Evidence-aware
Safety focused
Women’s Health Clinic FAQ
Can the O-Shot make orgasms easier to achieve?
The O-Shot may make orgasm easier for some selected patients if reduced sensitivity, dryness, discomfort, tissue changes, or reduced genital arousal are limiting pleasure. It cannot promise easier orgasm, because stimulation pattern, arousal, mental focus, pain, medication, hormones, pelvic floor function, and partner context all matter.
Direct answer
The O-Shot may make orgasm easier for some selected patients if reduced sensitivity, dryness, discomfort, tissue changes, or reduced genital arousal are limiting pleasure. It cannot promise easier orgasm, because stimulation pattern, arousal, mental focus, pain, medication, hormones, pelvic floor function, and partner context all matter.
The most useful plan starts with the underlying cause, not the treatment name. Your clinician should review symptoms, medical history, alternatives, expected benefits, limitations and safety.
Educational only. Suitability must be confirmed after consultation. Results vary. Not a cure.

At a glance
These are the main points to understand before deciding whether this option is suitable.
At a glance
Clinical summary
O-Shot (Orgasm Shot)
The injection of autologous Platelet-Rich Plasma (PRP) into the clitoris and upper vaginal wall.
Vaginal Laser/Radiofrequency (RF)
Energy-based treatments (e. g.
G-Shot
An augmentation procedure involving the injection of hyaluronic acid filler into the anterior vaginal wall (the theoretical G-spot.
Emsella Chair (HIFEM)
A non-invasive device utilizing High-Intensity Focused Electromagnetic (HIFEM) energy to induce supramaximal pelvic floor muscle contractions.
Important safety note
Contraindications: Active infections, pregnancy, and certain medical implants (specifically for energy-based devices).
Suitability
Evidence
Safety
Aftercare
Detailed answer
Detailed answer
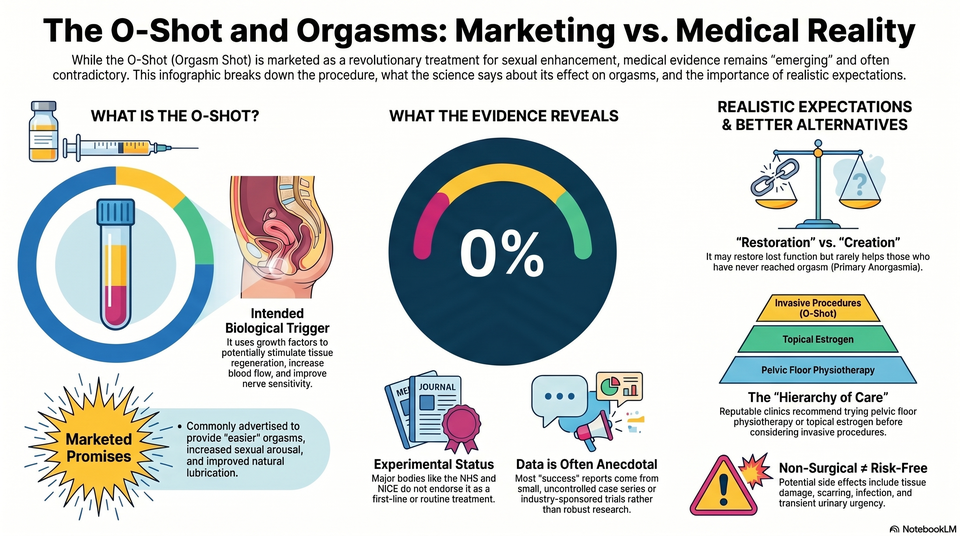
The Primary Anorgasmia Myth: These procedures are restorative rather than "creative." They are highly unlikely to enable orgasms in women who have never experienced them (Primary Anorgasmia), as these cases are often rooted in neurological or psychological factors rather than structural deficits. Marketing vs.
Clinical context
The Primary Anorgasmia Myth: These procedures are restorative rather than "creative."
Evidence
Symptoms
Alternatives
What it means
The Primary Anorgasmia Myth: These procedures are restorative rather than "creative."
Why it happens
Marketing vs. Data: Marketing frequently promises a "climax boost," yet a 2024 cross-sectional analysis of 18 clinical trials (Hunt, R. , et al.)
Evidence limits
Evidence may be developing, so the page should avoid promise-based language and explain uncertainty.
Treatment fit
Suitability depends on history, symptoms, examination where appropriate and discussion of alternatives.
What this means in practice
PRP Preparation: Utilizing a two-spin centrifugation method to isolate the platelet pellet. A validated protocol involves an initial spin at 2500 rpm for 3 minutes, followed by a second spin at 4000 rpm for 15 minutes.
Adhering to clinical governance and British Menopause Society (BMS) standards, practitioners must observe a mandatory Hierarchy of Care (Step-Ladder approach) before proceeding to interventional treatments: First-Line: Lifestyle modifications, pelvic floor physiotherapy, and non-hormonal moisturisers/lubricants. Second-Line: Topical estrogens (creams, pessaries, or rings) for hormonal-related atrophy.
Patient safety
Why proper assessment matters
Assessment helps separate marketing claims from safe, individualised clinical decision-making.
It checks the cause
The Primary Anorgasmia Myth: These procedures are restorative rather than "creative."
It protects safety
Contraindications: Active infections, pregnancy, and certain medical implants (specifically for energy-based devices).
It reviews alternatives
PRP Preparation: Utilizing a two-spin centrifugation method to isolate the platelet pellet.
It sets expectations
First-Line: Lifestyle modifications, pelvic floor physiotherapy, and non-hormonal moisturisers/lubricants.
A clinical decision, not a shortcut
The safest final page should explain what the intervention may do, what it cannot promise, and when another route may be better.
Treatment should be discussed with realistic goals, informed consent, clear aftercare and a plan for review.
Considerations
What to consider
PRP Preparation: Utilizing a two-spin centrifugation method to isolate the platelet pellet. A validated protocol involves an initial spin at 2500 rpm for 3 minutes, followed by a second spin at 4000 rpm for 15 minutes.
Consultation priorities
Clinical Assessment: Identification of root causes (hormonal, psychological, or physical).
Consent
Aftercare
Follow-up
Before treatment
Clinical Assessment: Identification of root causes (hormonal, psychological, or physical).
During care
Conservative Trial: Mandatory attempt of evidence-based standards (Physiotherapy/Topical Estrogens).
Aftercare
Informed Consent: Explicit documentation that the patient understands long-term safety data (>12 months) is limited and results vary.
When to reassess
Procedure: Conducted in a regulated, CQC-registered medical setting.
Practical expectations
First-Line: Lifestyle modifications, pelvic floor physiotherapy, and non-hormonal moisturisers/lubricants.
Analgesia: Topical lidocaine cream must be applied to target areas one hour prior to the procedure.
Common concerns and myths
Common misconceptions
Clear patient information should correct over-simple claims and keep expectations realistic.
Myth: The O-Shot always makes orgasms easier.
Reality: suitability depends on the symptom pattern, medical history, contraindications, alternatives and individual goals.
Myth: If orgasm is difficult, the problem must be local tissue.
Reality: results vary, evidence may be developing, and non-response should prompt reassessment.
Myth: A partner should be able to create orgasm without clitoral.
Reality: injections, devices and intimate procedures can still carry risks and need proper consent and aftercare.
Evidence and advertising
Marketing vs. Data: Marketing frequently promises a "climax boost," yet a 2024 cross-sectional analysis of 18 clinical trials (Hunt, R. , et al.)
Alternatives
PRP Preparation: Utilizing a two-spin centrifugation method to isolate the platelet pellet.
Safety checklist
Safety checklist
Use these questions to decide whether treatment should be discussed, delayed or redirected.
Has the cause been assessed?
Symptoms should be reviewed in context before selecting a treatment.
Are red flags absent?
Contraindications: Active infections, pregnancy, and certain medical implants (specifically for energy-based devices).
Are alternatives clear?
PRP Preparation: Utilizing a two-spin centrifugation method to isolate the platelet pellet.
Is follow-up planned?
The clinic should explain aftercare, review timing and when to seek help.
Reassuring signs
Proceeding is more reasonable when goals are clear, red flags have been checked, and expectations are realistic.
No red flags
Follow-up plan
Reasons to pause
Contraindications: Active infections, pregnancy, and certain medical implants (specifically for energy-based devices).
Bleeding
Infection
When to escalate
When to seek medical help
Some symptoms should be assessed before any elective intimate treatment. Use NHS 111 online
Severe or worsening pain
Contraindications: Active infections, pregnancy, and certain medical implants (specifically for energy-based devices).
Bleeding or discharge
Clinical Red Flags: Immediate GP referral is required if the patient experiences:
Infection signs
Sudden loss of genital sensation.
Emergency symptoms
Call 999 in a life-threatening emergency, including collapse, chest pain or breathing difficulty.
Use NHS 111 for urgent advice or call 999 in a life-threatening emergency. This page is educational and does not replace individual medical assessment.
More clinical detail
Benchmark positioning
- The strongest page should combine the commercial promise patients are searching for with WHC-grade limits and assessment.
Clinical reality
- The Primary Anorgasmia Myth: These procedures are restorative rather than "creative."
- Marketing vs. Data: Marketing frequently promises a "climax boost," yet a 2024 cross-sectional analysis of 18 clinical trials (Hunt, R. , et al.) found no statistically significant improvements in sexual satisfaction or arousal.
Timeline and expectations
- First-Line: Lifestyle modifications, pelvic floor physiotherapy, and non-hormonal moisturisers/lubricants.
- Second-Line: Topical estrogens (creams, pessaries, or rings) for hormonal-related atrophy.
- Interventional: Regenerative or energy-based procedures are considered only when first- and second-line therapies are contraindicated or have failed to provide relief.
- Treatment Frequency: Protocols vary; energy-based devices and PRP typically require 1–4 sessions spaced 4–6 weeks apart.
- Observation Window: Therapeutic effects attributed to stem cell activation and tissue transformation are standardized for assessment at the 12-week (3-month) mark.
- Duration: Benefits are often temporary. Hyaluronic fillers (G-Shot) last only a few months, and regenerative results usually require annual maintenance.
Practical logistics
- PRP Preparation: Utilizing a two-spin centrifugation method to isolate the platelet pellet.
- Analgesia: Topical lidocaine cream must be applied to target areas one hour prior to the procedure.
- Injection Technique (O-Shot): Using a 31G needle, the clinician creates a ring of PRP "blebs" at the cardinal points (12, 3, 6, and 9 o'clock) around the clitoral shaft.
- Post-Procedure Restrictions: Patients must avoid sexual intercourse for 2–3 days and refrain from baths or swimming pools for several days.
Research sources
- Hunt, R., et al. (2024): Cross-sectional analysis of 18 trials; confirmed no statistically significant improvements in arousal or satisfaction domains.
- Salam, K. A. , et al. (2022): Retrospective cohort study (n=30) reported significant improvements in sexual distress and function at 4 months. Quantitative metrics included a 72% increase in total FSFI scores (16.
- Sukgen, G., et al. (2023): Prospective study reporting a 60% improvement in orgasmic function following a 4-session PRP protocol.
- NICE IPG696/697: Mandates that these procedures only be performed under special arrangements for clinical governance, including formal audit.
Regulatory resources
Authoritative resources
These resources support assessment-led, evidence-aware patient information.
NICE guidance on vaginal laser for urogenital atrophy
NICE is a UK authority for interventional procedure governance and supports cautious language about evidence, consent and audit.
FDA safety communication on vaginal rejuvenation devices
This safety communication is a useful regulatory reference for avoiding over-claiming around sexual enhancement procedures.
RCOG patient information on menopause symptom treatment
RCOG patient information supports assessment-led discussion of vaginal dryness, discomfort and hormone-related symptoms.
Next step
Book a clinical consultation
A consultation can confirm whether this treatment may be suitable, whether another pathway should come first, and what realistic outcomes and aftercare would look like.
▶ View Full Research Bibliography (10 Sources)
Educational only. This report is for educational purposes only and does not constitute medical advice. Results of regenerative and energy-based procedures vary by individual. These treatments are not a substitute for clinical assessment and should only be considered following a full clinical assessment by a qualified medical professional. Always consult your GP or a specialist for symptoms requiring urgent review. Results vary. Not a cure.