Evidence-aware
Safety focused
Women’s Health Clinic FAQ
Can the O-Shot improve clitoral sensation?
Clitoral sensation is one of the more relevant search intents for the O-Shot, because many clinic pages describe PRP around the clitoral area.
Direct answer
Clitoral sensation is one of the more relevant search intents for the O-Shot, because many clinic pages describe PRP around the clitoral area. clinicians should still keep claims cautious: it may support local tissue response and sensitivity in selected patients, but sensation depends on nerve health, hormones, skin conditions, pain, pelvic floor tone, stimulation, and medication history.
The most useful plan starts with the underlying cause, not the treatment name. Your clinician should review symptoms, medical history, alternatives, expected benefits, limitations and safety.
Educational only. Suitability must be confirmed after consultation. Results vary. Not a cure.

At a glance
These are the main points to understand before deciding whether this option is suitable.
At a glance
Clinical summary
Sexual Function
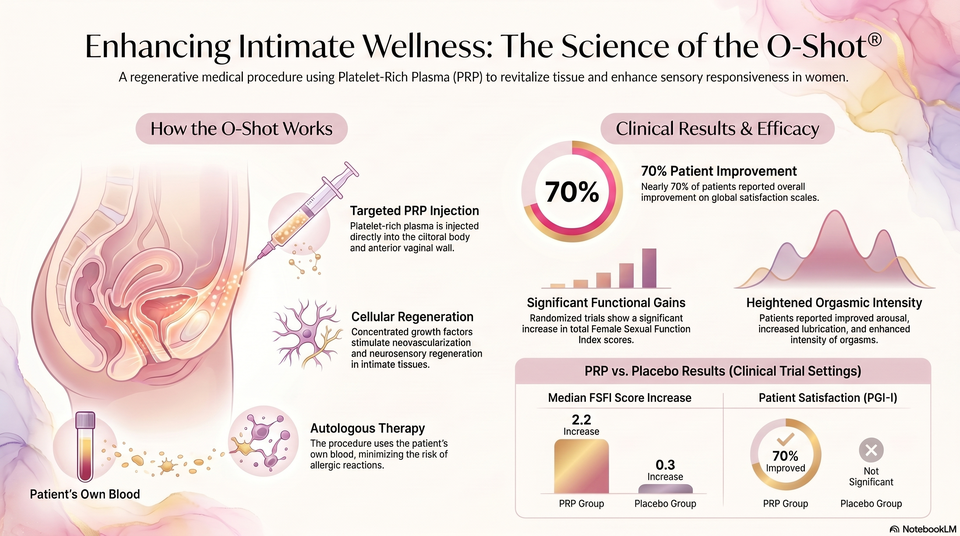
Documented improvements in clitoral sensitivity, arousal, and orgasmic intensity.
Urogynaecology
Management of mild-to-moderate stress urinary incontinence (SUI) via the stimulation of collagen synthesis in the periurethral tissues to.
Dermatological & Menopausal Health
Rejuvenation of the vulva (addressing volume loss and sagging in the labia majora and minora), management of Lichen.
Suitability must be confirmed after consultation.
Suitability must be confirmed after consultation.
Important safety note
Localized pain and pressure at the injection site.
Suitability
Evidence
Safety
Aftercare
Detailed answer
Detailed answer
The field of regenerative gynecology is in a "nascent stage," where high patient satisfaction (70% on the PGI-I scale) currently outpaces the depth of large-scale clinical data. Evidence Synthesis: While pilot trials show "positive outcomes" for vaginal atrophy and SUI, the current evidence base lacks the volume of robust, multi-center RCTs required for standard-of-care status.
Clinical context
Evidence Synthesis: While pilot trials show "positive outcomes" for vaginal atrophy and SUI, the current evidence base lacks the volume of robust, multi-center RCTs required for standard-of-care status.
Evidence
Symptoms
Alternatives
What it means
Evidence Synthesis: While pilot trials show "positive outcomes" for vaginal atrophy and SUI, the current evidence base lacks the volume of robust, multi-center RCTs required for standard-of-care status.
Why it happens
Statistical Nuance: Clinicians should note that while total FSFI scores often show significant improvement, individual subscales for desire, arousal, and lubrication may not reach statistical significance against placebos.
Evidence limits
Standardization: There is an urgent need for standardized preparation protocols (G-force, concentration yields) and long-term longitudinal data to validate early findings.
Treatment fit
Suitability depends on history, symptoms, examination where appropriate and discussion of alternatives.
What this means in practice
PRP administration in the UK is governed by the Medicines and Healthcare products Regulatory Agency (MHRA) and professional regulatory bodies. Regulatory Classification: PRP is classified as an "unlicensed human medicine."
The procedure is a minimally invasive, office-based intervention with high patient compliance and "little downtime." Immediate Recovery: Following venepuncture and targeted injection, patients may resume normal activities almost immediately, though localized tenderness is expected.
Patient safety
Why proper assessment matters
Assessment helps separate marketing claims from safe, individualised clinical decision-making.
It checks the cause
Evidence Synthesis: While pilot trials show "positive outcomes" for vaginal atrophy and SUI, the current evidence base lacks the volume of robust, multi-center RCTs required for standard-of-care status.
It protects safety
Localized pain and pressure at the injection site.
It reviews alternatives
Regulatory Classification: PRP is classified as an "unlicensed human medicine."
It sets expectations
Immediate Recovery: Following venepuncture and targeted injection, patients may resume normal activities almost immediately, though localized tenderness is expected.
A clinical decision, not a shortcut
The safest final page should explain what the intervention may do, what it cannot promise, and when another route may be better.
Treatment should be discussed with realistic goals, informed consent, clear aftercare and a plan for review.
Considerations
What to consider
PRP administration in the UK is governed by the Medicines and Healthcare products Regulatory Agency (MHRA) and professional regulatory bodies. Regulatory Classification: PRP is classified as an "unlicensed human medicine."
Consultation priorities
Diagnostic Consultation: Mandatory assessment with a GMC-registered doctor to confirm suitability and exclude contraindications.
Consent
Aftercare
Follow-up
Before treatment
Diagnostic Consultation: Mandatory assessment with a GMC-registered doctor to confirm suitability and exclude contraindications.
During care
Venepuncture: Collection of 15–30ml of autologous blood using a CE-marked medical device.
Aftercare
Processing: Centrifugation to isolate the "buffy coat" layer, concentrating the platelets for therapeutic use.
When to reassess
Targeted Injection: Precise administration into the clitoral body, anterior vaginal wall (G-spot), or periurethral/labial tissues.
Practical expectations
Immediate Recovery: Following venepuncture and targeted injection, patients may resume normal activities almost immediately, though localized tenderness is expected.
Legal Framework for Administration:
Common concerns and myths
Common misconceptions
Clear patient information should correct over-simple claims and keep expectations realistic.
Myth: Clitoral sensation is only about blood flow.
Reality: suitability depends on the symptom pattern, medical history, contraindications, alternatives and individual goals.
Myth: The O-Shot guarantees stronger clitoral orgasm.
Reality: results vary, evidence may be developing, and non-response should prompt reassessment.
Myth: Numbness should be treated cosmetically without medical assessment.
Reality: injections, devices and intimate procedures can still carry risks and need proper consent and aftercare.
Evidence and advertising
Statistical Nuance: Clinicians should note that while total FSFI scores often show significant improvement, individual subscales for desire, arousal, and lubrication may not reach statistical significance against placebos.
Alternatives
Regulatory Classification: PRP is classified as an "unlicensed human medicine."
Safety checklist
Safety checklist
Use these questions to decide whether treatment should be discussed, delayed or redirected.
Has the cause been assessed?
Symptoms should be reviewed in context before selecting a treatment.
Are red flags absent?
Localized pain and pressure at the injection site.
Are alternatives clear?
Regulatory Classification: PRP is classified as an "unlicensed human medicine."
Is follow-up planned?
The clinic should explain aftercare, review timing and when to seek help.
Reassuring signs
Proceeding is more reasonable when goals are clear, red flags have been checked, and expectations are realistic.
No red flags
Follow-up plan
Reasons to pause
Localized pain and pressure at the injection site.
Bleeding
Infection
When to escalate
When to seek medical help
Some symptoms should be assessed before any elective intimate treatment. Use NHS 111 online
Severe or worsening pain
Localized pain and pressure at the injection site.
Bleeding or discharge
Temporary swelling, redness, or bruising.
Infection signs
Potential for localized infection.
Emergency symptoms
Call 999 in a life-threatening emergency, including collapse, chest pain or breathing difficulty.
Use NHS 111 for urgent advice or call 999 in a life-threatening emergency. This page is educational and does not replace individual medical assessment.
More clinical detail
Benchmark positioning
- This is one of the strongest O-Shot-fit topics, but the winning page must pair anatomy with caution.
Clinical reality
- Evidence Synthesis: While pilot trials show "positive outcomes" for vaginal atrophy and SUI, the current evidence base lacks the volume of robust, multi-center RCTs required for standard-of-care status.
- Statistical Nuance: Clinicians should note that while total FSFI scores often show significant improvement, individual subscales for desire, arousal, and lubrication may not reach statistical significance against placebos in small-sample trials ($n=52$).
- Standardization: There is an urgent need for standardized preparation protocols (G-force, concentration yields) and long-term longitudinal data to validate early findings.
Timeline and expectations
- Immediate Recovery: Following venepuncture and targeted injection, patients may resume normal activities almost immediately, though localized tenderness is expected.
- Clinical Follow-up: Established protocols require assessments at the 6-week mark to evaluate initial response and a comprehensive 6-month follow-up to monitor long-term efficacy.
- Biological Progression: The clinical effect is driven by the immediate release of growth factors—including PDGF, VEGF, EGF, and TGF-β—which initiate angiogenesis and extracellular matrix remodeling.
Practical logistics
- Regulatory Classification: PRP is classified as an "unlicensed human medicine."
- Legal Framework for Administration:
- Doctors (GMC): Are exempt from manufacturing licenses when preparing PRP for a named patient at the point of care.
- Physiotherapists: Cannot manufacture PRP. They may only administer it when directed by a doctor, dentist, nurse independent prescriber, or pharmacist independent prescriber within the same clinical practice.
- Liability: The Chartered Society of Physiotherapy (CSP) explicitly states there is no cover for PRP administration within their standard PLI policy.
- Financial Entry Point: Treatment costs typically start from £1500, as cited by Dr. Sarah Jenkins.
Research sources
- Clarke B et al. Vaginal Injection of Platelet-Rich Plasma for Sexual Function: A Randomized Controlled Trial. Obstet Gynecol. 2026.
- De Ponte A et al. Platelet-rich plasma in the management of vulvovaginal disorders: a systematic review. J Sex Med. 2026.
- Saleh D.M. & Abdelghani R. Clinical evaluation of autologous platelet rich plasma injection in postmenopausal vulvovaginal atrophy. J Cosmet Dermatol. 2022.
- Prodromidou A. et al. The emerging role on the use of platelet rich plasma products in the management of urogynaecological disorders. Surg Innov. 2022.
Regulatory resources
Authoritative resources
These resources support assessment-led, evidence-aware patient information.
NICE interventional procedures guidance
NICE is a UK authority for interventional procedure governance and supports cautious language about evidence, consent and audit.
FDA safety communication on vaginal rejuvenation devices
This safety communication is a useful regulatory reference for avoiding over-claiming around sexual enhancement procedures.
RCOG patient information on menopause symptom treatment
RCOG patient information supports assessment-led discussion of vaginal dryness, discomfort and hormone-related symptoms.
Next step
Book a clinical consultation
A consultation can confirm whether this treatment may be suitable, whether another pathway should come first, and what realistic outcomes and aftercare would look like.
▶ View Full Research Bibliography (10 Sources)
Educational only. This content is for educational and informational purposes only and does not constitute professional medical advice, diagnosis, or treatment. Individual clinical results of autologous therapies vary significantly based on patient biology. A mandatory diagnostic consultation with a registered medical professional is required to determine suitability and assess individual risks before undergoing any PRP-based procedure. Results vary. Not a cure.