Why is sex painful after childbirth—scar tissue vs muscle tension vs dryness?
Pain during sex after childbirth is common and usually results from a combination of physical changes. The three main causes are perineal scar tissue from tears or episiotomy, protective muscle tension in the pelvic floor, and hormonal dryness—especially during breastfeeding when oestrogen levels drop significantly. Each cause produces different sensations and requires tailored treatment, but all are treatable with the right support.
Show Detailed Answer
Postpartum dyspareunia affects approximately 45–60% of women in the first three months after birth, and for many it persists well beyond six months. The pain can feel like burning, tearing, or deep aching, and it often leads to anxiety about intimacy, relationship strain, and feelings of inadequacy or guilt. Understanding the specific cause is the first step toward effective treatment.
Childbirth profoundly changes the pelvic tissues. The vagina and perineum stretch during delivery, sometimes tearing or being cut. Hormones shift dramatically, particularly if you are breastfeeding. The pelvic floor muscles may weaken, overcompensate, or develop protective “guarding” patterns. Each of these changes can contribute to pain, and often more than one factor is at play.
Cause 1: Scar Tissue (Perineal Trauma)
During vaginal birth, the perineum—the area between the vagina and anus—often tears or is surgically cut (episiotomy). As this heals, scar tissue forms. Scar tissue is less elastic than normal skin and can create tight, tender “bands” that pull or sting during penetration.
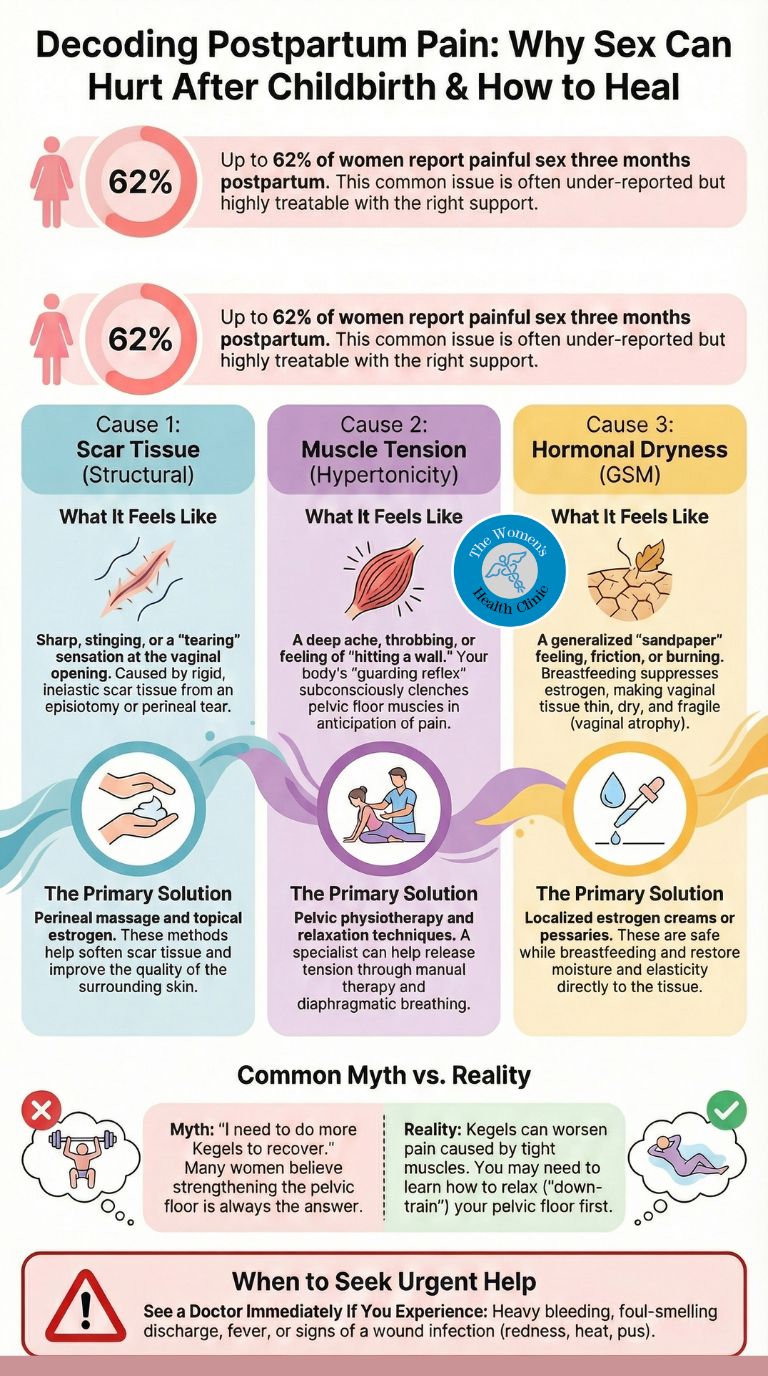
- What it feels like: Sharp, localised pain at the vaginal opening or perineum, especially with initial penetration. Some describe it as a “ripping” or “tearing” sensation at the scar site.
- Why it happens: Scars are made of dense collagen fibres that don’t stretch like healthy tissue. Poor healing, infection, or deep tears increase the likelihood of painful scarring.
- Risk factors: Assisted delivery (forceps, ventouse), large baby, rapid delivery, or previous scarring.
Cause 2: Pelvic Floor Muscle Tension (Vaginismus)
After birth, the pelvic floor muscles may become over-active or “guarded” to protect against pain or further injury. This involuntary tightening, sometimes called secondary vaginismus, makes the vaginal opening narrow and resistant to penetration.
- What it feels like: A “wall” or “clenching” sensation at the entrance, as if the vagina won’t open. Penetration may be impossible or only achievable with significant discomfort.
- Why it happens: Pain during or after birth creates a fear-pain cycle. The brain anticipates pain and signals the muscles to contract protectively, even when there is no current threat.
- Associated symptoms: Difficulty inserting tampons, discomfort during smear tests, or generalised pelvic tension.
Cause 3: Vaginal Dryness (Hormonal Atrophy)
Oestrogen levels plummet after childbirth and remain low throughout breastfeeding. Oestrogen keeps vaginal tissues thick, elastic, and well-lubricated. Without it, the vaginal lining becomes thin, fragile, and dry—a condition called vaginal atrophy or Genitourinary Syndrome of Menopause (GSM), though it affects new mothers too.
- What it feels like: Burning, rawness, or friction pain throughout intercourse. The vagina may feel “tight” but in a dry, uncomfortable way rather than muscular.
- Why it happens: Prolactin (the breastfeeding hormone) suppresses oestrogen production. This is nature’s way of delaying fertility but has the side effect of reducing vaginal health.
- Duration: Symptoms typically improve after weaning, but some women continue to experience dryness if they don’t resume normal hormonal cycling.
How to Tell Them Apart
While these causes often overlap, certain clues can help identify the dominant issue:
- Scar tissue: Pain is localised to a specific spot you can often feel or see. It may improve with scar massage or positional changes.
- Muscle tension: Pain is more diffuse at the entrance, varies with stress or anxiety, and may improve with relaxation techniques or pelvic physiotherapy.
- Dryness: Pain is widespread, worse without lubrication, and often accompanied by itching, soreness, or a “sandpaper” feeling. It typically improves with topical oestrogen.
Common Concerns & Myths
“Should sex feel normal by six weeks postpartum?”
No. The six-week check is about medical safety, not sexual comfort. Many women need months—or specialist support—before sex feels comfortable again. There is no “normal” timeline.
“Is it because my vagina is ‘loose’ now?”
No. Pain after childbirth is not caused by looseness. In fact, overly tight muscles or scar tissue are far more common causes. The idea that the vagina is “ruined” by birth is a harmful myth.
“Will it hurt forever?”
No. With the right combination of scar massage, pelvic physiotherapy, lubrication, and—if needed—topical oestrogen, the vast majority of women experience significant improvement or complete resolution.
Clinical Context
Postpartum sexual pain is under-reported and under-treated, yet it is one of the most common complications of childbirth. Studies show that up to 62% of women report dyspareunia at three months postpartum, with rates remaining elevated at 12 months, particularly in those who had instrumental deliveries or significant tears. The psychological impact—including postnatal depression, relationship distress, and loss of sexual identity—can be profound. Early intervention with pelvic health physiotherapy and appropriate hormonal support significantly improves outcomes. Educational only. Results vary. Not a cure.
Evidence-Based Approaches
Self-Care & Lifestyle
Initial steps focus on reducing friction, calming the nervous system, and allowing tissues time to heal.
- Lubrication: Use generous amounts of a high-quality, water-based or oil-based lubricant. Reapply as needed. Avoid anything with glycerin, parabens, or fragrance.
- Pacing: Prioritise non-penetrative intimacy. When ready, try shallow penetration first, using positions that allow you to control depth and speed.
- Scar Massage: From around six weeks postpartum (once bleeding has stopped and wounds are closed), gentle massage of perineal scars can improve elasticity. Use vitamin E oil or a plain moisturiser and apply light pressure in circular motions for 5–10 minutes daily.
- Pelvic Floor Relaxation: Practice diaphragmatic breathing and reverse Kegels (gently “bulging” the pelvic floor on inhale) to release tension. Avoid doing traditional Kegels if you have overactive muscles.
Medical & Specialist Options
When self-care is not enough, targeted medical and therapeutic interventions are highly effective.
- Pelvic Health Physiotherapy: A specialist women’s health physio can assess scar tissue, muscle tone, and pelvic floor coordination. Treatment includes manual therapy, desensitisation, dilator training, and biofeedback. This is the gold standard for postpartum pain.
- Topical Oestrogen: If you are breastfeeding or have vaginal atrophy, localised oestrogen cream or pessaries restore tissue health. Safe during breastfeeding as absorption is minimal.
- Scar Revision or Injection: In cases of severe or painful scarring, a gynaecologist may offer steroid injections or minor surgical revision to release tight bands.
- Psychosexual Therapy: Addresses the emotional and relational impact of pain, helping to break the fear-pain-avoidance cycle.
For a comprehensive, integrated approach to postpartum intimacy concerns, you can view our step-by-step treatment plan. If you’re ready to take the next step, you can book a consultation with our specialist team.
Red Flags (When to Seek Urgent Review)
Contact your GP or maternity unit immediately if you experience heavy bleeding, foul-smelling discharge, fever, severe pelvic pain, or signs of wound infection such as redness, heat, or pus at the perineal site.
External Resources:
Educational only. Results vary. Not a cure.
Diagnosis First: Treating painful sex requires knowing the source. "Deep aching" usually signals muscle tension requiring relaxation, whereas "sharp stinging" suggests scar tissue or dryness requiring mobilization or hydration.
Additional information
MYTH: "I need to do more Kegels to recover."
REALITY: If your pain is caused by Hypertonicity (tight muscles), doing Kegels is like clenching a fist that is already cramping. It will increase your pain. You may actually need "Down-Training" (learning to relax the pelvic floor) instead of strengthening it.
Use these clinical indicators to help discuss your symptoms with a GP or Physiotherapist.
1. The Scar (Structural)
- Sensation: Sharp, stinging, or "tearing" feeling.
- Location: Specific to the vaginal entrance (introitus) or the perineum.
- Cause: Rigid collagen fibers from a tear or episiotomy that haven't regained elasticity.
- Solution: Perineal Massage (mobilization) to soften the tissue. Estrogen cream may be prescribed to improve tissue quality.
2. The Muscle (Hypertonicity)
- Sensation: Deep ache, throb, or a feeling of "hitting a wall." Pain often lingers after intercourse.
- Location: Deeper inside the pelvis or radiating to the hips/back.
- Cause: The "Guarding Reflex." Your body anticipates pain and subconsciously clenches the pelvic floor muscles.
- Solution: Diaphragmatic Breathing and Pelvic Physiotherapy (Internal Release). Avoid Kegels until the tone normalizes.
3. The Hormones (Dryness/GSM)
- Sensation: Friction, burning, or "sandpaper" feeling.
- Location: Generalized throughout the canal.
- Cause: Breastfeeding suppresses estrogen, mimicking temporary menopause (Genitourinary Syndrome of Menopause).
- Solution: Local Estrogen (pessaries/creams). Unlike HRT, these stay local to the tissue and are generally considered safe while breastfeeding.
Sometimes, a wound "over-heals," creating bright red, raw, elevated tissue known as Granulation Tissue (proud flesh). This is common after stitches loosen too early.
- Key Symptom: Specific sharp pain at the scar site + occasional spotting/bleeding after sex.
- Treatment: This rarely heals on its own. A GP or Gynaecologist can treat it easily with Silver Nitrate to cauterize the tissue.