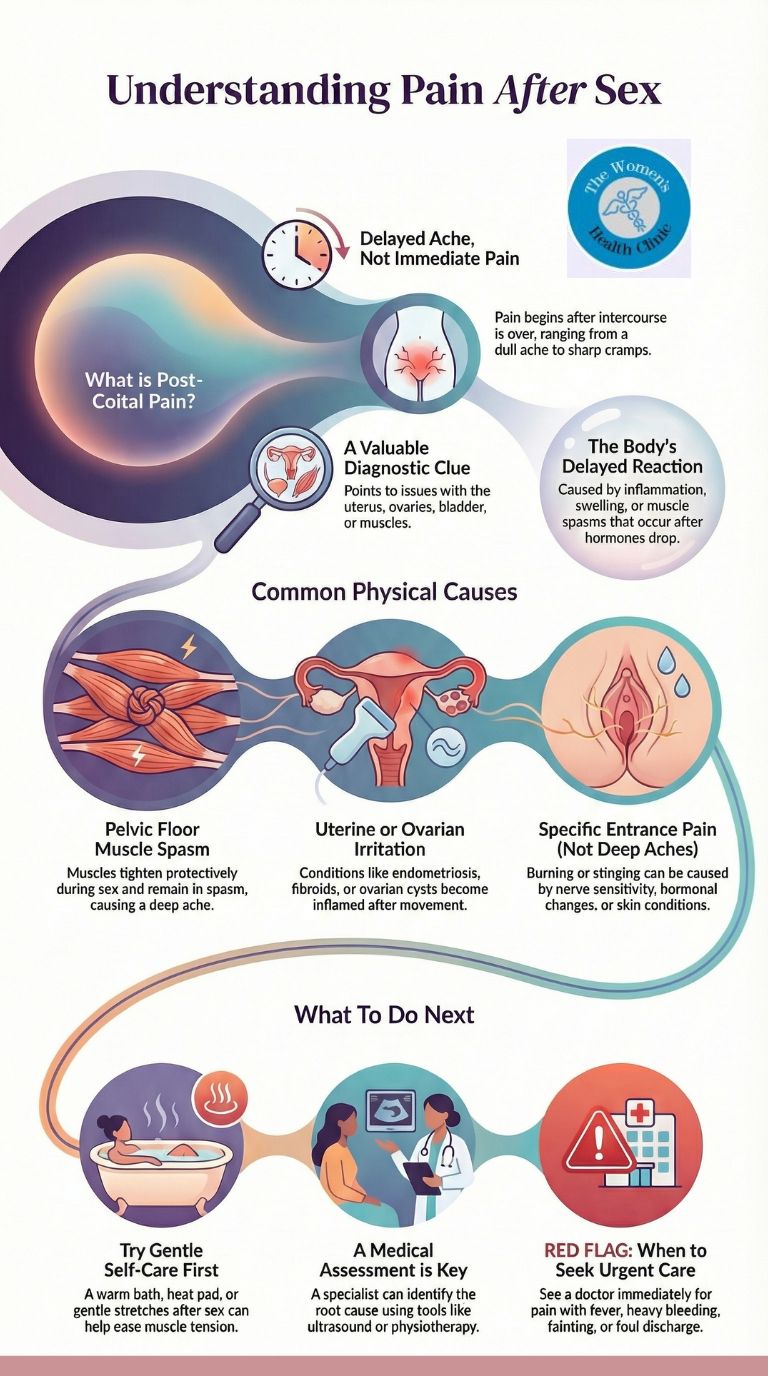
Pain after sex rather than during—what could that indicate?
Pain that appears after sex—rather than during penetration or thrusting—is often linked to pelvic floor muscle tension, uterine or ovarian irritation, or inflammation triggered by the physical activity of intercourse. Post-coital pain lasting minutes to hours typically suggests deep pelvic structures such as ovaries, uterus, or bladder are responding to mechanical pressure or muscular spasm. It is a recognised symptom with identifiable physical causes that warrant proper assessment.
Show Detailed Answer
Post-coital pain is distinct from pain felt during penetration or deep thrusting. It emerges once intercourse has finished and can range from a dull ache to sharp cramping. Some people describe it as feeling like period cramps, a heavy dragging sensation, or bladder pressure. The pain may last minutes, hours, or occasionally into the next day.
This delayed pain pattern is clinically significant because it points toward structures that become inflamed or irritated after mechanical stimulation—such as the pelvic floor muscles going into spasm, the uterus contracting post-orgasm, or ovarian cysts being jostled. Understanding the timing and character of the pain helps clinicians narrow down the likely anatomical source.
Common Physical Causes of Post-Coital Pain
Several gynaecological and musculoskeletal conditions can trigger pain after sex:
- Pelvic Floor Muscle Spasm: The pelvic floor muscles may tighten protectively during intercourse and remain in spasm afterwards, causing a deep ache or cramping that persists for hours. This is particularly common in people with underlying tension or a history of pain.
- Ovarian Cysts: Functional cysts on the ovaries can be knocked or compressed during deep penetration. The pain may not be felt immediately but develops as the ovary swells or fluid shifts afterwards.
- Endometriosis: Endometrial tissue outside the uterus can become inflamed after mechanical disturbance, causing delayed pelvic pain, often accompanied by bowel or bladder symptoms.
- Uterine Conditions: Fibroids, adenomyosis, or a retroverted (tilted) uterus can all cause the uterus to cramp or ache after being moved during intercourse.
- Bladder Irritation: The bladder sits just in front of the vagina. Pressure during sex can trigger inflammation, leading to post-coital urgency, burning, or a heavy ache.
- Infection or Inflammation: Pelvic inflammatory disease (PID), cervicitis, or chronic low-grade infection can flare after intercourse, causing delayed pain and sometimes abnormal discharge.
Why the Delay? Understanding the Mechanism
The reason pain appears after—not during—is often due to the body’s inflammatory or muscular response. During intercourse, adrenaline and endorphins may mask discomfort. Once these hormones drop, the pelvic floor muscles may spasm, inflamed tissues swell, or the uterus contracts (especially post-orgasm due to oxytocin release). This delayed inflammatory or muscular reaction is what you feel as post-coital pain.
Emotional and Relational Impact
Post-coital pain can be deeply confusing and frustrating. Many people feel guilty, worried they are “broken,” or anxious that their partner will take it personally. It can lead to avoidance of intimacy, reduced desire, and a sense of disconnection. Recognising that this is a physical symptom with identifiable causes—not a psychological failing—is the first step toward reclaiming comfort and confidence.
Common Concerns & Myths
“Does post-sex pain mean I have an STI?”
Not necessarily. While pelvic inflammatory disease (often caused by untreated STIs) can cause post-coital pain, many other non-infectious causes—such as endometriosis or pelvic floor tension—are more common. A full sexual health screen is still sensible as part of your assessment.
“Is it just because we were too rough?”
Vigorous activity can trigger symptoms, but if pain consistently appears after sex regardless of intensity or position, there is likely an underlying anatomical or muscular issue that needs clinical attention.
“Will it go away on its own?”
Occasionally, if linked to a transient cyst or minor muscle strain. However, persistent or worsening post-coital pain warrants investigation to rule out conditions like endometriosis or chronic infection.
Clinical Context
Post-coital pain is a presenting symptom in a significant proportion of women with endometriosis, pelvic floor dysfunction, and ovarian pathology. It is often under-reported because patients feel embarrassed or believe it is “normal.” In reality, it is a valuable diagnostic clue. A thorough history—including the timing, location, and associated symptoms—guides appropriate investigation, which may include pelvic ultrasound, swabs for infection, or referral to a specialist pelvic health physiotherapist. Educational only. Results vary. Not a cure.
Evidence-Based Approaches
Self-Care & Lifestyle
Initial self-management can help reduce the frequency and severity of post-coital pain while you await medical review.
- Pelvic Floor Relaxation: Gentle stretches, deep breathing, and avoiding immediate post-sex activity (such as rushing to the toilet) can help muscles release rather than spasm.
- Heat Therapy: A warm bath or heat pad applied to the lower abdomen after sex can ease cramping and muscular tension.
- Hydration: If bladder irritation is part of the picture, drinking water after intercourse may help flush the bladder and reduce discomfort.
- Positioning Experimentation: Certain positions place less pressure on the posterior fornix (area behind the cervix) or ovaries, potentially reducing the mechanical trigger for delayed pain.
Medical & Specialist Options
Treatment is guided by the underlying cause, which is identified through examination, imaging, and sometimes diagnostic laparoscopy.
- Pelvic Ultrasound: Identifies ovarian cysts, fibroids, or uterine abnormalities.
- Infection Screening: Swabs and blood tests to rule out PID or chronic cervicitis.
- Pelvic Floor Physiotherapy: Specialist internal physiotherapy releases hypertonic muscles, retrains the pelvic floor, and desensitises painful areas.
- Hormonal Management: For endometriosis or adenomyosis, combined hormonal contraceptives or progestogens may reduce inflammation and pain.
- Laparoscopy: Diagnostic keyhole surgery may be recommended if endometriosis or adhesions are suspected.
To explore a holistic approach to pelvic wellness, you can explore treatment benefits. If you are ready to take the next step, you can book a consultation with our specialist team.
C. Red Flags (When to see a GP urgently)
Seek immediate medical attention if post-coital pain is accompanied by fever, heavy vaginal bleeding, severe abdominal pain, fainting, or abnormal discharge with a foul odour. These may indicate acute infection, ectopic pregnancy, or ovarian torsion.
External Resources:
Educational only. Results vary. Not a cure.
Clinical Diagnostic: Pain at the entrance isn't always "tightness." It can be Neural (Vestibulodynia), Hormonal (Pill-induced), or Dermatological (Lichen Sclerosus). If "relaxing" doesn't help, the cause may be nerve hypersensitivity, not muscle tension.
Additional Diagnostic Insights
If the pain feels like "burning," "stinging," or "raw paper cuts" specifically at the entrance, it is likely nerve-related, not just muscular.
The Q-Tip Test
- Mechanism: In PVD, the nerves at the entrance (Vestibule) are hypersensitive (Allodynia). Light touch feels like fire.
- Location: Pain is typically sharpest at 5 o'clock and 7 o'clock (the back corners of the opening).
- Difference from Vaginismus: Vaginismus is a "blocking" sensation (muscle); PVD is a "burning" sensation (nerve).
For some women, the Combined Oral Contraceptive Pill causes **Hormonally Mediated Vestibulodynia**.
- How it happens: The Pill increases SHBG (Sex Hormone Binding Globulin), which lowers free testosterone. The vestibular glands need testosterone to stay healthy. Without it, they thin out and become painful.
- The Fix: Stopping the pill and using topical Estrogen/Testosterone cream (prescribed) can often reverse this atrophy.
If you have white patches or tiny splits (fissures) that bleed after sex, you may have a skin condition called Lichen Sclerosus.
- Symptoms: Itching, white "parchment-like" skin, and tearing at the entrance.
- Action: This is an autoimmune condition, not an infection. It requires steroid ointment to prevent scarring.