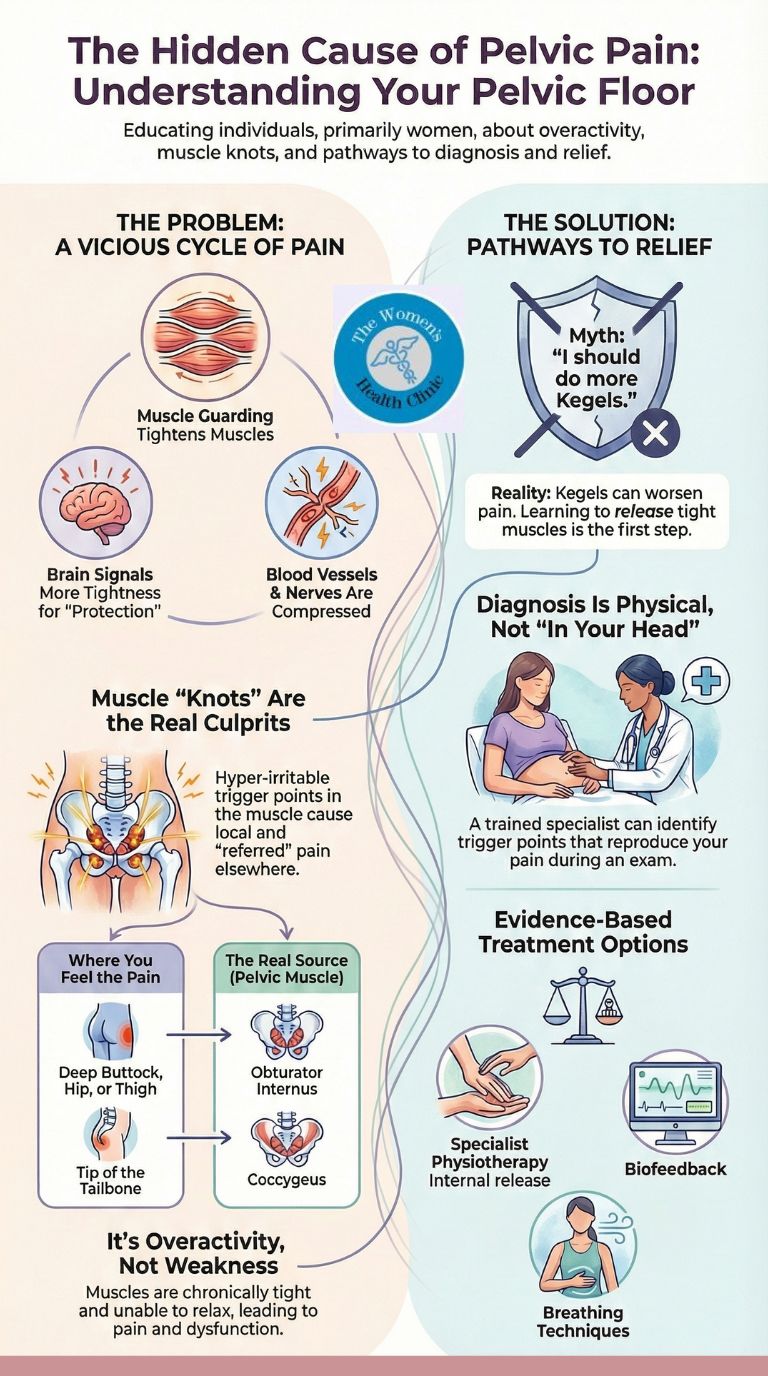
Pelvic Floor Overactivity and Trigger Points: How Do They Cause Pain?
Pelvic floor overactivity occurs when the muscles at the base of the pelvis remain chronically tight or spasm, unable to relax fully. Trigger points—hyperirritable knots within these muscles—generate pain locally and refer it to the bladder, vagina, rectum, or lower back, creating a cycle of guarding that amplifies discomfort. This tension can cause pain during sex, bladder urgency, and even difficulty emptying the bowel.
Show Detailed Answer
The pelvic floor is a hammock of muscles, ligaments, and connective tissue that supports the bladder, uterus, and bowel whilst controlling continence and sexual function. When functioning properly, these muscles contract and relax in a coordinated rhythm. However, when they become overactive—constantly engaged, tight, or stuck in a shortened position—they lose their ability to respond flexibly to everyday activities like sitting, walking, or intimacy.
This overactivity is not a sign of weakness. In fact, it is often the opposite: the muscles are working too hard, driven by protective reflexes following injury, infection, trauma, or chronic stress. Over time, discrete areas within the muscle develop trigger points—localised, tender nodules that reproduce your pain when pressed. These trigger points do not just hurt where they sit; they send pain signals to other pelvic structures, a phenomenon called “referred pain.”
The Anatomy: Why the Pelvic Floor Matters
The pelvic floor includes several key muscle groups:
- Levator Ani: The largest group, forming the main supportive sling. Includes the pubococcygeus, puborectalis, and iliococcygeus muscles.
- Coccygeus: Sits at the back, supporting the tailbone.
- Obturator Internus and Piriformis: Deep hip rotators that attach near the pelvic floor and can harbour trigger points that refer pain into the pelvis.
All of these muscles are richly innervated by the pudendal nerve and sacral plexus. When muscles remain chronically contracted, they compress these nerves, generating pain, burning, or electric-shock sensations that radiate along nerve pathways.
What Are Trigger Points and How Do They Form?
Trigger points are taut bands within a muscle that do not fully release. They form when:
- Protective guarding occurs: After a painful experience (e.g., vaginal birth, infection, surgery), the nervous system tells the pelvic floor to “brace” to prevent further injury. If this guarding never switches off, muscles become stuck in contraction.
- Repetitive strain builds up: Prolonged sitting, heavy lifting, or high-impact exercise without adequate rest can fatigue muscles and create micro-tears that heal as tight, fibrous nodules.
- Emotional stress is stored: Chronic anxiety, trauma, or fear can keep the entire nervous system on high alert, preventing muscles from ever fully relaxing.
These trigger points restrict blood flow to the muscle, creating a hypoxic (low oxygen) environment that perpetuates pain and prevents healing.
How Trigger Points Generate Pain: The Vicious Cycle
Once established, trigger points create a self-sustaining loop:
- Muscle contraction compresses blood vessels: This reduces oxygen delivery and waste removal, leading to a build-up of metabolic irritants (e.g., lactic acid, bradykinin) that sensitise pain receptors.
- Pain receptors signal the brain: The brain interprets this as danger and sends signals to tighten the muscles further for “protection.”
- Referred pain confuses the picture: A trigger point in the levator ani might be felt as bladder urgency, rectal pressure, or clitoral burning—making it hard to identify the true source.
- Fear and avoidance worsen the cycle: Anticipation of pain leads to guarding before the activity even starts, reinforcing overactivity.
Common Symptoms of Pelvic Floor Overactivity
The presentation varies, but typical symptoms include:
- Pain with vaginal penetration (superficial or deep dyspareunia)
- Difficulty inserting tampons or having a smear test
- Bladder urgency, frequency, or hesitancy (despite negative urine tests)
- Constipation or pain with bowel movements
- Tailbone, lower back, or hip pain
- A feeling of pelvic heaviness or “sitting on a golf ball”
- Post-coital aching that lasts hours or days
Common Concerns & Myths
“I thought pelvic floor problems meant I was too weak—why am I being told I’m too tight?”
This confusion is common. While stress incontinence often results from pelvic floor weakness, pain syndromes are usually caused by overactivity. A tight pelvic floor can also be a weak one—muscles that never relax cannot generate force effectively.
“Will doing more Kegels fix this?”
No. In fact, traditional Kegel exercises (squeeze and hold) can worsen overactivity. Treatment focuses on lengthening, releasing, and retraining the muscles to relax before they contract.
“Is this pain all in my head?”
Absolutely not. Pelvic floor trigger points are physical, palpable findings that a trained physiotherapist can identify during internal examination. The pain is real, and it has a structural cause.
Clinical Context
Pelvic floor overactivity and myofascial trigger points are increasingly recognised as key contributors to chronic pelvic pain syndromes, including vaginismus, vulvodynia, chronic prostatitis (in men), and interstitial cystitis. It is estimated that up to 85% of women with chronic pelvic pain have pelvic floor muscle dysfunction, yet many go years without an accurate diagnosis. Assessment requires internal vaginal or rectal examination by a pelvic health physiotherapist trained in myofascial techniques. Educational only. Results vary. Not a cure.
Evidence-Based Approaches
Self-Care & Lifestyle
While professional treatment is essential, self-care strategies can support muscle relaxation and nervous system calming.
- Diaphragmatic Breathing: Slow, deep belly breathing activates the vagus nerve and encourages the pelvic floor to release in sync with the breath.
- Heat Therapy: A warm bath, heat pack, or microwavable wheat bag applied to the lower abdomen or perineum can ease muscle tension.
- Mindful Movement: Gentle yoga (especially hip openers), Pilates, or walking can improve circulation and reduce chronic bracing patterns.
- Posture Awareness: Avoid prolonged sitting or “tucking” the pelvis under. Use a cushion to support neutral alignment.
- Stress Management: Chronic stress keeps the nervous system in fight-or-flight mode. Meditation, counselling, or somatic therapies can help.
Medical & Specialist Options
Treatment is led by specialist pelvic health physiotherapists, often in collaboration with gynaecologists, pain specialists, or psychosexual therapists.
- Internal Myofascial Release: The physiotherapist uses gloved fingers to apply sustained pressure to trigger points, encouraging release and restoring length to shortened muscles.
- Biofeedback: A sensor is placed in the vagina or rectum to display muscle activity on a screen, helping you learn to consciously relax the pelvic floor.
- Electrical Stimulation: Low-frequency currents can fatigue overactive muscles, encouraging them to relax.
- Dilator Therapy: Graduated vaginal dilators help desensitise the area and retrain the muscles to tolerate gentle stretch without guarding.
- Botulinum Toxin (Botox) Injections: In severe cases, injections into the pelvic floor can temporarily paralyse overactive muscles, breaking the pain cycle and allowing physiotherapy to progress.
- Cognitive Behavioural Therapy (CBT) or Psychosexual Counselling: Addresses the fear-pain-avoidance cycle and helps restore intimacy and confidence.
For a comprehensive pathway combining these modalities, you can view our step-by-step treatment plan or book a consultation with our specialist team.
Red Flags (When to See a GP Urgently)
Seek immediate medical review if you experience sudden-onset severe pelvic pain, fever, heavy bleeding, loss of bladder or bowel control, numbness in the saddle area (perineum, inner thighs), or leg weakness. These may indicate cauda equina syndrome or another serious condition requiring emergency care.
External Resources:
Educational only. Results vary. Not a cure.
Clinical Insight: Trigger points are "muscle knots" that cheat—they send pain to distant areas ("Referred Pain"). For example, a knot deep inside the pelvis (Obturator Internus) often mimics hip pain or sciatica. Crucially, these tight muscles can physically strangle the nerves running through them.
Additional Clinical Context
Pain in your hip or tailbone may actually be originating from inside the pelvic floor. This is called Referred Pain.
1. The Hip Mimic (Obturator Internus)
- The Muscle: A fan-shaped muscle that rotates the hip but lines the pelvic wall.
- The Pain: When this muscle has trigger points, it refers pain to the deep buttock, hip joint, or back of the thigh. Patients often think they have a hip problem, but the issue is pelvic.
- The Sign: Pain worsens when rotating the leg inward.
2. The Tailbone Mimic (Coccygeus)
- The Muscle: The muscle connecting the sit bones to the tailbone.
- The Pain: It refers pain directly to the tip of the coccyx (tailbone).
- The Reality: Many cases of "Coccydynia" (tailbone pain) are actually just a tight Coccygeus muscle pulling on the bone, not a bone injury itself.
Why does muscle tension cause nerve pain? It's anatomical.
- The Trap: The Pudendal Nerve runs through a tunnel called Alcock's Canal.
- The Connection: This tunnel is formed by the fascia (connective tissue) of the Obturator Internus muscle.
- The Result: If the Obturator muscle is spastic or bulky from tension, it crushes the tunnel. This strangles the nerve, causing burning, numbness, or electric shock pain (Pudendal Neuralgia).
How do we know if it's a Trigger Point or just soreness?
- The Test: During an internal exam, the physio applies pressure to the taut band of muscle.
- Positive Result: A "Jump Sign"—the patient involuntarily flinches or the muscle physically twitches under the finger. This confirms a Trigger Point (a localized contraction knot) rather than general inflammation.
MYTH: "My pelvic floor is weak, so I need to do Kegels."
REALITY: A tight muscle is often a weak muscle because it is exhausted from being "on" 24/7. Doing Kegels (contractions) on a hypertonic floor is like doing bicep curls with a cramped arm—it causes more damage. You must learn to Release (Down-Train) before you strengthen.