Pain on thrusting or deep inside—what might be the cause?
Pain deep inside the vagina or pelvis during thrusting is known as deep dyspareunia. It is most commonly caused by structural issues such as endometriosis, ovarian cysts, fibroids, or pelvic floor muscle tension, though pelvic inflammatory disease and adhesions from previous surgery can also be responsible. This type of pain typically worsens with deeper penetration and certain positions, and it often signals that something in the pelvic region requires medical assessment.
Show Detailed Answer
Deep pelvic pain during intercourse is a distressing symptom that can significantly affect intimate relationships and emotional wellbeing. Unlike pain felt at the vaginal entrance (superficial dyspareunia), deep pain occurs further inside—often felt in the lower abdomen, around the cervix, or radiating into the back or thighs. Many describe it as a dull ache, sharp stabbing, or a sensation of being “bumped” internally.
This pain is not psychosomatic or “in your head.” It is a physical signal that structures deep in the pelvis—such as the uterus, ovaries, pelvic ligaments, or surrounding muscles—are being compressed, stretched, or inflamed during movement. Understanding the specific cause is essential, as treatment varies widely depending on whether the issue is hormonal, structural, muscular, or inflammatory.
Common Causes of Deep Pelvic Pain During Sex
1. Endometriosis
Endometriosis occurs when tissue similar to the lining of the womb grows outside the uterus—on the ovaries, bowel, or pelvic walls. During penetration, the movement can pull on these inflamed areas, causing sharp or cramping pain. Symptoms often worsen just before or during menstruation. Deep pain with thrusting, especially in certain positions (e.g., deep missionary or doggy style), is a hallmark sign.
2. Ovarian Cysts or Fibroids
Functional ovarian cysts (fluid-filled sacs) or uterine fibroids (benign muscle growths) can create a “collision” effect during deep penetration. If the penis or a toy strikes the enlarged ovary or fibroid, it causes sudden, intense pain. Large fibroids can also change the position of the uterus, making certain angles more painful.
3. Pelvic Inflammatory Disease (PID)
PID is an infection of the reproductive organs, usually caused by untreated sexually transmitted infections like chlamydia or gonorrhoea. It inflames the uterus, fallopian tubes, and ovaries, making them tender. Deep penetration can aggravate this inflammation, causing pain alongside abnormal discharge, fever, or irregular bleeding.
4. Pelvic Floor Muscle Dysfunction
The pelvic floor muscles support the bladder, bowel, and uterus. When chronically tight or in spasm (often due to previous pain, trauma, or stress), they can create referred pain deep in the pelvis during thrusting. This is sometimes mistaken for organ pathology but is actually a muscular issue that responds well to physiotherapy.
5. Adhesions from Surgery or Infection
Scar tissue (adhesions) can form after pelvic surgery (e.g., caesarean section, appendectomy, or ovarian cyst removal) or previous infection. These bands of tissue can tether organs together, restricting movement and causing pain when the pelvis shifts during intercourse.
6. Retroverted Uterus
In about 20% of women, the uterus tilts backwards (retroverted) rather than forwards. While this is a normal anatomical variant, it can make the cervix and uterus more vulnerable to being bumped during deep penetration, especially in rear-entry positions.
7. Genitourinary Syndrome of Menopause (GSM)
After menopause, declining oestrogen causes the vaginal canal to shorten and lose elasticity. Deep thrusting can then reach the top of the vagina or cervix more easily, causing discomfort. This is often accompanied by dryness and thinning of the vaginal walls.
Common Concerns & Myths
“Is it because I’m not aroused enough?”
Not necessarily. While arousal does lengthen and widen the vagina (tenting), deep pain is more often due to structural or inflammatory causes inside the pelvis that arousal cannot resolve.
“Will changing positions fix it?”
Changing positions may reduce pain by avoiding certain angles (e.g., shallow penetration positions give you more control), but it does not treat the underlying cause. If the pain persists across all positions, medical review is needed.
“Is this just part of ageing?”
No. While some changes are hormone-related and treatable, persistent deep pain is never “just normal ageing” and should always be investigated.
Clinical Context
Deep dyspareunia is a common presenting symptom in gynaecology clinics and requires careful assessment to distinguish between gynaecological pathology (endometriosis, PID, fibroids) and musculoskeletal dysfunction (pelvic floor tension). Diagnosis typically involves a detailed pain history, pelvic examination, and often imaging such as transvaginal ultrasound. In some cases, laparoscopy may be required to confirm endometriosis. Treatment is highly individualised and may involve hormonal therapy, physiotherapy, or surgical intervention. Educational only. Results vary. Not a cure.
Evidence-Based Approaches
Self-Care & Lifestyle
While self-care alone cannot treat structural causes, it can help manage symptoms and improve comfort during intimacy.
- Control depth: Use positions where you control penetration depth (e.g., woman-on-top, spooning) to avoid painful collision.
- Use cushions: Placing a pillow under your hips can tilt the pelvis and reduce deep contact with sensitive areas.
- Communicate openly: Signal your partner immediately if something hurts, and explore non-penetrative intimacy while awaiting diagnosis.
- Pain diary: Track when pain occurs (time in cycle, specific positions, severity) to help your clinician identify patterns.
Medical & Specialist Options
Treatment depends entirely on the underlying diagnosis and may include medical, physiotherapy, or surgical approaches.
- Hormonal treatments: For endometriosis, combined contraceptive pills, progestogens, or GnRH analogues can suppress lesion growth and reduce inflammation.
- Pelvic floor physiotherapy: Specialist physios use internal manual therapy, dilators, and biofeedback to release muscle tension and desensitise painful areas.
- Antibiotics: PID requires prompt antibiotic treatment to prevent long-term complications such as infertility or chronic pain.
- Surgery: Laparoscopy to excise endometriosis, remove large cysts, or release adhesions may be recommended if conservative measures fail.
- Topical oestrogen: For postmenopausal women with GSM, vaginal oestrogen restores tissue health and elasticity.
If you are exploring specialist care pathways, you can meet the clinical team and book a consultation to discuss your symptoms in detail.
C. Red Flags (When to see a GP urgently)
Seek same-day medical attention if deep pain is accompanied by fever, heavy vaginal bleeding, sudden severe abdominal pain, vomiting, or fainting. These may indicate acute PID, ovarian torsion, or ectopic pregnancy—all medical emergencies.
External Resources:
Educational only. Results vary. Not a cure.
Clinical Diagnostic: "Deep Pain" is specific. A sharp sharp pain on impact suggests "Collision Dyspareunia" (often due to a Tilted Uterus or Adhesions), while a dull, heavy ache that lasts for hours afterwards suggests Pelvic Congestion (Varicose Veins).
Additional Clinical Insights
MYTH: "If I relax enough, deep sex won't hurt."
REALITY: Relaxation helps muscles, but it cannot fix Adhesions. If your ovaries or uterus are "glued" in place by scar tissue (from Endometriosis or past surgery), they cannot slide out of the way of the penis. No amount of breathing will prevent that mechanical impact pain.
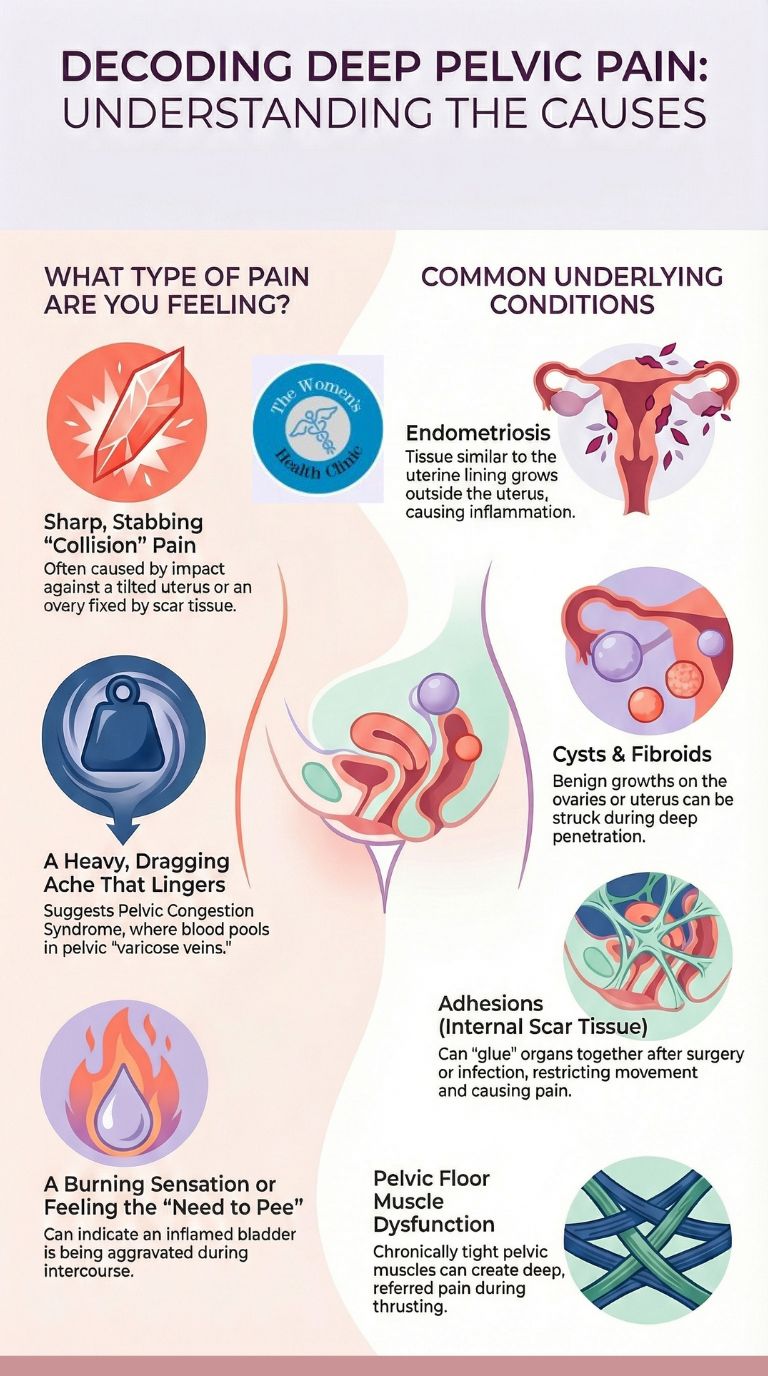
The type of pain you feel offers a clue to the anatomical cause.
1. Sharp, Stabbing Impact (Collision)
- Cause: Retroverted Uterus ("Tilted Womb"). About 25% of women have a uterus that tilts backward towards the tailbone (Sacrum).
- Mechanism: During deep thrusting, the penis hits the cervix, which pushes the uterus directly against the sensitive nerves of the sacrum. This is mechanical "Collision Dyspareunia".
- Fix: Positions that limit depth (like "Spoons") or using depth-limiting rings (Ohnut).
2. Heavy, Dragging Ache (Vascular)
- Cause: Pelvic Congestion Syndrome (PCS). Essentially "varicose veins" in the pelvis.
- Mechanism: Sexual arousal increases blood flow to the pelvis. If your veins have weak valves, this blood gets trapped (pools), causing a swollen, throbbing ache that often lasts for hours after sex. It is typically worse after standing all day.
3. Burning or "Need to Pee" (Bladder)
- Cause: Interstitial Cystitis (Painful Bladder Syndrome).
- Mechanism: The bladder sits directly on top of the anterior vaginal wall. Deep thrusting physically batters the inflamed bladder, causing pain that feels "vaginal" but is actually urinary. You may feel a flare of urgency the next day.
In a healthy pelvis, your ovaries are mobile—they float and slide out of the way during intercourse.
- The Problem: Conditions like Endometriosis or previous C-sections create sticky scar tissue (Adhesions).
- The Result: The ovary becomes "Fixed" (stuck) to the pelvic wall or uterus. When hit during sex, it cannot move, resulting in a sickening, visceral pain. This is a key sign to look for on an ultrasound (the "Sliding Sign").