Evidence-aware
Safety focused
Women’s Health Clinic FAQ
Can the O-Shot help me orgasm for the first time?
The O-Shot may be worth discussing if reduced genital sensitivity, dryness, discomfort, low-oestrogen tissue change, or blood-flow/tissue-health factors are part of the picture, but it cannot promise a first orgasm. First orgasm difficulty is often multifactorial and may need medical, pelvic floor, medication, hormone, and psychosexual assessment.
Direct answer
The O-Shot may be worth discussing if reduced genital sensitivity, dryness, discomfort, low-oestrogen tissue change, or blood-flow/tissue-health factors are part of the picture, but it cannot promise a first orgasm. First orgasm difficulty is often multifactorial and may need medical, pelvic floor, medication, hormone, and psychosexual assessment.
The most useful plan starts with the underlying cause, not the treatment name. Your clinician should review symptoms, medical history, alternatives, expected benefits, limitations and safety.
Educational only. Suitability must be confirmed after consultation. Results vary. Not a cure.

At a glance
These are the main points to understand before deciding whether this option is suitable.
At a glance
Clinical summary
Improvement Rate
64% of participants demonstrated clinical improvement.
Distress Reduction
Mean FSDS-R (Female Sexual Distress Scale) scores dropped from 17 to 7 (p=0.04).
Overall Function
82% of women showed improved total FSFI scores.
Hyaluronic Acid (Armonía®)
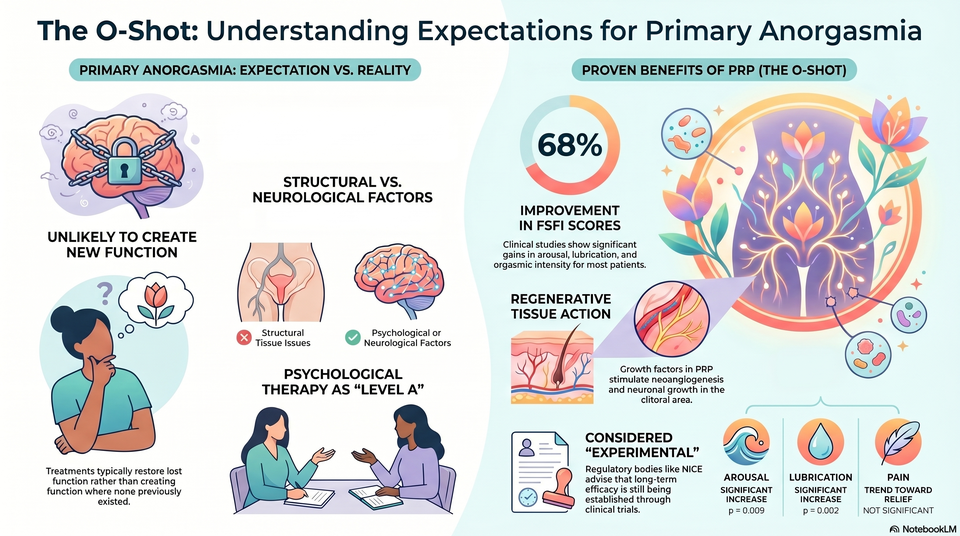
Demonstrated a 68.1% improvement in FSFI scores.
Important safety note
Mild edema (swelling) and localized bruising.
Suitability
Evidence
Safety
Aftercare
Detailed answer
Detailed answer
While marketing for "intimate rejuvenation" is prolific, the clinical reality is defined by a conservative Hierarchy of Care. According to the British Menopause Society (BMS), NICE, and the Royal College of Obstetricians and Gynaecologists (RCOG), injectables are not first-line therapies. The Evidence-Based Standard of Care: Pelvic floor physiotherapy. Topical oestrogens (creams/pessaries) and non-hormonal lubricants.
Clinical context
Pelvic floor physiotherapy.
Evidence
Symptoms
Alternatives
What it means
Pelvic floor physiotherapy.
Why it happens
Topical oestrogens (creams/pessaries) and non-hormonal lubricants.
Evidence limits
Psychosexual Therapy: Identified by the RCOG’s "Tomorrow’s Specialist" document as one of the top three treatments women expect and require for holistic care.
Treatment fit
Suitability depends on history, symptoms, examination where appropriate and discussion of alternatives.
What this means in practice
The procedure requires standardized preparation to ensure both efficacy and patient comfort. Anesthesia: Analgesia is achieved using a specialized compounded topical cream consisting of bupivacaine 20%, lidocaine 8%, and tetracaine 8%, applied 20 minutes prior to the procedure.
The therapeutic window for regenerative injectables is governed by the underlying biological processes of the materials used: Hyaluronic Acid: Onset is immediate, providing mechanical support and increased thickness of the urethrovaginal space upon injection. Platelet-Rich Plasma: Therapeutic effects are typically observed at 12–16 weeks.
Patient safety
Why proper assessment matters
Assessment helps separate marketing claims from safe, individualised clinical decision-making.
It checks the cause
Pelvic floor physiotherapy.
It protects safety
Mild edema (swelling) and localized bruising.
It reviews alternatives
Anesthesia: Analgesia is achieved using a specialized compounded topical cream consisting of bupivacaine 20%, lidocaine 8%, and tetracaine 8%, applied 20 minutes prior to the procedure.
It sets expectations
Hyaluronic Acid: Onset is immediate, providing mechanical support and increased thickness of the urethrovaginal space upon injection.
A clinical decision, not a shortcut
The safest final page should explain what the intervention may do, what it cannot promise, and when another route may be better.
Treatment should be discussed with realistic goals, informed consent, clear aftercare and a plan for review.
Considerations
What to consider
The procedure requires standardized preparation to ensure both efficacy and patient comfort. Anesthesia: Analgesia is achieved using a specialized compounded topical cream consisting of bupivacaine 20%, lidocaine 8%, and tetracaine 8%, applied 20 minutes prior to the procedure. PRP Preparation: A blood draw of 10–60ml undergoes double-spin centrifugation.
Consultation priorities
Satisfaction: Trials report high satisfaction rates (87.5% for HA; 75% for PRP), though the Placebo Effect remains a significant consideration in sexual medicine research.
Consent
Aftercare
Follow-up
Before treatment
Satisfaction: Trials report high satisfaction rates (87.5% for HA; 75% for PRP), though the Placebo Effect remains a significant consideration in sexual medicine research.
During care
Shared Decision-Making: As emphasized by Dr. Farzana Khan, the journey must be rooted in realistic expectations rather than marketing hyperbole.
Aftercare
Paradoxical Distress: Clinicians should screen for distress resulting from a libido increase that exceeds a partner's capacity or desire, creating a relational mismatch despite "successful" physiological treatment.
When to reassess
If expected improvement does not occur, the plan should be reviewed rather than repeated automatically.
Practical expectations
Hyaluronic Acid: Onset is immediate, providing mechanical support and increased thickness of the urethrovaginal space upon injection.
PRP Preparation: A blood draw of 10–60ml undergoes double-spin centrifugation. High-precision systems like TruPRP® utilize a laser device to visualize the buffy coat for optimal platelet concentration.
Common concerns and myths
Common misconceptions
Clear patient information should correct over-simple claims and keep expectations realistic.
Myth: One injection can reliably create a first orgasm.
Reality: suitability depends on the symptom pattern, medical history, contraindications, alternatives and individual goals.
Myth: Not having orgasmed means something is wrong with the patient.
Reality: results vary, evidence may be developing, and non-response should prompt reassessment.
Myth: Vaginal orgasm is the only valid goal.
Reality: injections, devices and intimate procedures can still carry risks and need proper consent and aftercare.
Evidence and advertising
Topical oestrogens (creams/pessaries) and non-hormonal lubricants.
Alternatives
Anesthesia: Analgesia is achieved using a specialized compounded topical cream consisting of bupivacaine 20%, lidocaine 8%, and tetracaine 8%, applied 20 minutes prior to the procedure.
Safety checklist
Safety checklist
Use these questions to decide whether treatment should be discussed, delayed or redirected.
Has the cause been assessed?
Symptoms should be reviewed in context before selecting a treatment.
Are red flags absent?
Mild edema (swelling) and localized bruising.
Are alternatives clear?
Anesthesia: Analgesia is achieved using a specialized compounded topical cream consisting of bupivacaine 20%, lidocaine 8%, and tetracaine 8%, applied 20 minutes prior to the procedure.
Is follow-up planned?
The clinic should explain aftercare, review timing and when to seek help.
Reassuring signs
Proceeding is more reasonable when goals are clear, red flags have been checked, and expectations are realistic.
No red flags
Follow-up plan
Reasons to pause
Mild edema (swelling) and localized bruising.
Bleeding
Infection
When to escalate
When to seek medical help
Some symptoms should be assessed before any elective intimate treatment. Use NHS 111 online
Severe or worsening pain
Mild edema (swelling) and localized bruising.
Bleeding or discharge
Transient burning sensations at the injection site.
Infection signs
Rare "Extreme Sexual Arousal" (resolving within 1–2 weeks), including spontaneous orgasm or arousal during urination.
Emergency symptoms
Call 999 in a life-threatening emergency, including collapse, chest pain or breathing difficulty.
Use NHS 111 for urgent advice or call 999 in a life-threatening emergency. This page is educational and does not replace individual medical assessment.
More clinical detail
Benchmark positioning
- WHC should be the page that gives hope without exploitation: intimate PRP may be one option, but a first orgasm usually needs a wider, respectful assessment.
Clinical reality
- Pelvic floor physiotherapy.
- Topical oestrogens (creams/pessaries) and non-hormonal lubricants.
- Psychosexual Therapy: Identified by the RCOG’s "Tomorrow’s Specialist" document as one of the top three treatments women expect and require for holistic care.
Timeline and expectations
- Hyaluronic Acid: Onset is immediate, providing mechanical support and increased thickness of the urethrovaginal space upon injection.
- Platelet-Rich Plasma: Therapeutic effects are typically observed at 12–16 weeks. This delay corresponds to the biological timeline required for stem cell activation, fibroblast growth, and neoangiogenesis.
- Follow-up: Standard clinical monitoring in pilot trials is established at the 3-month interval to assess peak functional response.
Practical logistics
- Anesthesia: Analgesia is achieved using a specialized compounded topical cream consisting of bupivacaine 20%, lidocaine 8%, and tetracaine 8%, applied 20 minutes prior to the procedure.
- PRP Preparation: A blood draw of 10–60ml undergoes double-spin centrifugation. High-precision systems like TruPRP® utilize a laser device to visualize the buffy coat for optimal platelet concentration.
- Injection Technique:
- PRP: Distributed into the clitoral cavernous body and the anterior vaginal wall submucosa using 27-gauge needles.
- HA: Injected at precise coordinates: 2.5 cm posterior and 2 cm lateral to the mid-urethra into the submucosal layer.
Research sources
- Runels C, et al. (2014). A Pilot Study of the Effect of Localized Injections of Autologous Platelet Rich Plasma (PRP) for the Treatment of Female Sexual Dysfunction. J Women’s Health Care.
- Barber MA, Eguiluz I (2026). Anterior Vaginal Wall Augmentation using Cross-Linked Hyaluronic Acid versus Platelet-Rich Plasma. JSM Sexual Med.
- Pyrgidis N, et al. (2023). Efficacy and Safety of Platelet-Rich Plasma Injections for the Treatment of FSD: A Systematic Review. Biomedicines.
- NICE Interventional Procedure Guidance (IPG615, IPG697; IPG696 for SUI).
Regulatory resources
Authoritative resources
These resources support assessment-led, evidence-aware patient information.
NICE guidance on vaginal laser for urogenital atrophy
NICE is a UK authority for interventional procedure governance and supports cautious language about evidence, consent and audit.
FDA safety communication on vaginal rejuvenation devices
This safety communication is a useful regulatory reference for avoiding over-claiming around sexual enhancement procedures.
RCOG patient information on menopause symptom treatment
RCOG patient information supports assessment-led discussion of vaginal dryness, discomfort and hormone-related symptoms.
Next step
Book a clinical consultation
A consultation can confirm whether this treatment may be suitable, whether another pathway should come first, and what realistic outcomes and aftercare would look like.
▶ View Full Research Bibliography (10 Sources)
Educational only. This document is for educational and clinical synthesis purposes only and does not constitute medical advice. Results of regenerative therapies vary significantly by individual. These procedures remain investigational and are not a substitute for professional diagnosis or the established medical standard of care. Patients must consult with a qualified specialist to explore evidence-based first-line treatments before pursuing injectable interventions. Results vary. Not a cure.