Evidence-aware
Safety focused
Women’s Health Clinic FAQ
Can the O-Shot improve arousal?
Arousal is both a brain-body experience and a genital response. The O-Shot may support physical arousal in selected patients by improving comfort, lubrication, sensitivity, or tissue response, but it cannot force desire or emotional arousal and should be assessed alongside hormones, stress, pain, medication, and relationship context.
Direct answer
Arousal is both a brain-body experience and a genital response. The O-Shot may support physical arousal in selected patients by improving comfort, lubrication, sensitivity, or tissue response, but it cannot force desire or emotional arousal and should be assessed alongside hormones, stress, pain, medication, and relationship context.
The most useful plan starts with the underlying cause, not the treatment name. Your clinician should review symptoms, medical history, alternatives, expected benefits, limitations and safety.
Educational only. Suitability must be confirmed after consultation. Results vary. Not a cure.

At a glance
These are the main points to understand before deciding whether this option is suitable.
At a glance
Clinical summary
Superficial (Entry) Pain
Localized to the vulva or vaginal introitus.
Deep (Collision) Pain
Experienced higher in the vaginal vault or pelvic cavity during thrusting.
Key point 3
Patients with severe vasomotor or psychological symptoms that persist despite standard oral or transdermal HRT.
Key point 4
Younger patients in surgical menopause requiring higher estradiol levels for bone protection.
Important safety note
Hemorrhage: Vaginal bleeding that soaks one sanitary pad per hour for two consecutive hours.
Suitability
Evidence
Safety
Aftercare
Detailed answer
Detailed answer
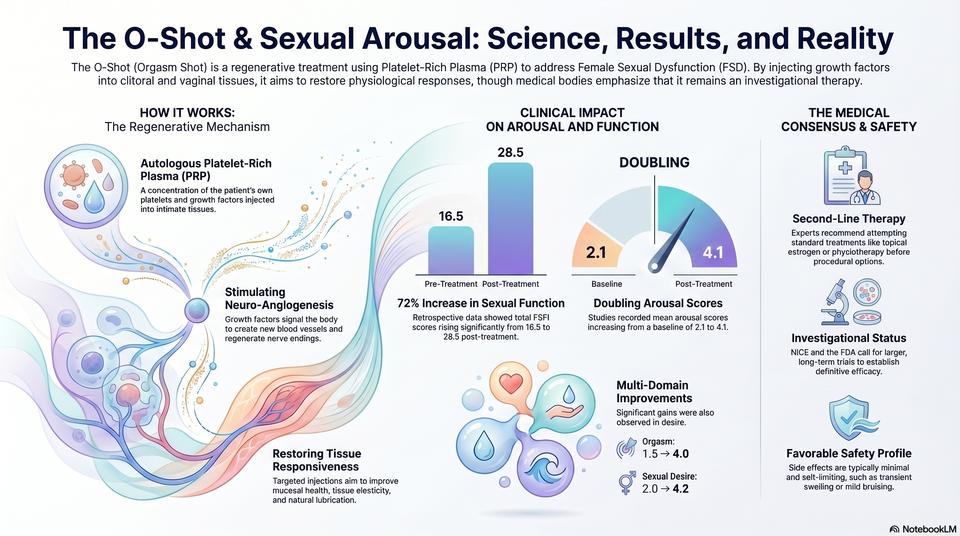
The clinical evidence for regenerative modalities remains a subject of significant debate within the gynaecological community. Evidence Synthesis: The systematic review by Ismail et al. (2025) reported statistically significant improvements in Female Sexual Function Index (FSFI) scores, specifically noting a 20–60% increase in the vaginal lubrication domain.
Clinical context
Evidence Synthesis: The systematic review by Ismail et al.
Evidence
Symptoms
Alternatives
What it means
Evidence Synthesis: The systematic review by Ismail et al.
Why it happens
Methodological Concerns: Critics highlight that the "O-Shot®" protocol stems from questionable origins.
Evidence limits
NICE Regulatory Position:
Treatment fit
IPG615: States evidence on efficacy for energy devices is "limited in quantity and quality."
What this means in practice
Post-Procedural Abstinence Vaginal Laser: 5 to 7 days of pelvic rest to allow microscopic treatment channels to heal. PRP (O-Shot): 24 hours of abstinence to allow injection points to seal.
Clinicians must set realistic expectations based on established biological healing and remodeling markers: Regenerative Remodeling: Following PRP or energy-based treatments, collagen remodeling and tissue repair typically peak at 12 weeks.
Patient safety
Why proper assessment matters
Assessment helps separate marketing claims from safe, individualised clinical decision-making.
It checks the cause
Evidence Synthesis: The systematic review by Ismail et al.
It protects safety
Hemorrhage: Vaginal bleeding that soaks one sanitary pad per hour for two consecutive hours.
It reviews alternatives
Vaginal Laser: 5 to 7 days of pelvic rest to allow microscopic treatment channels to heal.
It sets expectations
Regenerative Remodeling: Following PRP or energy-based treatments, collagen remodeling and tissue repair typically peak at 12 weeks.
A clinical decision, not a shortcut
The safest final page should explain what the intervention may do, what it cannot promise, and when another route may be better.
Treatment should be discussed with realistic goals, informed consent, clear aftercare and a plan for review.
Considerations
What to consider
Post-Procedural Abstinence Vaginal Laser: 5 to 7 days of pelvic rest to allow microscopic treatment channels to heal. PRP (O-Shot): 24 hours of abstinence to allow injection points to seal.
Consultation priorities
Green: Proceed with the exam.
Consent
Aftercare
Follow-up
Before treatment
Green: Proceed with the exam.
During care
Amber: Pause or slow down.
Aftercare
Red: Stop the examination immediately.
When to reassess
The Pain Map: History-taking utilizes sensory descriptors to distinguish between nerve-related "burning," structural "bruising/aching," or muscle-spasm "hitting a wall."
Practical expectations
Regenerative Remodeling: Following PRP or energy-based treatments, collagen remodeling and tissue repair typically peak at 12 weeks.
PRP (O-Shot): 24 hours of abstinence to allow injection points to seal.
Common concerns and myths
Common misconceptions
Clear patient information should correct over-simple claims and keep expectations realistic.
Myth: Arousal is purely physical.
Reality: suitability depends on the symptom pattern, medical history, contraindications, alternatives and individual goals.
Myth: The O-Shot can make someone want sex.
Reality: results vary, evidence may be developing, and non-response should prompt reassessment.
Myth: Lubrication alone equals arousal.
Reality: injections, devices and intimate procedures can still carry risks and need proper consent and aftercare.
Evidence and advertising
Methodological Concerns: Critics highlight that the "O-Shot®" protocol stems from questionable origins.
Alternatives
Vaginal Laser: 5 to 7 days of pelvic rest to allow microscopic treatment channels to heal.
Safety checklist
Safety checklist
Use these questions to decide whether treatment should be discussed, delayed or redirected.
Has the cause been assessed?
Symptoms should be reviewed in context before selecting a treatment.
Are red flags absent?
Hemorrhage: Vaginal bleeding that soaks one sanitary pad per hour for two consecutive hours.
Are alternatives clear?
Vaginal Laser: 5 to 7 days of pelvic rest to allow microscopic treatment channels to heal.
Is follow-up planned?
The clinic should explain aftercare, review timing and when to seek help.
Reassuring signs
Proceeding is more reasonable when goals are clear, red flags have been checked, and expectations are realistic.
No red flags
Follow-up plan
Reasons to pause
Hemorrhage: Vaginal bleeding that soaks one sanitary pad per hour for two consecutive hours.
Bleeding
Infection
When to escalate
When to seek medical help
Some symptoms should be assessed before any elective intimate treatment. Use NHS 111 online
Severe or worsening pain
Hemorrhage: Vaginal bleeding that soaks one sanitary pad per hour for two consecutive hours.
Bleeding or discharge
"Thunderclap" Pain: Sudden, severe pelvic pain, with or without vomiting, which may indicate Ovarian Torsion.
Infection signs
Cauda Equina Signs: New-onset saddle anesthesia (numbness in the groin/buttocks) or loss of bladder/bowel control.
Emergency symptoms
Call 999 in a life-threatening emergency, including collapse, chest pain or breathing difficulty.
Use NHS 111 for urgent advice or call 999 in a life-threatening emergency. This page is educational and does not replace individual medical assessment.
More clinical detail
Benchmark positioning
- The benchmark should be the clearest page for patients who use arousal to mean several different things.
Clinical reality
- Evidence Synthesis: The systematic review by Ismail et al. (2025) reported statistically significant improvements in Female Sexual Function Index (FSFI) scores, specifically noting a 20–60% increase in the vaginal lubrication domain.
- Methodological Concerns: Critics highlight that the "O-Shot®" protocol stems from questionable origins.
- NICE Regulatory Position:
- IPG615: States evidence on efficacy for energy devices is "limited in quantity and quality."
- IPG696 & IPG697: Evidence for long-term safety is "inadequate." These are third-line interventions and require "special arrangements" for clinical governance, mandatory audits, and specific consent regarding the uncertainty of long-term results.
Timeline and expectations
- Regenerative Remodeling: Following PRP or energy-based treatments, collagen remodeling and tissue repair typically peak at 12 weeks.
- Nerve Regeneration: For patients seeking restoration of sensation, nerve regeneration occurs at a physiological rate of approximately 1mm per day.
- Pelvic Physiotherapy: Meaningful change in pelvic floor muscle tone and the "down-training" of hypertonicity generally requires 8 to 12 weeks of consistent therapeutic intervention.
- Treatment Frequency: Procedural protocols for PRP (the "O-Shot®") are heterogeneous, ranging from a single dose to four sessions spaced over 4–6 weeks, depending on the clinical presentation and protocol.
Practical logistics
- Vaginal Laser: 5 to 7 days of pelvic rest to allow microscopic treatment channels to heal.
- PRP (O-Shot): 24 hours of abstinence to allow injection points to seal.
- The "Jug Trick": Patients should pour lukewarm water over the vulva while urinating to prevent stinging on treated tissue.
- Side Effects: Expect transient swelling ("puffy" appearance), localized spotting, or a sensation of fullness for 1–2 days.
Research sources
- Ismail, M. A., et al. (2025). "Role of Platelet-Rich Plasma in Female Sexual Health and Recovery: A Systematic Review." Revista Iberoamericana de Psicología del Ejercicio y el Deporte.
- NICE Interventional Procedure Guidance IPG615 (2018). "Microwave treatment for severe menopausal symptoms."
- Salam, K. A., et al. (2022). "Value of injection of plasma-rich platelets in the vaginal and the clitoris in cases with female sexual dysfunction." Ginekologia i Położnictwo.
- Runels, C., et al. (2014). "A pilot study of the effect of localized injections of autologous platelet rich plasma (PRP) for the treatment of female sexual dysfunction." Journal of Women’s Health Care.
Regulatory resources
Authoritative resources
These resources support assessment-led, evidence-aware patient information.
NICE guidance on vaginal laser for urogenital atrophy
NICE is a UK authority for interventional procedure governance and supports cautious language about evidence, consent and audit.
FDA safety communication on vaginal rejuvenation devices
This safety communication is a useful regulatory reference for avoiding over-claiming around sexual enhancement procedures.
RCOG patient information on menopause symptom treatment
RCOG patient information supports assessment-led discussion of vaginal dryness, discomfort and hormone-related symptoms.
Next step
Book a clinical consultation
A consultation can confirm whether this treatment may be suitable, whether another pathway should come first, and what realistic outcomes and aftercare would look like.
▶ View Full Research Bibliography (10 Sources)
Educational only. This clinical report is provided for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. Individual suitability for any medical or procedural intervention must be determined by a qualified clinician following a formal consultation. Clinical results vary significantly between patients and these treatments do not constitute a "cure" for underlying chronic conditions. Always seek the advice of a healthcare provider regarding medical concerns. Results vary. Not a cure.