Vaginal DHEA—who might consider it for sexual comfort?
Vaginal DHEA (prasterone) is a hormone therapy applied directly inside the vagina to treat moderate to severe dryness and pain during sex caused by low oestrogen after menopause. It is particularly suited to women who cannot or prefer not to use oestrogen-based treatments, or who have not fully responded to standard vaginal oestrogen. DHEA is converted locally into both oestrogen and testosterone, helping restore tissue thickness, lubrication, and sensitivity.
Show Detailed Answer
DHEA (dehydroepiandrosterone) is a naturally occurring hormone produced by the adrenal glands. Its levels decline sharply with age, particularly after menopause. Vaginal DHEA is inserted as a small pessary (usually 6.5mg nightly) and works directly in the vaginal tissue, where it is metabolised into active oestrogen and androgens. This dual action can improve not only the structure and moisture of vaginal tissue, but also sexual arousal and pleasure.
Unlike oral hormone replacement therapy (HRT), vaginal DHEA acts locally with minimal absorption into the bloodstream, making it a safer option for women with certain health histories. The treatment is licensed in the UK and Europe under the brand name Intrarosa, though availability through the NHS can vary by region.
Who Might Benefit from Vaginal DHEA?
Vaginal DHEA is specifically designed for postmenopausal women experiencing genitourinary syndrome of menopause (GSM), which includes symptoms such as:
- Vaginal dryness and atrophy: Thinning of vaginal walls, reduced elasticity, and loss of natural moisture.
- Dyspareunia (painful sex): Burning, tearing, or discomfort during or after penetration.
- Loss of libido or sensation: Reduced sexual desire or difficulty achieving arousal, possibly linked to low androgens.
- Urinary symptoms: Recurrent urinary tract infections (UTIs), urgency, or stress incontinence related to tissue changes.
When DHEA May Be Preferred Over Oestrogen
There are several clinical scenarios where vaginal DHEA might be considered instead of or alongside vaginal oestrogen:
- Incomplete response to oestrogen: Some women find that vaginal oestrogen improves dryness but does not fully restore sexual comfort or sensation. DHEA’s androgen activity may address this gap.
- History of oestrogen-sensitive conditions: Women with a past diagnosis of breast cancer or endometrial cancer may be advised to avoid even localised oestrogen. DHEA offers an alternative, though discussion with an oncologist is essential.
- Preference for non-oestrogen therapy: Some women simply prefer a treatment that does not contain oestrogen, whether for personal, medical, or psychological reasons.
- Concurrent systemic HRT: Women already taking oral or transdermal HRT may still experience vaginal symptoms and benefit from adding local DHEA.
How Quickly Does It Work?
Clinical trials show that most women notice improvement in vaginal dryness and pain within 2–4 weeks, with continued benefit over 12 weeks. Some women report enhanced sexual pleasure and arousal within a similar timeframe. Treatment is typically continued long-term, as symptoms can return if stopped.
Common Concerns & Myths
“Will DHEA increase my risk of breast cancer?”
Current evidence suggests that vaginal DHEA has minimal systemic absorption and does not significantly raise blood levels of oestrogen or testosterone. However, women with a history of hormone-sensitive cancers should always discuss risks and benefits with their oncology team before starting.
“Is it the same as testosterone therapy?”
Not quite. While DHEA is converted into testosterone locally, it also produces oestrogen. It is not the same as systemic testosterone replacement, which is used for different indications and administered differently.
“Can I use it if I’m still having periods?”
Vaginal DHEA is licensed only for postmenopausal women. If you are perimenopausal or still menstruating, other treatments such as vaginal oestrogen or lubricants are more appropriate first-line options.
Clinical Context
Vaginal DHEA was approved by the European Medicines Agency (EMA) in 2018 following robust clinical trials demonstrating its efficacy and safety. It is now available in the UK on private prescription and, in some areas, via NHS specialist menopause clinics. DHEA therapy is part of a broader shift towards personalised treatment for GSM, recognising that no single hormone suits every woman. It is particularly valuable for those who need both tissue restoration and improved sexual function. Educational only. Results vary. Not a cure.
Evidence-Based Approaches
Self-Care & Lifestyle
While DHEA is a prescription treatment, supporting vaginal health through lifestyle can enhance its effectiveness:
- Regular sexual activity: Gentle, regular vaginal stimulation (with or without a partner) helps maintain blood flow and tissue elasticity.
- Water-based lubricants: Continue using lubricants during sex to reduce friction, even as tissue health improves.
- Pelvic floor exercises: Gentle pelvic floor training can improve circulation and reduce pain, but avoid over-tightening if you have vaginismus or tension.
- Avoid irritants: Steer clear of perfumed soaps, douches, or wipes that can disrupt the vaginal microbiome.
Medical & Specialist Options
Vaginal DHEA is typically prescribed by GPs with a special interest in menopause, gynaecologists, or specialist menopause clinics. A typical regimen involves:
- Dosing: One 6.5mg pessary inserted nightly at bedtime, using the applicator provided.
- Monitoring: Initial follow-up at 3 months to assess symptom relief and tolerability, then annually.
- Combination therapy: DHEA can be used alongside systemic HRT, pelvic physiotherapy, or psychosexual counselling for a holistic approach.
- Alternative formulations: If DHEA is not suitable or available, vaginal oestrogen (e.g. Ovestin, Vagifem) or vaginal moisturisers remain excellent options.
If you are exploring treatment pathways, you may wish to explore treatment benefits or book a consultation with a specialist menopause clinician.
C. Red Flags (When to see a GP)
Seek urgent medical advice if you experience unexplained vaginal bleeding, severe pelvic pain, persistent discharge with odour, or any new lumps. These symptoms require investigation before starting or continuing hormonal therapy.
External Resources:
- NICE – Menopause: diagnosis and management (NG23)
- NHS – Hormone replacement therapy (HRT) overview
- RCOG – Vaginal dryness and menopause
- BNF – Prasterone (vaginal DHEA) prescribing guidance
- The Menopause Charity – Vaginal dryness and treatment options
- PubMed – Efficacy and safety of prasterone for vulvovaginal atrophy
Educational only. Results vary. Not a cure.
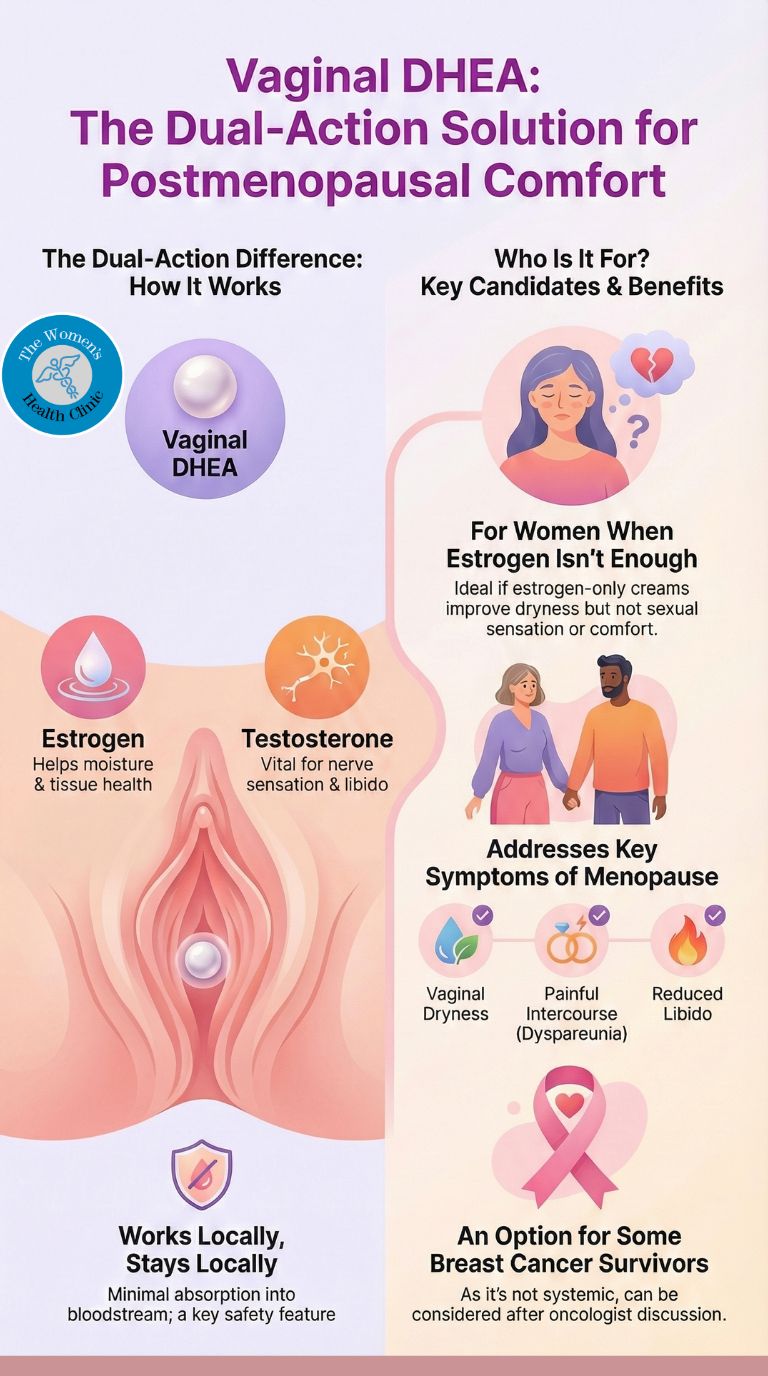
Clinical Insight: DHEA is not just a lubricant. It is a "Pro-Hormone" that your body converts into both Estrogen (for wetness) AND Testosterone (for nerve sensation) locally. This makes it a unique option for women experiencing "sexual numbness" or those restricted from systemic HRT.
Additional Clinical Context
Standard creams (like Vagifem or Ovestin) only replace Estrogen. However, healthy vaginal tissue requires both Estrogen and Testosterone to function.
The Testosterone Factor
- Sensation & Nerves: Estrogen plumps the tissue, but Testosterone is required to maintain nerve density. If you feel "lubricated but numb" or struggle to reach orgasm, the lack of local testosterone may be the cause.
- Intracrinology: DHEA (Prasterone) is inactive in the box. Once inserted, your vaginal cells ingest it and convert it into exactly the amount of Estrogen and Testosterone they need, strictly inside the cell.
Many women with a history of breast cancer are told to avoid HRT. However, local vaginal treatments are treated differently.
BMS & NAMS Position
- No Systemic Spike: Clinical trials confirm that daily use of vaginal DHEA maintains serum (blood) hormone levels within the normal "post-menopausal" range. It does not cause a systemic spike like oral HRT.
- The Guidelines: The British Menopause Society (BMS) and NICE suggest that local vaginal treatments can be considered for breast cancer survivors if non-hormonal lubricants fail, though this must always be discussed with your oncologist.
Switching to DHEA (Intrarosa) requires a different routine than standard Estrogen pessaries.
- Daily vs. Weekly: Unlike Vagifem (which is used twice weekly), DHEA is typically a daily treatment inserted at bedtime. It mimics the body's natural daily production.
- The "Waxy" Discharge: The DHEA molecule is suspended in a hard fat (Witepsol). As it melts, it often causes a white, creamy discharge the next morning. This is not Thrush. It is simply the carrier base leaving the body.
MYTH: "It's a hormone, so it will grow hair on my face."
REALITY: Because of "Intracrinology," the conversion to testosterone happens only inside the vaginal tissue. It is inactivated before it can travel to the rest of the body. You will not experience systemic side effects like voice deepening or hair growth.