Evidence-aware
Safety focused
Women’s Health Clinic FAQ
Can the O-Shot improve G-spot sensitivity?
Many O-Shot pages refer to the G-spot or anterior vaginal wall, but clinicians should avoid over-simplifying this anatomy.
Direct answer
Many O-Shot pages refer to the G-spot or anterior vaginal wall, but clinicians should avoid over-simplifying this anatomy. The treatment may support sensitivity in selected patients, but orgasm and pleasure are usually linked with the clitoral-urethral-vaginal complex, arousal, stimulation pattern, tissue comfort, and pelvic floor function rather than one single spot.
The most useful plan starts with the underlying cause, not the treatment name. Your clinician should review symptoms, medical history, alternatives, expected benefits, limitations and safety.
Educational only. Suitability must be confirmed after consultation. Results vary. Not a cure.

At a glance
These are the main points to understand before deciding whether this option is suitable.
At a glance
Clinical summary
| Intervention | Mechanism of.
--- | :--- | :--- | :--- | :--- | | Cross-Linked Hyaluronic Acid (HA) | Immediate volumetric.
Suitability must be confirmed after consultation.
Suitability must be confirmed after consultation.
Suitability must be confirmed after consultation.
Suitability must be confirmed after consultation.
Suitability must be confirmed after consultation.
Suitability must be confirmed after consultation.
Important safety note
Procedural (HA/PRP): Transient effects include localized bruising, swelling, and burning.
Suitability
Evidence
Safety
Aftercare
Detailed answer
Detailed answer
Anatomical discourse has shifted from the "G-spot" toward the concept of a functional clitourethrovaginal complex. Clinical justification for augmentation is based on data showing that women experiencing vaginal orgasms typically possess a thicker urethrovaginal space. The "timing hypothesis" dictates that the benefits for atherosclerosis reduction and mortality are specific to HRT initiation before age 60.
Clinical context
Anatomical discourse has shifted from the "G-spot" toward the concept of a functional clitourethrovaginal complex.
Evidence
Symptoms
Alternatives
What it means
Anatomical discourse has shifted from the "G-spot" toward the concept of a functional clitourethrovaginal complex.
Why it happens
The "timing hypothesis" dictates that the benefits for atherosclerosis reduction and mortality are specific to HRT initiation before age 60.
Evidence limits
Limitations of current regenerative research include the pilot nature of major studies ($n=16$), short follow-up durations, and extreme heterogeneity in PRP protocols, where administration volumes vary widely from.
Treatment fit
Suitability depends on history, symptoms, examination where appropriate and discussion of alternatives.
What this means in practice
HA Injection Protocol: Target: Submucosal layer of the anterior vaginal wall. Technique: Use a metallic Pederson speculum. Perform a clockwise rotation of approximately 20 degrees to identify the paramedial periurethral area. Coordinates/Volume: 2. 5 mL volume, injected 2.
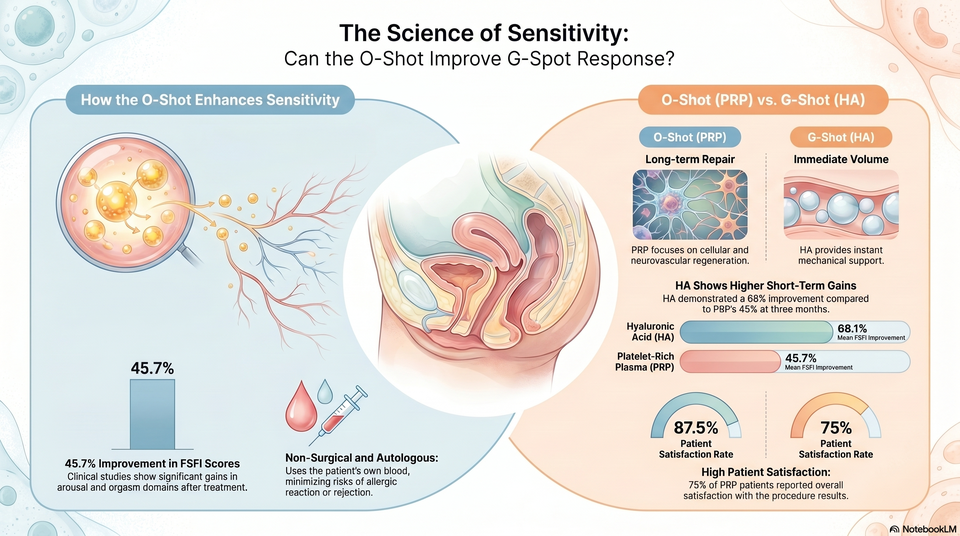
Hyaluronic Acid (HA): Clinically significant improvements in desire, arousal, and orgasm are validated at the 3-month post-treatment interval. Platelet-Rich Plasma (PRP): Significant improvement occurs by 3 months; however, due to its reliance on collagen synthesis and neovascularization, maximal regenerative efficacy may necessitate more extended follow-up.
Patient safety
Why proper assessment matters
Assessment helps separate marketing claims from safe, individualised clinical decision-making.
It checks the cause
Anatomical discourse has shifted from the "G-spot" toward the concept of a functional clitourethrovaginal complex.
It protects safety
Procedural (HA/PRP): Transient effects include localized bruising, swelling, and burning.
It reviews alternatives
HA Injection Protocol:
It sets expectations
Hyaluronic Acid (HA): Clinically significant improvements in desire, arousal, and orgasm are validated at the 3-month post-treatment interval.
A clinical decision, not a shortcut
The safest final page should explain what the intervention may do, what it cannot promise, and when another route may be better.
Treatment should be discussed with realistic goals, informed consent, clear aftercare and a plan for review.
Considerations
What to consider
HA Injection Protocol: Target: Submucosal layer of the anterior vaginal wall. Technique: Use a metallic Pederson speculum. Perform a clockwise rotation of approximately 20 degrees to identify the paramedial periurethral area. Coordinates/Volume: 2. 5 mL volume, injected 2. 5 cm posterior and 2 cm lateral to the mid-urethra.
Consultation priorities
Step 1: Clinical Baseline: Establish scores across all six FSFI domains (desire, arousal, lubrication, orgasm, satisfaction, and pain).
Consent
Aftercare
Follow-up
Before treatment
Step 1: Clinical Baseline: Establish scores across all six FSFI domains (desire, arousal, lubrication, orgasm, satisfaction, and pain).
During care
Step 2: Procedural Analgesia: Application of topical lidocaine (EMLA®) to the vaginal introitus and clitoris.
Aftercare
Step 3: Intervention:
When to reassess
For injections: Position patient in dorsal lithotomy.
Practical expectations
Hyaluronic Acid (HA): Clinically significant improvements in desire, arousal, and orgasm are validated at the 3-month post-treatment interval.
Target: Submucosal layer of the anterior vaginal wall.
Common concerns and myths
Common misconceptions
Clear patient information should correct over-simple claims and keep expectations realistic.
Myth: The G-spot is a certain button.
Reality: suitability depends on the symptom pattern, medical history, contraindications, alternatives and individual goals.
Myth: The O-Shot creates vaginal orgasm for everyone.
Reality: results vary, evidence may be developing, and non-response should prompt reassessment.
Myth: Clitoral stimulation is less valid than G-spot orgasm.
Reality: injections, devices and intimate procedures can still carry risks and need proper consent and aftercare.
Evidence and advertising
The "timing hypothesis" dictates that the benefits for atherosclerosis reduction and mortality are specific to HRT initiation before age 60.
Alternatives
HA Injection Protocol:
Safety checklist
Safety checklist
Use these questions to decide whether treatment should be discussed, delayed or redirected.
Has the cause been assessed?
Symptoms should be reviewed in context before selecting a treatment.
Are red flags absent?
Procedural (HA/PRP): Transient effects include localized bruising, swelling, and burning.
Are alternatives clear?
HA Injection Protocol:
Is follow-up planned?
The clinic should explain aftercare, review timing and when to seek help.
Reassuring signs
Proceeding is more reasonable when goals are clear, red flags have been checked, and expectations are realistic.
No red flags
Follow-up plan
Reasons to pause
Procedural (HA/PRP): Transient effects include localized bruising, swelling, and burning.
Bleeding
Infection
When to escalate
When to seek medical help
Some symptoms should be assessed before any elective intimate treatment. Use NHS 111 online
Severe or worsening pain
Procedural (HA/PRP): Transient effects include localized bruising, swelling, and burning.
Bleeding or discharge
Mandatory Technique: Clinicians must employ a 10-second gentle aspiration prior to HA injection to prevent embolic or intravascular complications.
Infection signs
Hormonal (HRT):
Emergency symptoms
Call 999 in a life-threatening emergency, including collapse, chest pain or breathing difficulty.
Use NHS 111 for urgent advice or call 999 in a life-threatening emergency. This page is educational and does not replace individual medical assessment.
More clinical detail
Benchmark positioning
- WHC can outperform G-spot marketing pages by turning a hype-heavy topic into a clear, respectful anatomy lesson.
Clinical reality
- Anatomical discourse has shifted from the "G-spot" toward the concept of a functional clitourethrovaginal complex.
- The "timing hypothesis" dictates that the benefits for atherosclerosis reduction and mortality are specific to HRT initiation before age 60.
- Limitations of current regenerative research include the pilot nature of major studies ($n=16$), short follow-up durations, and extreme heterogeneity in PRP protocols, where administration volumes vary widely from 2 mL to 10 mL.
Timeline and expectations
- Hyaluronic Acid (HA): Clinically significant improvements in desire, arousal, and orgasm are validated at the 3-month post-treatment interval.
- Platelet-Rich Plasma (PRP): Significant improvement occurs by 3 months; however, due to its reliance on collagen synthesis and neovascularization, maximal regenerative efficacy may necessitate more extended follow-up.
- Hormone Replacement Therapy (HRT):
- Window of Opportunity: Initiation must ideally occur before age 60 or within 10 years of menopause to optimize cardiovascular and bone mineral density benefits.
- Symptom Management: Patients should be counseled that the median duration of vasomotor symptoms (VMS) exceeds 7 years, requiring a long-term management strategy.
Practical logistics
- HA Injection Protocol:
- Target: Submucosal layer of the anterior vaginal wall.
- Technique: Use a metallic Pederson speculum. Perform a clockwise rotation of approximately 20 degrees to identify the paramedial periurethral area.
- Coordinates/Volume: 2.5 mL volume, injected 2.5 cm posterior and 2 cm lateral to the mid-urethra.
- PRP Preparation Protocol:
- Centrifugation: Process autologous blood for exactly 8 minutes.
Research sources
- Barber MA, Eguiluz I (2026). Anterior Vaginal Wall Augmentation using Cross-Linked Hyaluronic Acid versus Platelet-Rich Plasma. JSM Sexual Med 10(1): 1174.
- British Menopause Society & Women’s Health Concern (2020/2025). Recommendations on hormone replacement therapy in menopausal women.
- Moamen Abdelfadil Ismail, et al. (2025). Role of Platelet-Rich Plasma in Female Sexual Health and Recovery: A Systematic Review. Revista Iberoamericana de Psicología del Ejercicio y el Deporte. Vol. 20, nº 5.
Regulatory resources
Authoritative resources
These resources support assessment-led, evidence-aware patient information.
NICE interventional procedures guidance
NICE is a UK authority for interventional procedure governance and supports cautious language about evidence, consent and audit.
FDA safety communication on vaginal rejuvenation devices
This safety communication is a useful regulatory reference for avoiding over-claiming around sexual enhancement procedures.
RCOG patient information on menopause symptom treatment
RCOG patient information supports assessment-led discussion of vaginal dryness, discomfort and hormone-related symptoms.
Next step
Book a clinical consultation
A consultation can confirm whether this treatment may be suitable, whether another pathway should come first, and what realistic outcomes and aftercare would look like.
▶ View Full Research Bibliography (10 Sources)
Educational only. This report is based on current clinical research and consensus statements for informational purposes only. Treatment for female sexual dysfunction and menopausal symptoms must be individualized. Clinicians should refer to the full peer-reviewed studies and institutional guidelines before performing procedures or prescribing HRT. Results vary. Not a cure.