Evidence-aware
Safety focused
Women’s Health Clinic FAQ
Can the O-Shot improve sexual desire?
Sexual desire is not the same as genital sensitivity. The O-Shot may indirectly improve desire if discomfort, dryness, low confidence, or reduced sensation are making sex feel unrewarding or avoidable, but desire can be affected by hormones, mood, relationship context, medication, pain, trauma, fatigue, body image, and stress.
Direct answer
Sexual desire is not the same as genital sensitivity. The O-Shot may indirectly improve desire if discomfort, dryness, low confidence, or reduced sensation are making sex feel unrewarding or avoidable, but desire can be affected by hormones, mood, relationship context, medication, pain, trauma, fatigue, body image, and stress.
The most useful plan starts with the underlying cause, not the treatment name. Your clinician should review symptoms, medical history, alternatives, expected benefits, limitations and safety.
Educational only. Suitability must be confirmed after consultation. Results vary. Not a cure.

At a glance
These are the main points to understand before deciding whether this option is suitable.
At a glance
Clinical summary
Multifactorial Triage
Assessment requires a detailed "Pain Map" and clinical history, which provides 80% of diagnostic clues.
Gold Standard First-Line Treatments
Gold Standard First-Line Treatments:
Local Vaginal Oestrogen
The primary intervention for Genitourinary Syndrome of Menopause (GSM).
Specialist Pelvic Physiotherapy
Focuses on "down-training" hypertonic muscles and internal myofascial release.
Important safety note
Hemorrhage: Soaking one pad per hour for two consecutive hours.
Suitability
Evidence
Safety
Aftercare
Detailed answer
Detailed answer
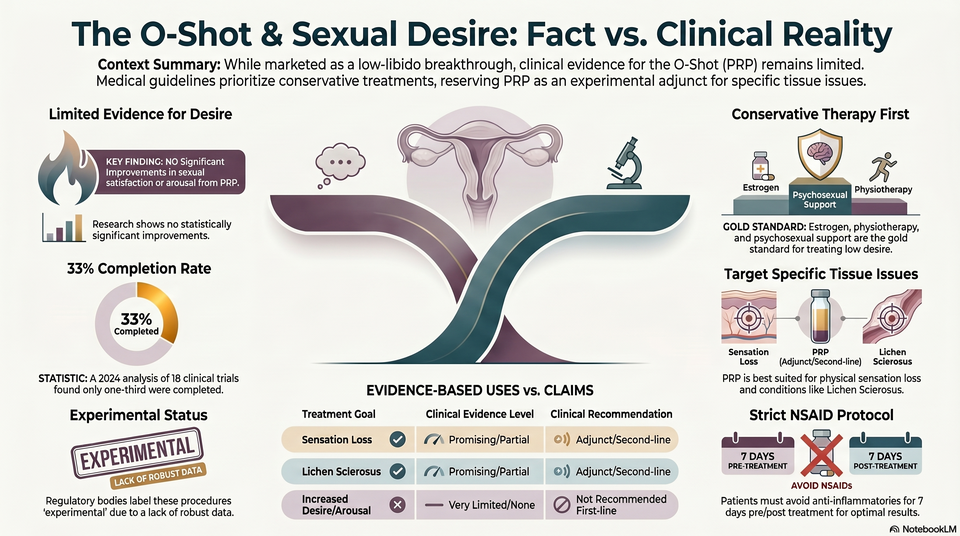
The PRP Evidence Gap: Hunt et al. (2024) found that while PRP is marketed for improved sexual arousal and satisfaction, registered clinical trials show no statistically significant improvements in these outcomes. Bioethical Framework: Using the Nuffield Council on Bioethics lens, the marketing of PRP presents a challenge to informed consent.
Clinical context
The PRP Evidence Gap: Hunt et al.
Evidence
Symptoms
Alternatives
What it means
The PRP Evidence Gap: Hunt et al.
Why it happens
Bioethical Framework: Using the Nuffield Council on Bioethics lens, the marketing of PRP presents a challenge to informed consent.
Evidence limits
The "SHBG Trap": Oral oestrogens and combined contraceptives increase Sex Hormone-Binding Globulin (SHBG), which binds free testosterone and induces tissue thinning (vestibulodynia) and low libido.
Treatment fit
The G-Spot Myth: Scientific data fails to verify the G-spot as a distinct anatomical zone; neuroscientists describe it as a "gynaecologic UFO."
What this means in practice
Administration Protocols: Tostran (2% gel): Starting dose is 1 metered pump (0. 5g/10mg) on alternate days. Testogel (40. 5mg/2. 5g sachet): Starting dose is 1/8 of a sachet daily (approx. 5mg). AndroFeme 1 (1% cream): Starting dose is 0. 5ml daily (5mg).
Clinical recovery in sexual dysfunction is a longitudinal process. Pelvic Physiotherapy: True muscle remodeling and desensitization typically require 8–12 weeks of consistent intervention. Testosterone Replacement Therapy (TRT): A trial of 3–6 months is mandatory to evaluate efficacy for HSDD.
Patient safety
Why proper assessment matters
Assessment helps separate marketing claims from safe, individualised clinical decision-making.
It checks the cause
The PRP Evidence Gap: Hunt et al.
It protects safety
Hemorrhage: Soaking one pad per hour for two consecutive hours.
It reviews alternatives
Tostran (2% gel): Starting dose is 1 metered pump (0.5g/10mg) on alternate days.
It sets expectations
Pelvic Physiotherapy: True muscle remodeling and desensitization typically require 8–12 weeks of consistent intervention.
A clinical decision, not a shortcut
The safest final page should explain what the intervention may do, what it cannot promise, and when another route may be better.
Treatment should be discussed with realistic goals, informed consent, clear aftercare and a plan for review.
Considerations
What to consider
Administration Protocols: Tostran (2% gel): Starting dose is 1 metered pump (0. 5g/10mg) on alternate days. Testogel (40. 5mg/2. 5g sachet): Starting dose is 1/8 of a sachet daily (approx. 5mg). AndroFeme 1 (1% cream): Starting dose is 0. 5ml daily (5mg).
Consultation priorities
pH Diagnostics: pH 4.5 suggests Bacterial Vaginosis (BV).
Consent
Aftercare
Follow-up
Before treatment
pH Diagnostics: pH 4.5 suggests Bacterial Vaginosis (BV).
During care
Q-Tip Test: Identifies localized nerve hypersensitivity (allodynia) at the vestibule.
Aftercare
Single-Digit Palpation: Checks for pelvic floor hypertonicity.
When to reassess
If expected improvement does not occur, the plan should be reviewed rather than repeated automatically.
Practical expectations
Pelvic Physiotherapy: True muscle remodeling and desensitization typically require 8–12 weeks of consistent intervention.
Testogel (40.5mg/2.5g sachet): Starting dose is 1/8 of a sachet daily (approx. 5mg).
Common concerns and myths
Common misconceptions
Clear patient information should correct over-simple claims and keep expectations realistic.
Myth: Desire can be injected into tissue.
Reality: suitability depends on the symptom pattern, medical history, contraindications, alternatives and individual goals.
Myth: If sensation improves, desire automatically returns.
Reality: results vary, evidence may be developing, and non-response should prompt reassessment.
Myth: Low desire is always hormonal.
Reality: injections, devices and intimate procedures can still carry risks and need proper consent and aftercare.
Evidence and advertising
Bioethical Framework: Using the Nuffield Council on Bioethics lens, the marketing of PRP presents a challenge to informed consent.
Alternatives
Tostran (2% gel): Starting dose is 1 metered pump (0.5g/10mg) on alternate days.
Safety checklist
Safety checklist
Use these questions to decide whether treatment should be discussed, delayed or redirected.
Has the cause been assessed?
Symptoms should be reviewed in context before selecting a treatment.
Are red flags absent?
Hemorrhage: Soaking one pad per hour for two consecutive hours.
Are alternatives clear?
Tostran (2% gel): Starting dose is 1 metered pump (0.5g/10mg) on alternate days.
Is follow-up planned?
The clinic should explain aftercare, review timing and when to seek help.
Reassuring signs
Proceeding is more reasonable when goals are clear, red flags have been checked, and expectations are realistic.
No red flags
Follow-up plan
Reasons to pause
Hemorrhage: Soaking one pad per hour for two consecutive hours.
Bleeding
Infection
When to escalate
When to seek medical help
Some symptoms should be assessed before any elective intimate treatment. Use NHS 111 online
Severe or worsening pain
Hemorrhage: Soaking one pad per hour for two consecutive hours.
Bleeding or discharge
"Thunderclap" Pain: Sudden, severe pelvic pain +/- vomiting (potential Ovarian Torsion).
Infection signs
Cauda Equina Signs: Saddle anesthesia (numbness in the groin/buttocks) or loss of bladder/bowel control.
Emergency symptoms
Call 999 in a life-threatening emergency, including collapse, chest pain or breathing difficulty.
Use NHS 111 for urgent advice or call 999 in a life-threatening emergency. This page is educational and does not replace individual medical assessment.
More clinical detail
Benchmark positioning
- This page should refuses lazy libido marketing and gives women a more accurate map of desire.
Clinical reality
- The PRP Evidence Gap: Hunt et al. (2024) found that while PRP is marketed for improved sexual arousal and satisfaction, registered clinical trials show no statistically significant improvements in these outcomes.
- Bioethical Framework: Using the Nuffield Council on Bioethics lens, the marketing of PRP presents a challenge to informed consent.
- The "SHBG Trap": Oral oestrogens and combined contraceptives increase Sex Hormone-Binding Globulin (SHBG), which binds free testosterone and induces tissue thinning (vestibulodynia) and low libido.
- The G-Spot Myth: Scientific data fails to verify the G-spot as a distinct anatomical zone; neuroscientists describe it as a "gynaecologic UFO."
Timeline and expectations
- Pelvic Physiotherapy: True muscle remodeling and desensitization typically require 8–12 weeks of consistent intervention.
- Testosterone Replacement Therapy (TRT): A trial of 3–6 months is mandatory to evaluate efficacy for HSDD. If no clinical improvement is noted by 6 months, therapy should be discontinued.
- Post-Procedural Recovery:
- Vaginal Laser: 5–7 days of sexual abstinence to allow microscopic channels to heal.
- PRP (O-Shot): 24 hours of abstinence to ensure entry point sealing.
- The NSAID Nuance:
Practical logistics
- Tostran (2% gel): Starting dose is 1 metered pump (0.5g/10mg) on alternate days.
- Testogel (40.5mg/2.5g sachet): Starting dose is 1/8 of a sachet daily (approx. 5mg).
- AndroFeme 1 (1% cream): Starting dose is 0.5ml daily (5mg).
- Site Management: Apply to clean, dry skin on the lower abdomen or thighs; rotate sites to avoid localized hirsutism. Wash hands immediately; avoid skin-to-skin contact with others until dry.
- Timing: Samples must be collected in the morning prior to application. Collection within 2–3 hours post-dose is not recommended due to peak/trough variability.
- Schedule: Baseline, 3-month review, and annual testing. Mandatory Rule: No further prescriptions should be issued at the 3-month or annual marks until blood results are reviewed.
Research sources
- Hunt, R., et al. (2024). Evaluating Clinical Trials using Platelet-Rich Plasma to Treat Female Sexual Dysfunction. 2024 Symposium on Tribal and Rural Innovations.
- Gibbons, S. M., et al. (2025). Optimising testosterone therapy in patients with hypoactive sexual desire disorder. British Journal of General Practice.
- Nuffield Council on Bioethics (2018). Bioethics briefing note: Patient access to experimental treatments.
- The Women's Health Clinic (2025). Clinical Practice Guideline: Assessment and Management of Dyspareunia.
Regulatory resources
Authoritative resources
These resources support assessment-led, evidence-aware patient information.
NICE guidance on vaginal laser for urogenital atrophy
NICE is a UK authority for interventional procedure governance and supports cautious language about evidence, consent and audit.
FDA safety communication on vaginal rejuvenation devices
This safety communication is a useful regulatory reference for avoiding over-claiming around sexual enhancement procedures.
RCOG patient information on menopause symptom treatment
RCOG patient information supports assessment-led discussion of vaginal dryness, discomfort and hormone-related symptoms.
Next step
Book a clinical consultation
A consultation can confirm whether this treatment may be suitable, whether another pathway should come first, and what realistic outcomes and aftercare would look like.
▶ View Full Research Bibliography (10 Sources)
Educational only. This report is for educational and informational purposes only and does not constitute medical advice, diagnosis, or treatment. Clinical suitability for any procedure or medication mentioned must be determined by a qualified healthcare professional. For medical emergencies, contact NHS 111 or 999 immediately. Results vary. Not a cure.