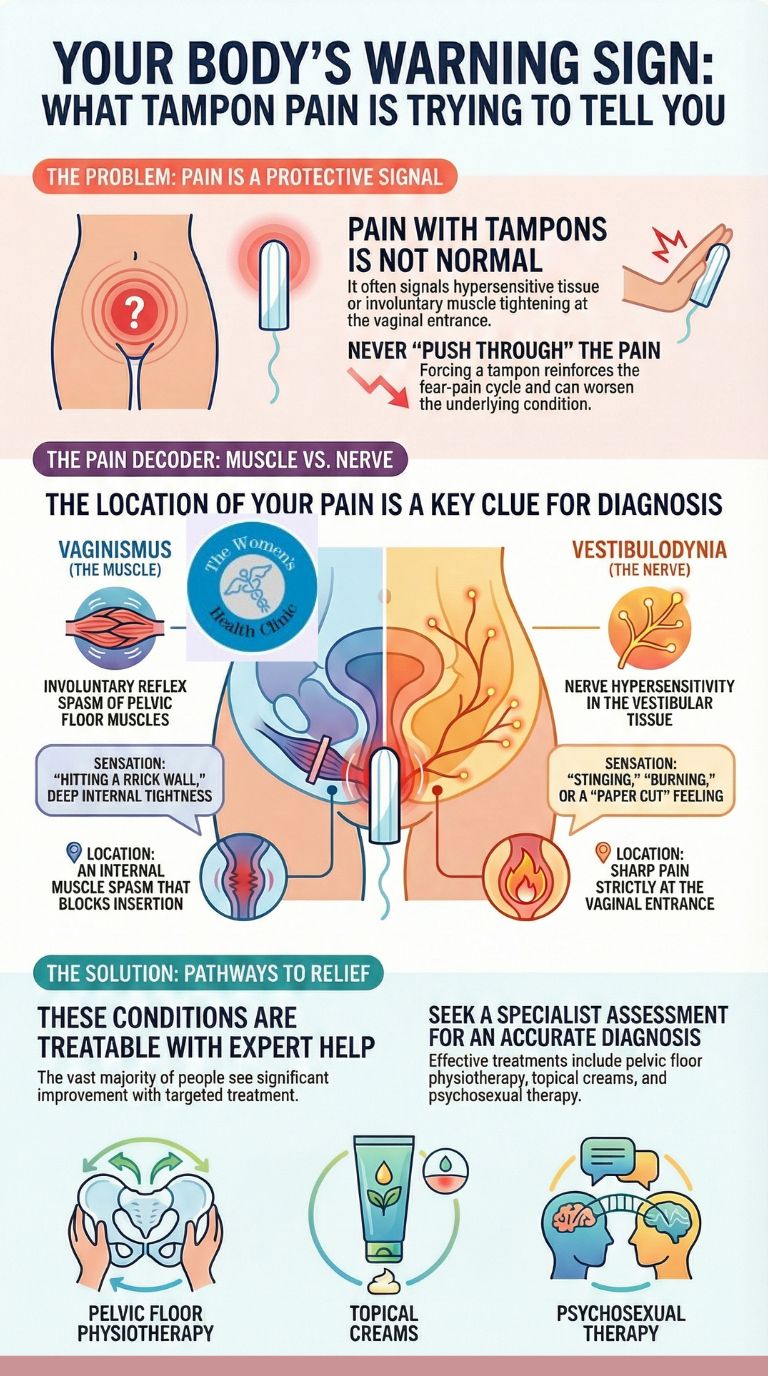
Tampon Pain—Does It Predict Vaginismus or Vestibulodynia?
Pain when inserting or removing tampons is not normal and can signal an underlying pelvic health condition. While it does not automatically mean you have vaginismus or vestibulodynia, it is a valuable early warning sign that the vaginal entrance or pelvic floor muscles may be hypersensitive, inflamed, or involuntarily tightening. The pattern of your pain—whether it is sharp and superficial or deep and cramping—helps clinicians identify the most likely cause and target treatment effectively.
Show Detailed Answer
Tampon insertion should feel neutral or mildly uncomfortable at most, particularly during your first attempts. If you experience sharp, burning, or tearing pain at the vaginal opening, or if the tampon feels “stuck” despite being anatomically positioned correctly, this suggests tissue sensitivity or muscle guarding that warrants investigation.
Many people assume the pain is due to inexperience or “doing it wrong,” but persistent tampon pain often reflects a measurable physical issue: nerve hypersensitivity in the vestibule (the entrance to the vagina), involuntary contraction of the pelvic floor muscles, or inflammation of the vaginal tissue. These mechanisms overlap significantly with the diagnostic criteria for vaginismus and vestibulodynia.
Understanding Vaginismus vs. Vestibulodynia
Though both conditions cause pain at the vaginal entrance, they have distinct characteristics:
- Vaginismus: An involuntary reflex spasm of the pelvic floor muscles (specifically the pubococcygeus and bulbospongiosus) that occurs in anticipation of vaginal penetration. It creates a “closing off” sensation, making tampon insertion feel impossible or like hitting a wall. The pain is often described as a tightness or “gripping” sensation. The muscle contraction is protective and often develops after a painful experience, such as a difficult smear test, infection, or even fear-based anticipation.
- Vestibulodynia (formerly Vulvar Vestibulitis): Chronic pain or burning localised to the vestibule—the small area surrounding the vaginal opening. Even light touch, such as inserting a tampon, can trigger sharp, stinging, or raw pain. Unlike vaginismus, the primary issue is not muscle spasm but nerve hypersensitivity and tissue inflammation. It is often described as feeling like “touching a cut” or “acid on skin.”
How Tampon Pain Links to These Conditions
Tampon insertion is a low-pressure, controlled form of vaginal penetration, which makes it a useful diagnostic clue. If you experience:
- Pain only at the very entrance, with burning or stinging: This pattern strongly suggests vestibulodynia. The vestibule contains a high density of nerve endings, and when these become sensitised (often due to hormonal changes, recurrent thrush, or skin conditions like lichen sclerosus), even minimal contact triggers intense pain.
- A sensation of “hitting a wall” or complete inability to insert the tampon: This is more indicative of vaginismus. The pelvic floor muscles contract reflexively, narrowing the vaginal canal. You may also notice this tightening during smear tests or sexual activity.
- Deep aching or cramping once the tampon is inside: This is less likely to be vaginismus or vestibulodynia and may point to conditions like endometriosis, adenomyosis, or pelvic floor tension affecting the deeper pelvic structures.
Other Causes of Tampon Pain
Not all tampon pain is due to vaginismus or vestibulodynia. Other causes include:
- Vaginal Dryness: Low oestrogen (common in breastfeeding, perimenopause, or hormonal contraception) reduces natural lubrication and thins the vaginal lining, making insertion painful.
- Infections: Recurrent thrush, bacterial vaginosis, or sexually transmitted infections can inflame the vaginal tissue and create surface tenderness.
- Skin Conditions: Lichen sclerosus, lichen planus, or contact dermatitis (e.g., reaction to scented sanitary products) can cause chronic vulval and vestibular pain.
- Anatomical Variations: A rigid or thickened hymen (imperforate or microperforate hymen) can make tampon insertion difficult, though this is uncommon and usually identified in adolescence.
Common Concerns & Myths
“Does tampon pain mean I’ll never be able to have sex?”
No. Tampon pain is a signal, not a life sentence. With targeted treatment—whether pelvic floor physiotherapy, topical oestrogen, or desensitisation therapy—the vast majority of people see significant improvement. Early intervention often prevents the condition from worsening.
“Is it because I’m a virgin or just nervous?”
Nervousness can cause temporary muscle tension, but ongoing, severe pain is not explained by virginity or anxiety alone. Both vaginismus and vestibulodynia have recognised physiological causes (muscle dysfunction and nerve sensitisation) that require clinical treatment, not just reassurance.
“Should I just push through the pain?”
Absolutely not. Forcing a tampon in when you are in pain reinforces the fear-pain cycle, worsens muscle guarding, and can cause micro-tears in the tissue. Pain is your body’s protective signal—listen to it and seek help.
Clinical Context
Tampon pain is frequently dismissed as a “technique issue,” but studies show that women with provoked vestibulodynia report significantly higher pain scores during tampon insertion compared to controls. Similarly, vaginismus is often first noticed during attempted tampon use in adolescence or early adulthood. Both conditions are underdiagnosed, with an average delay of several years between symptom onset and specialist referral. Early recognition through tampon-related pain can fast-track appropriate care, reducing the psychological impact and preventing chronic sensitisation. Educational only. Results vary. Not a cure.
Evidence-Based Approaches
Self-Care & Lifestyle
If you are experiencing tampon pain, consider these initial steps while seeking professional advice:
- Switch to Pads or Menstrual Cups: Temporarily avoid tampons to prevent reinforcing the pain response. Menstrual cups require a different insertion technique and may be easier for some, but if pain persists, do not force it.
- Use Lubrication: Apply a small amount of water-based, fragrance-free lubricant to the tip of the tampon to reduce friction at the entrance.
- Breathing & Relaxation: Practice diaphragmatic breathing (deep belly breaths) before insertion. This activates the parasympathetic nervous system and reduces pelvic floor tension.
- Positioning: Experiment with different angles (aiming towards the tailbone, not straight up) and try inserting with one leg raised on the toilet seat or lying down.
Medical & Specialist Options
Clinical treatment depends on whether the pain is muscular, neurological, or tissue-based. A specialist assessment can differentiate between vaginismus, vestibulodynia, and other causes.
- Pelvic Floor Physiotherapy: The gold standard for vaginismus. A specialist women’s health physiotherapist uses internal manual therapy, biofeedback, and dilator training to release muscle spasm and retrain the nervous system. This is highly effective and non-invasive.
- Topical Treatments for Vestibulodynia: Topical oestrogen (if tissue atrophy or dryness is present), lidocaine ointment (to reduce nerve hypersensitivity), or anti-inflammatory creams may be prescribed. Some patients benefit from topical gabapentin or amitriptyline compounded into a cream.
- Psychosexual Therapy: Cognitive behavioural therapy or mindfulness-based approaches address the fear-pain cycle and any anxiety or trauma linked to penetration.
- Diagnostic Investigations: A Q-tip test (cotton swab test) can map areas of tenderness in the vestibule. Vaginal swabs rule out infection. If deep pain is present, ultrasound or MRI may be needed to assess for endometriosis or structural abnormalities.
For a comprehensive pathway tailored to vaginal pain and sensitivity, you can view our step-by-step treatment plan. If you are ready to take the next step, you can book a consultation with our specialist team.
Red Flags (When to See a GP Urgently)
Seek medical review if you experience:
- Heavy, prolonged, or unexpected vaginal bleeding
- Foul-smelling discharge or fever (possible infection)
- Visible lumps, ulcers, or skin changes on the vulva
- Sudden onset of severe pain unrelated to your menstrual cycle
External Resources:
Educational only. Results vary. Not a cure.
Clinical Diagnostic: A tampon is more than a product; it is a diagnostic tool. "Hitting a wall" internally suggests muscular Vaginismus, while "stinging at the entrance" suggests neural Vestibulodynia. Structural issues like a Septate Hymen present as a physical snag during removal.
Additional Clinical Insights
Pain tells a story based on where it hurts. Use this guide to describe your symptoms to a clinician.
1. The Muscle: Vaginismus
- Sensation: "Hitting a brick wall" or inability to insert past the tip.
- Location: Internal tightness. The opening exists, but the pelvic floor muscles spasm shut involuntarily.
- Tampon Sign: The tampon slides out comfortably once inside, but insertion is the battle.
2. The Nerve: Provoked Vestibulodynia (PVD)
- Sensation: Burning, stinging, cutting, or "paper cut" feeling.
- Location: Strictly at the Entrance (Vestibule). Once past the entrance, deep insertion is often painless.
- Tampon Sign: Intense stinging upon insertion AND removal (when the dry cotton drags against the sensitive nerve endings).
Clinicians use the "Clock Face" method to map nerve pain. You can gently try this at home with a cotton bud.
[Image of female pelvic anatomy]- The Map: Imagine the opening is a clock. 12 o'clock is the urethra (top), 6 o'clock is the perineum (bottom).
- The Test: Lightly touch the 5 o'clock and 7 o'clock positions.
- The Result: If light touch here causes sharp pain (Allodynia), it is a classic sign of Localized Provoked Vestibulodynia. (Note: Tenderness at 12 o'clock is normal).
If you have never been able to use a tampon without pain, you may have Congenital Neuroproliferative Vestibulodynia.
- What it is: A condition where you are born with too many nerve endings (proliferation) in the vestibule tissue.
- The "Belly Button" Sign: Surprisingly, many women with this specific condition also have a sensitive belly button (Umbilical Hypersensitivity), as both tissues develop from the same embryonic source.
Sometimes the issue is physical, not muscular or neural.
- The Snag: A Septate Hymen has a band of tissue running down the middle, creating two small openings instead of one.
- Tampon Sign: You can insert a tampon, but it feels "stuck" or "hooked" on a strand of skin when you try to pull it out. This requires a minor surgical correction, not dilation.