Consultants must adhere to specific G-force vs. RPM instructions provided by the kit manufacturer.
Research sources
- Blaganje M, et al. (2018) Non-ablative Er:YAG laser therapy effect on stress urinary incontinence: A randomized controlled trial.
- Wang Y, et al. (2021) Safety and efficacy of vaginal laser therapy for stress urinary incontinence: a meta-analysis.
- Tahoon AS, et al. (2021) The Role of Platelet Rich Plasma Injections in Cases of Stress Incontinence.
- Gambacciani M, et al. (2020) Safety of vaginal erbium laser: A review of 113,000 patients treated in the past 8 years.
Regulatory resources
Authoritative resources
These resources support assessment-led, evidence-aware patient information.
NICE guidance on vaginal laser for urogenital atrophy
NICE is a UK authority for interventional procedure governance and supports cautious language about evidence, consent and audit.
FDA safety communication on vaginal rejuvenation devices
This safety communication is a useful regulatory reference for avoiding over-claiming around sexual enhancement procedures.
RCOG patient information on menopause symptom treatment
RCOG patient information supports assessment-led discussion of vaginal dryness, discomfort and hormone-related symptoms.
Next step
Book a clinical consultation
A consultation can confirm whether this treatment may be suitable, whether another pathway should come first, and what realistic outcomes and aftercare would look like.
▶ View Full Research Bibliography (10 Sources)
Educational only. These procedures are supported by limited clinical evidence. Long-term safety and efficacy profiles are not yet established, particularly regarding the durability of results beyond 24 months. Traditional conservative management (pelvic floor muscle training) and validated surgical interventions (mid-urethral slings) remain the gold standard. Clinicians should only offer these therapies within the context of robust clinical trials or after comprehensive counseling regarding their experimental status. Results vary. Not a cure.