Recurrent thrush or BV vs pain—how do I tell?
Recurrent thrush (candidiasis) and bacterial vaginosis (BV) typically cause itching, discharge, and odour, whereas vaginal pain—especially during sex or contact—is more often linked to tissue thinning, nerve sensitivity, or muscle tension. The key difference is that infections produce discharge and smell, while pain conditions often involve dryness, burning, or deep aching without abnormal discharge. However, the two can overlap, and persistent symptoms always warrant proper clinical assessment.
Show Detailed Answer
Many women experience cyclical vaginal symptoms and find it difficult to distinguish between infections and pain-related conditions. This confusion is understandable because both can cause discomfort, affect intimacy, and erode confidence. Understanding the distinctive clinical features of each helps you communicate more clearly with your clinician and receive the right treatment faster.
Thrush and BV are infections caused by an imbalance in the vaginal microbiome. Thrush is caused by an overgrowth of Candida yeast, while BV occurs when “good” lactobacilli are outnumbered by other bacteria. Pain conditions—such as vulvodynia, provoked vestibulodynia, or genitourinary syndrome of menopause (GSM)—are not infections. They involve changes in tissue health, nerve signalling, or muscle tone, often linked to hormonal shifts or chronic sensitisation.
Recognising Thrush (Vulvovaginal Candidiasis)
Thrush is one of the most common vaginal infections and tends to recur in some women, particularly if they are pregnant, taking antibiotics, have diabetes, or use hormonal contraception.
- Discharge: Thick, white, “cottage cheese-like” discharge with no strong smell.
- Itching: Intense vulval itching, often worse at night or after washing.
- Soreness: Redness, swelling, and a burning sensation, especially when urinating or during sex.
- Smell: Usually absent or very mild; thrush does not typically cause a fishy odour.
Recurrent thrush is defined as four or more episodes in a year. This pattern may signal an underlying issue, such as undiagnosed diabetes or immune suppression, and warrants further investigation.
Recognising Bacterial Vaginosis (BV)
BV is the most common cause of abnormal vaginal discharge in women of reproductive age. It is not sexually transmitted, but sexual activity can disrupt the vaginal pH and trigger an episode.
- Discharge: Thin, greyish-white, or watery discharge that coats the vaginal walls.
- Odour: A strong, “fishy” smell, particularly noticeable after sex or during menstruation.
- Itching: Usually mild or absent; BV rarely causes significant itching.
- Pain: Typically minimal, though some women report mild irritation.
Recurrent BV (defined as three or more episodes per year) can be frustrating and is linked to disrupted vaginal flora, sometimes exacerbated by over-washing, smoking, or the use of scented products.
Recognising Pain-Related Conditions
Pain conditions affecting the vulva and vagina are distinct from infections and often require a different diagnostic and therapeutic approach.
- Vulvodynia: Chronic vulval pain or burning lasting at least three months, without visible infection or skin disease. It may be constant or triggered by touch.
- Provoked Vestibulodynia: Sharp, burning pain at the vaginal entrance (vestibule) when touched, such as during tampon insertion or intercourse.
- GSM (Genitourinary Syndrome of Menopause): Thinning, drying, and inflammation of vaginal tissues due to low oestrogen, causing pain, dryness, and urinary symptoms.
- Pelvic Floor Dysfunction: Overactive or tense pelvic muscles causing deep aching, pressure, or pain during penetration.
These conditions often present with dryness, rawness, or a burning sensation rather than discharge. Pain may worsen with friction, touch, or deep penetration, and is not relieved by antifungal or antibiotic treatment.
When Symptoms Overlap
It is possible to have both an infection and a pain condition simultaneously. For example, recurrent thrush may sensitise nerve endings, leading to persistent vulval pain even after the infection clears. Similarly, GSM can make tissues more vulnerable to BV or thrush because the vaginal pH and immune environment are altered.
If you have been treated repeatedly for thrush or BV but symptoms persist, it may be worth exploring whether an underlying pain condition or hormonal change is contributing.
Common Concerns & Myths
“If I’ve no discharge, can it still be an infection?”
Possibly, but unlikely. Both thrush and BV almost always produce noticeable discharge. If you have pain without discharge, the cause is more likely to be hormonal, neurological, or muscular.
“Can thrush cause long-term pain?”
Yes. Repeated thrush infections can lead to chronic irritation and sensitisation of the nerve fibres in the vulva, a condition sometimes called “post-inflammatory vulvodynia.”
“Will probiotics cure recurrent BV?”
Evidence is mixed. Some women benefit from oral or vaginal probiotics containing lactobacilli, but they are not a guaranteed cure. Clinical treatment and lifestyle review (avoiding douching, perfumed products) are essential.
Clinical Context
Distinguishing between infection and pain is a core skill in vulvovaginal medicine. Many women are initially misdiagnosed or treated empirically for thrush when the real issue is atrophy or nerve pain. A thorough history, examination, and sometimes pH or swab testing are needed to confirm the diagnosis. Recurrent infections should also prompt screening for diabetes, immune conditions, or STIs. Educational only. Results vary. Not a cure.
Evidence-Based Approaches
Self-Care & Lifestyle
Simple changes can help you identify patterns and reduce symptom triggers.
- Symptom Diary: Track when symptoms occur, what they feel like, and any triggers (sex, periods, stress, products).
- Avoid Irritants: Stop using scented soaps, wipes, bubble baths, and douches. Wash with plain warm water only.
- Wear Breathable Clothing: Cotton underwear and loose trousers reduce moisture and heat, which can encourage thrush.
- Lubrication: If dryness is present, use a high-quality, pH-balanced lubricant during intimacy.
Medical & Specialist Options
Clinical management depends on accurate diagnosis and may involve swabs, pH testing, or specialist vulval examination.
- For Recurrent Thrush: Long-term antifungal treatment (oral or topical), screening for diabetes, and possibly maintenance therapy to prevent relapse.
- For Recurrent BV: Antibiotic courses (metronidazole or clindamycin), sometimes followed by vaginal acidifying gels or probiotics. Consider sexual health screening if applicable.
- For Pain Conditions: Topical oestrogen for GSM, pelvic floor physiotherapy for muscle tension, or specialist pain management for vulvodynia.
If you are unsure which pathway is right for you, you can read common questions about diagnosis and treatment. Many women also choose to book a consultation for personalised assessment and care planning.
C. Red Flags (When to see a GP)
Seek urgent medical review if you experience severe pelvic pain, fever, heavy or offensive discharge, unexplained bleeding, or if symptoms do not improve after treatment. Persistent pain or recurrent infections despite multiple treatments warrant specialist referral.
External Resources:
Educational only. Results vary. Not a cure.
Clinical Diagnostic: If standard treatment fails, you may be treating the wrong condition. "Recurrent Thrush" is often Cytolytic Vaginosis (an overgrowth of good bacteria), while "Recurrent BV" often hides behind a protective Biofilm. Using a simple pH test strip at home can help differentiate them.
Additional Clinical Diagnostics
If you have "thrush" symptoms (itching, white discharge) but anti-fungal creams burn or don't work, you may have Cytolytic Vaginosis.
Is it Thrush or CV?
- The Cause: CV is an overgrowth of Lactobacilli (the "good" bacteria). They produce too much acid, which burns the vaginal lining.
- The Clue: Symptoms typically worsen in the Luteal Phase (the week before your period) and improve during menstruation (because blood increases pH).
- The Treatment Flip: Thrush needs anti-fungals. CV needs Alkalising (e.g., Baking Soda sitz baths) to lower the acid levels. Using Canesten on CV will often make the pain worse.
Bacterial Vaginosis (BV) has a recurrence rate of over 50%. This is rarely due to hygiene; it is a survival mechanism of the bacteria.
- The Slime City: Gardnerella vaginalis creates a sticky protective mesh called a Biofilm. This shield adheres to the vaginal wall.
- Antibiotic Failure: Standard antibiotics kill the free-floating bacteria (resolving symptoms temporarily) but often fail to penetrate the biofilm nest. The bacteria then re-emerge weeks later.
You can buy vaginal pH test strips at most pharmacies. The number on the strip is a powerful diagnostic clue.
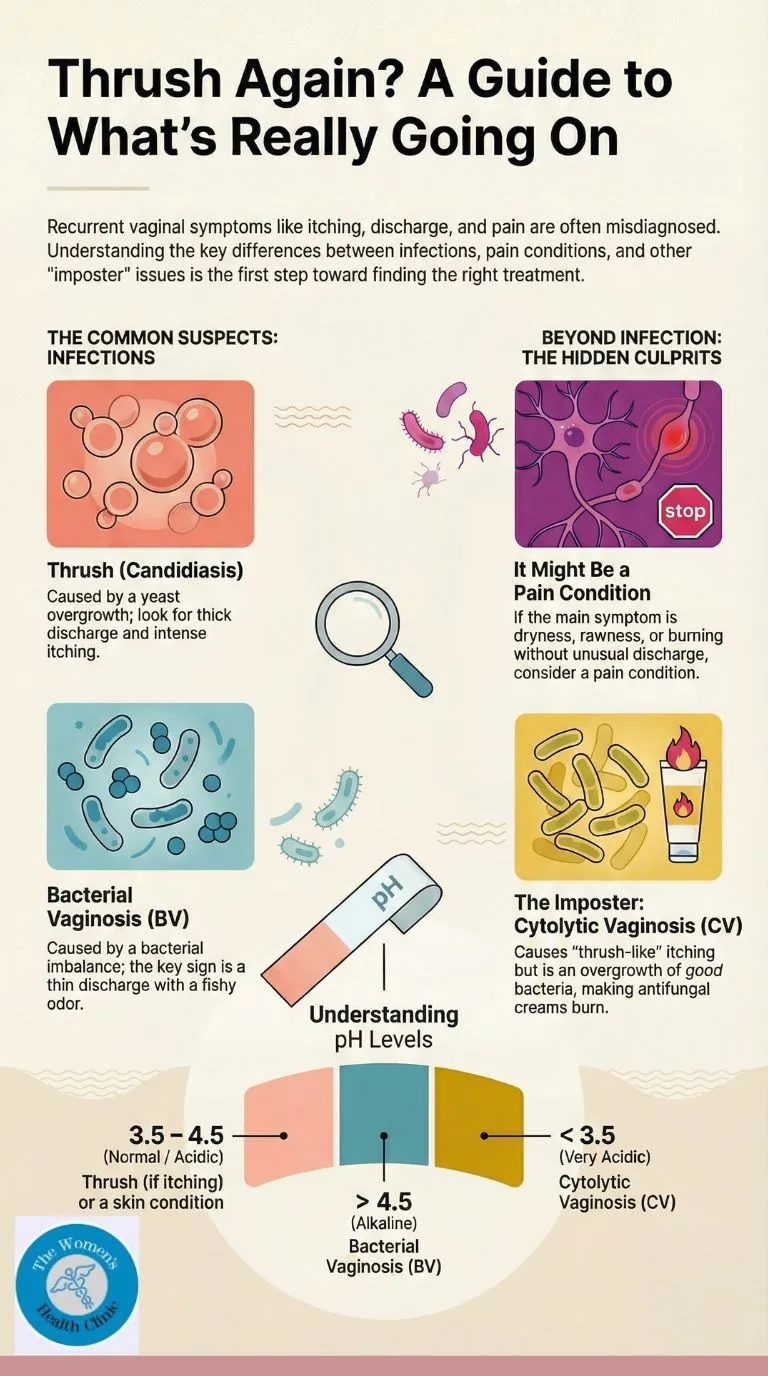
The pH Decoder
- pH 3.5 – 4.5 (Normal/Acidic): If you have itching with a normal pH, it is likely Thrush (Candida) or a skin condition like Eczema.
- pH < 3.5 (Very Acidic): This strongly suggests Cytolytic Vaginosis (Acid Overgrowth).
- pH > 4.5 (Alkaline): This indicates Bacterial Vaginosis (BV) or Trichomoniasis. BV bacteria cannot survive in an acidic environment, so a high pH is the key sign.
MYTH: "White patches mean it's definitely thrush."
REALITY: Persistent white patches that itch but don't rub off can be a sign of Lichen Sclerosus, a chronic skin condition. If you see a "figure-of-8" pattern of whiteness around the vulva and anus, or experience skin splitting (fissures), you need a dermatologist, not thrush cream.