Can topical lidocaine help vestibular pain before sex?
Yes, topical lidocaine can help manage vestibular pain before sex by temporarily numbing hypersensitive nerve endings at the vaginal opening. Applied 15–30 minutes before intimacy, it reduces burning or stinging sensations in women with provoked vestibulodynia, though it works best as part of a broader treatment plan that addresses underlying causes. It is not a cure, but it can break the pain-avoidance cycle while longer-term therapies take effect.
Show Detailed Answer
Topical lidocaine is a local anaesthetic that blocks pain signals from nerve fibres in the skin and mucous membranes. When applied to the vulvar vestibule—the sensitive area just inside the vaginal opening—it can dull the sharp, burning pain many women experience at the moment of touch or penetration. This type of pain is often linked to provoked vestibulodynia (PVD), a condition where the vestibular tissue becomes hypersensitive due to nerve upregulation, inflammation, or hormonal changes.
The pain of vestibulodynia is not “all in your head.” It is a real, measurable hypersensitivity of the pudendal nerve branches and surrounding tissue. For many women, even the lightest touch—such as inserting a tampon or during a smear test—can trigger intense discomfort. This creates a fear-pain cycle: anticipating pain causes pelvic floor muscles to tighten protectively, which in turn worsens the pain. Lidocaine helps interrupt this cycle by allowing touch without the immediate sensory alarm.
How Lidocaine Works for Vestibular Pain
Lidocaine functions by blocking voltage-gated sodium channels in nerve cell membranes, preventing pain signals from being transmitted to the brain. When applied topically, it absorbs through the mucosal surface and acts locally—meaning it does not cause systemic numbness or enter the bloodstream in significant amounts.
- Formulation: Most commonly used as 2% or 5% lidocaine gel or ointment. Some clinicians prefer aqueous gels as they are less likely to irritate sensitive tissue.
- Application: Apply a small amount directly to the vestibule (the “horseshoe” area around the vaginal opening) 15–30 minutes before sexual activity. Gently wipe away excess before penetration to avoid transferring numbness to your partner.
- Duration: The numbing effect typically lasts 30–60 minutes, giving a window for comfortable intimacy.
Clinical Evidence & Effectiveness
Research into topical lidocaine for vestibulodynia shows mixed but generally supportive results. A randomised controlled trial published in the journal Obstetrics & Gynecology found that nightly application of 5% lidocaine ointment to the vestibule for 7 weeks resulted in significant pain reduction in women with PVD, with some continuing to experience relief even after stopping the treatment.
However, lidocaine is considered a symptom management tool rather than a cure. It is most effective when combined with:
- Pelvic floor physiotherapy to release muscle guarding
- Topical oestrogen if tissue atrophy or dryness is present
- Cognitive behavioural therapy (CBT) or psychosexual counselling to address the anxiety and avoidance behaviour
Practical Tips for Use
- Test First: Apply a tiny amount to the inner forearm to check for allergic reaction or irritation before using on the vulva.
- Less is More: Use only a pea-sized amount. Over-application can cause excessive numbness or mess.
- Avoid Oil-Based Formulations with Condoms: Some lidocaine ointments contain petroleum jelly, which can weaken latex condoms. Choose water-based gels if using barrier contraception.
- Communicate with Your Partner: Let them know you are using a numbing agent so they understand if there is reduced sensation and can adjust touch accordingly.
Limitations & Side Effects
While generally safe, lidocaine is not suitable for everyone:
- Temporary Numbness: You may lose some pleasurable sensation as well as pain, which can affect arousal for some women.
- Partner Numbness: If not wiped off, it can transfer to your partner’s skin or mucous membranes.
- Allergic Reactions: Rare, but can include redness, swelling, or worsening burning. Stop use immediately if this occurs.
- Masking Underlying Issues: Numbing pain does not treat the root cause (e.g., oestrogen deficiency, infection, or nerve damage). Always seek a proper diagnosis.
Common Concerns & Myths
“Will using lidocaine make me dependent on it?”
No. Lidocaine does not cause physical dependence. However, relying solely on numbing without addressing the underlying cause can delay effective treatment. Think of it as a bridge, not a destination.
“Is it safe to use every time I have sex?”
Yes, for most women, occasional use before intimacy is safe. However, nightly or very frequent use should be discussed with a clinician, as it may indicate an underlying condition that needs active treatment rather than masking.
“Will it stop me from feeling pleasure?”
It may reduce sensation temporarily in the numbed area, but many women report that eliminating the sharp pain actually allows them to relax enough to feel pleasure elsewhere. Experiment with timing and amount to find the right balance.
Clinical Context
Provoked vestibulodynia (PVD) is one of the most common causes of painful sex in pre-menopausal women, though it can also affect those in perimenopause or post-menopause. The condition involves localised hypersensitivity of the vulvar vestibule, often triggered by touch, pressure, or friction. It can develop after childbirth, recurrent thrush infections, or hormonal changes, and is frequently associated with pelvic floor dysfunction. Topical lidocaine is endorsed by organisations including the International Society for the Study of Vulvovaginal Disease (ISSVD) as part of a multi-modal treatment approach. Educational only. Results vary. Not a cure.
Evidence-Based Approaches
Self-Care & Lifestyle
Alongside lidocaine, simple adjustments can help reduce vestibular irritation and support tissue health:
- Avoid Irritants: Stop using perfumed soaps, wipes, or douches. Wash the vulva with water only or a gentle, pH-balanced wash.
- Wear Breathable Underwear: Choose 100% cotton and avoid tight synthetic fabrics that trap moisture.
- Use Lubricant: Even with lidocaine, always use a generous amount of high-quality, body-safe lubricant to reduce friction.
- Ice Packs: Applying a wrapped ice pack to the vulva for 10 minutes after sex can reduce inflammation and soothe nerve endings.
Medical & Specialist Options
For persistent vestibular pain, a comprehensive treatment plan is essential. Options include:
- Topical Oestrogen: If tissue thinning (atrophy) is contributing to hypersensitivity, localised oestrogen creams or pessaries can restore thickness and elasticity.
- Pelvic Floor Physiotherapy: Specialist physios use internal manual therapy, dilators, and biofeedback to release muscle tension and desensitise the vestibule.
- Nerve Blocks or Injections: In severe cases, clinicians may offer pudendal nerve blocks or botulinum toxin injections to calm overactive nerves.
- Cognitive Behavioural Therapy (CBT): Addresses the fear-pain-avoidance cycle and helps rebuild intimacy confidence.
- Regenerative Treatments: Some clinics offer treatments such as platelet-rich plasma (PRP) or radiofrequency therapy to improve tissue health and nerve regulation.
To explore a structured pathway that combines these approaches, you can view our step-by-step treatment plan. If you are considering specialist care, you may also wish to book a consultation to discuss your symptoms in detail.
C. Red Flags (When to see a GP)
Seek medical review if you experience sudden onset of severe pain, visible sores or ulcers, persistent bleeding, unusual discharge with odour, or if the pain is accompanied by fever or systemic symptoms. These may indicate infection, dermatological conditions, or other pathology requiring investigation.
External Resources:
- NHS – Vulvodynia overview
- BNF – Lidocaine hydrochloride prescribing information
- RCOG – Vulval pain (vulvodynia) patient leaflet
- National Vulvodynia Association – Treatment overview
- PubMed – Randomised trial of topical lidocaine for vestibulodynia
- British Pain Society – Chronic pain management resources
Educational only. Results vary. Not a cure.
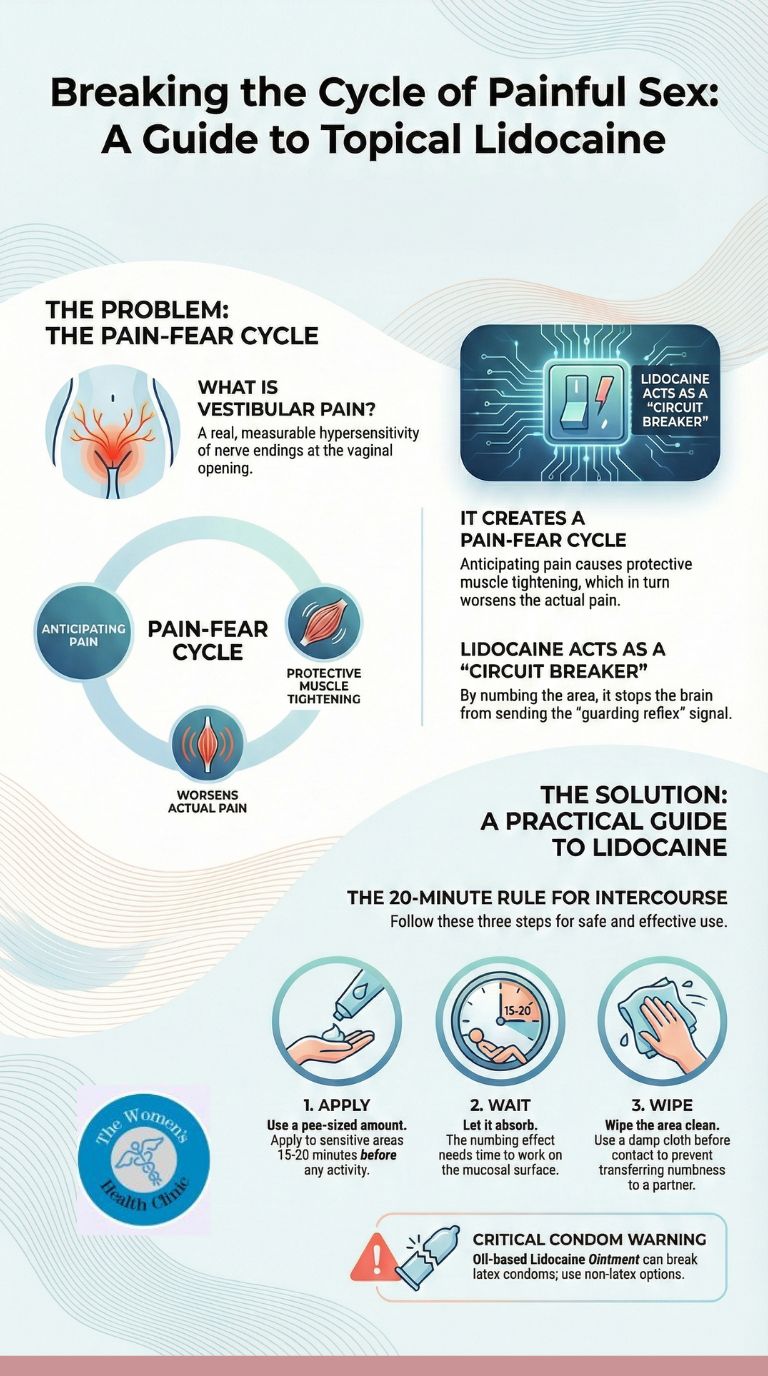
Clinical Protocol: Lidocaine can break the "Pain-Spasm" cycle, but timing is everything. To avoid numbing your partner, you must apply it 20 minutes before intimacy and wipe it off. For long-term nerve healing, the "Overnight Cotton Ball" technique is often more effective.
How to use Lidocaine safely
Lidocaine doesn't just mask pain; it prevents the Guarding Reflex. By numbing the entrance (vestibule), your brain doesn't receive the "sharp" signal, so it doesn't order the pelvic floor muscles to slam shut. This allows comfortable penetration.
Instructions for Intercourse
- Apply: Put a pea-sized amount of 5% Lidocaine Ointment on the sensitive areas (usually 5 and 7 o'clock) 15–20 minutes before activity.
- Wait: Let it absorb. It needs time to penetrate the mucosa.
- Wipe: Before any contact, wipe the area clean with a damp cloth. The skin is now numb, but the surface is clean. This prevents transferring the drug to your partner.
To treat the nerves long-term (not just for sex), we use "Desensitization."
- Technique: Soak a cotton ball in Lidocaine and place it against the vestibule (held by underwear) overnight for 6–8 weeks.
- Goal: This provides a continuous "quiet" signal to the nerves, helping to down-regulate the hypersensitivity (Allodynia) permanently.
MYTH: "Lidocaine is safe with all condoms."
REALITY: Lidocaine Ointment is usually oil-based (Vaseline base). Oil dissolves latex condoms, causing them to break. You must use polyurethane (non-latex) condoms or switch to a water-based Lidocaine Gel (though gels sting more).